Разделы презентаций
- Разное
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Геометрия
- Детские презентации
- Информатика
- История
- Литература
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
Chapter 23: The Respiratory System Biol 141 A & P
Содержание
- 1. Chapter 23: The Respiratory System Biol 141 A & P
- 2. The Respiratory SystemCells produce energy:for maintenance, growth,
- 3. OxygenIs obtained from the air by diffusion
- 4. 5 Functions of the Respiratory SystemProvides
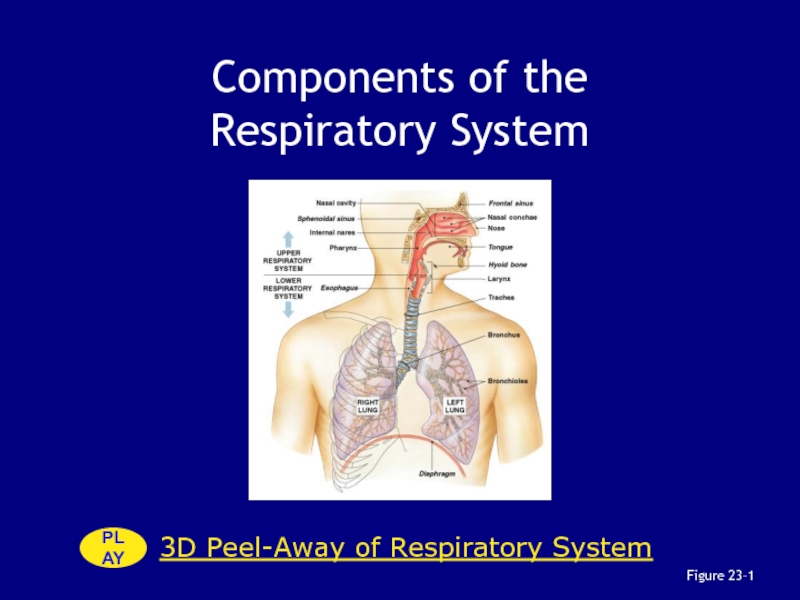
- 5. Components of the Respiratory SystemFigure 23–13D Peel-Away of Respiratory SystemPLAY
- 6. Organization of the Respiratory SystemThe respiratory
- 7. The Respiratory TractConsists of a conducting portion:from
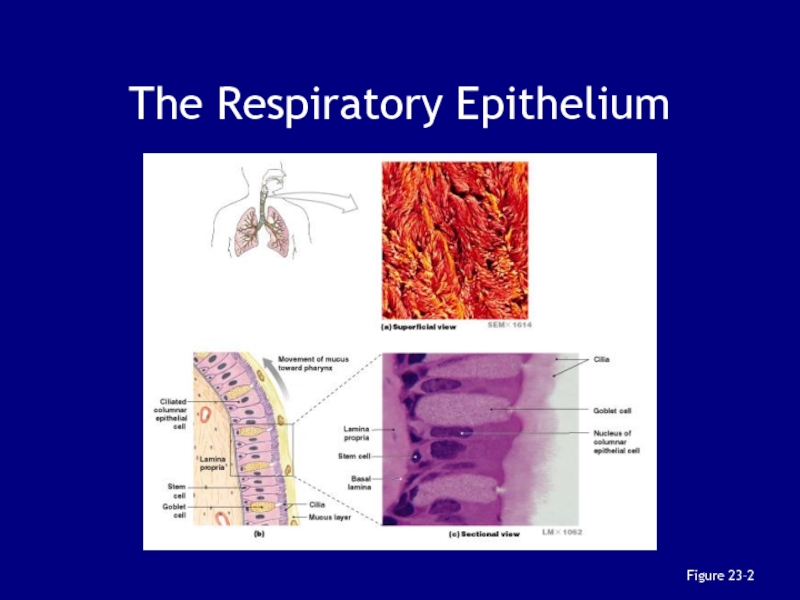
- 8. The Respiratory EpitheliumFigure 23–2
- 9. The Respiratory EpitheliumFor gases to exchange efficiently:alveoli
- 10. The Respiratory MucosaConsists of:an epithelial layeran areolar layerLines conducting portion of respiratory system
- 11. The Lamina PropriaUnderlies areolar tissueIn the upper
- 12. Structure of Respiratory EpitheliumChanges along respiratory
- 13. How are delicate respiratory exchange surfaces protected from pathogens, debris, and other hazards?
- 14. The Respiratory Defense System Consists of a
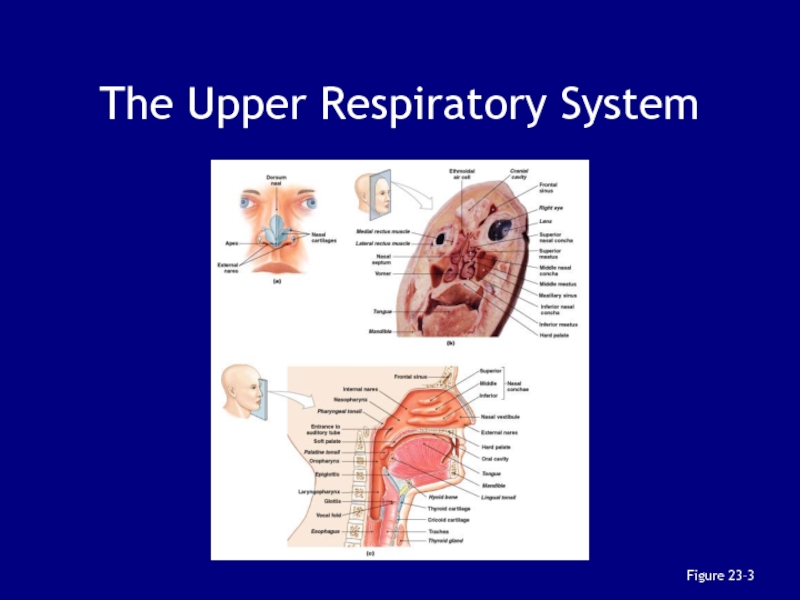
- 15. The Upper Respiratory SystemFigure 23–3
- 16. The Nose Air enters the respiratory system:through
- 17. The Nasal CavityThe nasal septum:divides nasal cavity
- 18. Air FlowFrom vestibule to internal nares:through superior,
- 19. The PalatesHard palate:forms floor of nasal cavityseparates
- 20. Air FlowNasal cavity opens into nasopharynx through
- 21. The Pharynx and DivisionsA chamber shared by
- 22. The Nasopharynx Superior portion of the pharynxContains
- 23. What is the structure of the
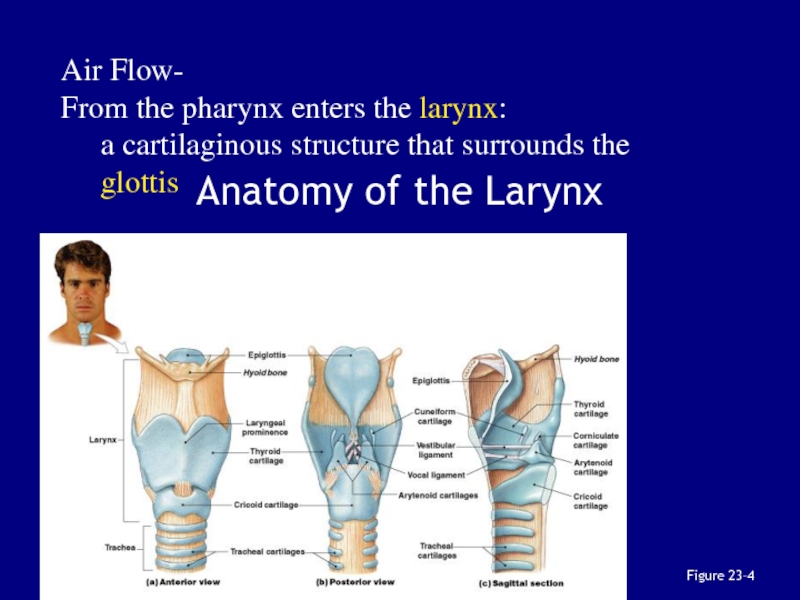
- 24. Anatomy of the LarynxFigure 23–4Air Flow-From the
- 25. Cartilages of the Larynx3 large, unpaired cartilages form the larynx:the thyroid cartilage the cricoid cartilagethe epiglottis
- 26. The Thyroid Cartilage Also called the Adam’s
- 27. The Cricoid CartilageIs a hyaline cartilageForm posterior
- 28. Cartilage FunctionsThyroid and cricoid cartilages support and
- 29. The GlottisFigure 23–5 3 pairs of Small Hyaline Cartilages of the Larynxarytenoid cartilages, corniculate cartilagescuneiform cartilages
- 30. Cartilage FunctionsCorniculate and arytenoid cartilages function in:opening and closing of glottisproduction of sound
- 31. Ligaments of the LarynxVestibular ligaments and vocal
- 32. Sound ProductionAir passing through glottis:vibrates vocal foldsproduces
- 33. SpeechIs produced by:phonation:sound production at the larynxarticulation:modification of sound by other structures
- 34. The Laryngeal MusculatureThe larynx is associated with:muscles
- 35. Anatomy of the TracheaFigure 23–6What is the structure of airways outside the lungs?
- 36. The Trachea Also called the windpipeExtends from
- 37. The Tracheal Cartilages 15–20 tracheal cartilages:strengthen and
- 38. The Primary BronchiRight and left primary bronchi:separated
- 39. Structure of Primary BronchiEach primary bronchus:travels to
- 40. The Root of the LungComplex of connective
- 41. Figure 23–7Gross Anatomy of the LungsLeft and
- 42. Lobes of the LungsLungs have lobes separated
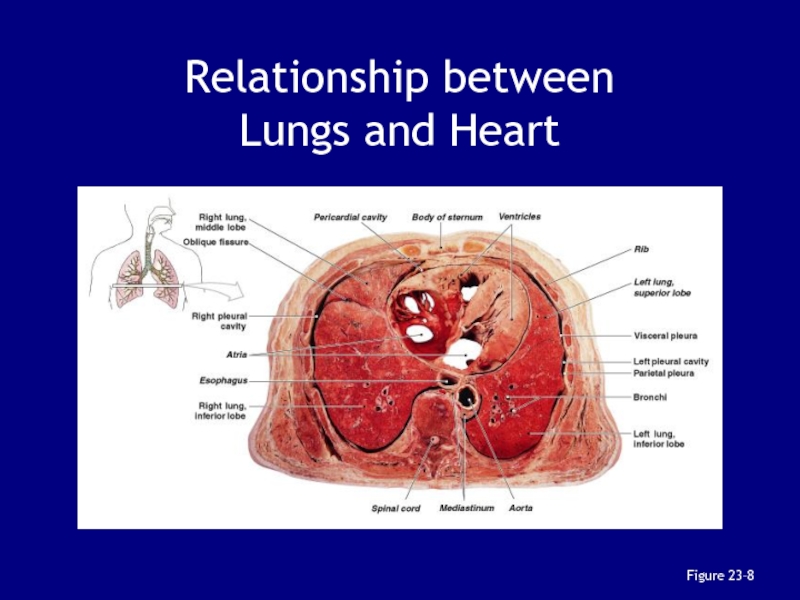
- 43. Relationship between Lungs and HeartFigure 23–8
- 44. Lung ShapeRight lung:is wider is displaced upward
- 45. The Bronchial TreeIs formed by the primary
- 46. Bronchi and LobulesFigure 23–9A Primary BronchusBranches to
- 47. Secondary Bronchi Branch to form tertiary bronchi,
- 48. Bronchial StructureThe walls of primary, secondary, and
- 49. Figure 23–10The BronchiolesBronchitis: Inflammation of bronchial walls: causes constriction and breathing difficulty
- 50. The BronchiolesEach tertiary bronchus branches into multiple
- 51. Bronchiole StructureBronchioles:have no cartilageare dominated by smooth
- 52. BronchodilationDilation of bronchial airwaysCaused by sympathetic ANS
- 53. AsthmaExcessive stimulation and bronchoconstriction Stimulation severely restricts airflow
- 54. Pulmonary LobulesAre the smallest compartments of the
- 55. Exchange SurfacesWithin the lobule:each terminal bronchiole branches
- 56. Figure 23–11Alveolar OrganizationRespiratory bronchioles are connected to
- 57. An AlveolusHas an extensive network of capillariesIs
- 58. Respiratory DistressDifficult respiration:due to alveolar collapse caused when septal cells do not produce enough surfactant
- 59. Respiratory Membrane - The thin membrane of
- 60. Inflammation of Lobules Also called pneumonia:causes fluid to leak into alveolicompromises function of respiratory membrane
- 61. Blood Supply to Respiratory SurfacesEach lobule
- 62. Blood Supply to the Lungs Capillaries supplied
- 63. Blood Pressure In pulmonary circuit is low
- 64. Figure 23–8Pleural Cavities and Pleural Membranes
- 65. Pleural Cavities and Pleural Membranes2 pleural
- 66. RespirationRefers to 2 integrated processes: External respiration-Includes
- 67. 3 Processes of External Respiration Pulmonary
- 68. What physical principles govern the movement of air into the lungs?
- 69. Pulmonary VentilationIs the physical movement of air
- 70. Gas Pressure and VolumeFigure 23–13Atmospheric PressureThe weight of air:has several important physiological effects
- 71. Boyle’s Law Defines the relationship between gas
- 72. Respiration: Pressure GradientsPLAYFigure 23–14Mechanisms of Pulmonary
- 73. A Respiratory CycleConsists of: an inspiration (inhalation)an
- 74. Compliance of the Lung An indicator of
- 75. Pressure and Volume Changes with Inhalation and
- 76. Intrapulmonary Pressure Also called intra-alveolar pressureIs relative
- 77. Maximum Intrapulmonary Pressure Maximum straining, a
- 78. Intrapleural Pressure Pressure in space between parietal
- 79. The Respiratory PumpCyclical changes in intrapleural pressure
- 80. Injury to the Chest WallPneumothorax:allows air into pleural cavityAtelectasis:also called a collapsed lungresult of pneumothorax
- 81. What are the origins and actions of the respiratory muscles responsible for respiratory movements?
- 82. Figure 23–16a, bThe Respiratory MusclesMost important are:the
- 83. The Respiratory MusclesFigure 23–16c, d
- 84. The Mechanics of BreathingInhalation:always activeExhalation:active or passive
- 85. 3 Muscle Groups of Inhalation Diaphragm:contraction draws
- 86. Muscles of Active Exhalation Internal intercostal and
- 87. Modes of BreathingRespiratory movements are classified:by pattern of muscle activityinto quiet breathing and forced breathing
- 88. Quiet Breathing (Eupnea) Involves active inhalation and
- 89. Forced Breathing Also called hyperpnea Involves active
- 90. Respiratory Rates and VolumesRespiratory system adapts to
- 91. Respiratory Minute VolumeAmount of air moved per
- 92. Alveolar Ventilation Amount of air reaching alveoli
- 93. Alveolar Ventilation RateDetermined by respiratory rate and
- 94. Respiratory Volumes and CapacitiesFigure 23–17
- 95. Lung VolumeTotal lung volume is divided into
- 96. 4 Pulmonary Volumes Resting tidal volume:in a
- 97. 4 Calculated Respiratory Capacities Inspiratory capacity:
- 98. Gas ExchangeOccurs between blood and alveolar airAcross
- 99. The Gas LawsDiffusion occurs in response to
- 100. Composition of AirNitrogen (N2) about 78.6%Oxygen (O2)
- 101. Gas PressureAtmospheric pressure (760 mm Hg):produced by
- 102. Partial Pressure The pressure contributed by each
- 103. Henry’s LawFigure 23–18When gas under pressure comes
- 104. Gas Content & Solubility in body
- 105. Diffusion and the Respiratory MembraneDirection and
- 106. Efficiency of Gas ExchangeDue to:– substantial differences
- 107. Respiratory Processes and Partial PressureFigure 23–19An
- 108. O2 and CO2Blood arriving in pulmonary arteries
- 109. Respiration: Gas Mixture in AirPLAYMixingOxygenated blood mixes
- 110. Interstitial Fluid PO2 40 mm Hg PCO2
- 111. How is oxygen picked up, transported,
- 112. Gas Pickup and DeliveryBlood plasma can’t transport
- 113. Oxygen TransportO2 binds to iron ions in
- 114. Oxyhemoglobin Saturation CurveFigure 23–20 (Navigator)Environmental Factors Affecting HemoglobinPO2 of blood, Blood pH, TemperatureMetabolic activity within RBCs
- 115. Oxyhemoglobin Saturation CurveIs a graph relating the
- 116. Oxygen ReservesO2 diffuses:from peripheral capillaries (high PO2)into
- 117. Figure 23–21pH, Temperature, and Hemoglobin Saturation
- 118. The Oxyhemoglobin Saturation Curve Is standardized
- 119. The Bohr EffectIs the effect of pH
- 120. 2,3-biphosphoglycerate (BPG) RBCs generate ATP by glycolysis:forming
- 121. Fetal and Adult HemoglobinFigure 23–22
- 122. Fetal and Adult HemoglobinThe structure of fetal
- 123. KEY CONCEPTHemoglobin in RBCs:carries most blood oxygenreleases
- 124. How is carbon dioxide transported in the
- 125. Carbon Dioxide (CO2) Is generated as a
- 126. CO2 in the Blood Stream70% is transported
- 127. KEY CONCEPTCO2 travels in the bloodstream primarily
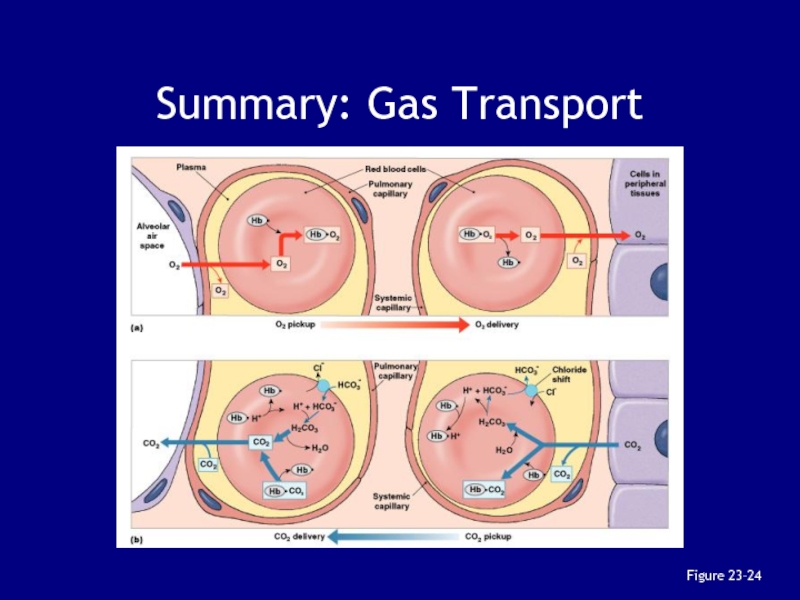
- 128. Summary: Gas TransportFigure 23–24
- 129. InterActive Physiology: Respiratory System: Control of RespirationPLAYControl
- 130. Local Regulation of O2 Transport (1
- 131. Respiratory Centers of the BrainWhen oxygen demand
- 132. Voluntary CentersIn cerebral cortex affect:respiratory centers of
- 133. Respiratory Rhythmicity Centers of the Medulla Oblongata
- 134. Figure 23–25aQuiet BreathingBrief activity in the DRG:stimulates inspiratory musclesDRG neurons become inactive:allowing passive exhalation
- 135. Figure 23–25bForced BreathingIncreased activity in DRG:stimulates VRGwhich
- 136. The Apneustic and Pneumotaxic Centers of
- 137. Respiratory Centers and Reflex ControlsFigure 23–26Interactions
- 138. SIDS Also known as sudden infant death
- 139. 5 Sensory Modifiers of Respiratory Center ActivitiesChemoreceptors
- 140. 5 Sensory Modifiers of Respiratory Center ActivitiesStretch
- 141. Chemoreceptor ReflexesRespiratory centers are strongly influenced by
- 142. Chemoreceptor Responses to PCO2Figure 23–27
- 143. Hypercapnia- An increase in arterial
- 144. Baroreceptor ReflexesCarotid and aortic baroreceptor stimulation:affects blood
- 145. Protective Reflexes Triggered by receptors in epithelium
- 146. Apnea A period of suspended respirationNormally followed
- 147. The Cerebral Cortex and Respiratory CentersStrong emotions:can
- 148. KEY CONCEPTSA basic pace of respiration is
- 149. Changes in Respiratory System at Birth
- 150. Changes in Respiratory System at Birth
- 151. Respiratory Performance and AgeFigure 23–28
- 152. 3 Effects of Aging on the
- 153. Integration with Other SystemsMaintaining homeostatic O2 and
- 154. Coordination of Respiratory and Cardiovascular SystemsImproves
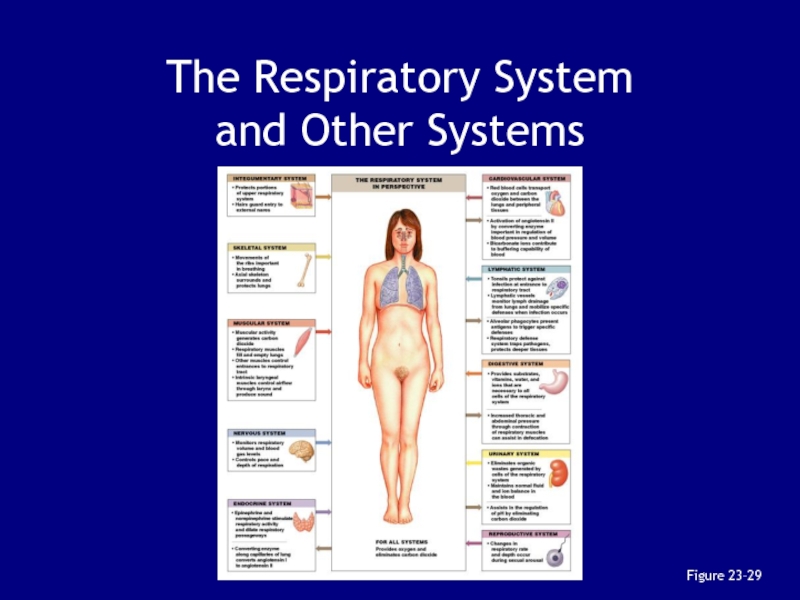
- 155. Figure 23–29The Respiratory System and Other Systems
- 156. SUMMARY (1 of 4)5 functions of the
- 157. SUMMARY (2 of 4)Structures and functions of
- 158. SUMMARY (3 of 4)Structures and functions of
- 159. SUMMARY (4 of 4)Gas exchange:the gas lawsdiffusion
- 160. Скачать презентанцию
Слайды и текст этой презентации
Слайд 2The Respiratory System
Cells produce energy:
for maintenance, growth, defense, and division
through
mechanisms that use oxygen and produce carbon dioxide
Слайд 3Oxygen
Is obtained from the air by diffusion across delicate exchange
surfaces of lungs
Is carried to cells by the cardiovascular system
which also returns carbon dioxide to the lungs 3D Movie of Respiratory System
PLAY
Слайд 45 Functions of the
Respiratory System
Provides extensive gas exchange surface
area between air and circulating blood
Moves air to and from
exchange surfaces of lungsProtects respiratory surfaces from outside environment
Produces sounds
Participates in olfactory sense
Слайд 6Organization of the
Respiratory System
The respiratory system is divided into
the upper respiratory system, above the larynx, and the lower
respiratory system, from the larynx downСлайд 7The Respiratory Tract
Consists of a conducting portion:
from nasal cavity to
terminal bronchioles
Consists of a respiratory portion:
the respiratory bronchioles and alveoli
Alveoli
Are air-filled pockets within the lungs
where all gas exchange takes place
The Respiratory Tract
PLAY
Слайд 9The Respiratory Epithelium
For gases to exchange efficiently:
alveoli walls must be
very thin (< 1 µm)
surface area must be very
great (about 35 times the surface area of the body)Слайд 10The Respiratory Mucosa
Consists of:
an epithelial layer
an areolar layer
Lines conducting portion
of respiratory system
Слайд 11The Lamina Propria
Underlies areolar tissue
In the upper respiratory system, trachea,
and bronchi:
contains mucous glands that secrete onto epithelial surface
In the
conducting portion of lower respiratory system:contains smooth muscle cells that encircle lumen of bronchioles
Слайд 12Structure of
Respiratory Epithelium
Changes along respiratory tract
Alveolar Epithelium
Is a very
delicate, simple squamous epithelium
Contains scattered and specialized cells
Lines exchange surfaces
of alveoliСлайд 13How are delicate respiratory exchange surfaces protected from pathogens, debris,
and other hazards?
Слайд 14The Respiratory Defense System
Consists of a series of filtration
mechanisms
Removes particles and pathogens
* Components of the Respiratory
Defense SystemGoblet cells and mucous glands: produce mucus that bathes exposed surfaces
Cilia: sweep debris trapped in mucus toward the pharynx (mucus escalator)
Filtration in nasal cavity removes large particles
Alveolar macrophages engulf small particles that reach lungs
Слайд 16The Nose
Air enters the respiratory system:
through nostrils or external
nares
into nasal vestibule
Nasal hairs:
are in nasal vestibule
are the
first particle filtration systemСлайд 17The Nasal Cavity
The nasal septum:
divides nasal cavity into left and
right
Mucous secretions from paranasal sinus and tears:
clean and moisten the
nasal cavitySuperior portion of nasal cavity is the olfactory region:
provides sense of smell
Слайд 18Air Flow
From vestibule to internal nares:
through superior, middle, and inferior
meatuses
Meatuses
Constricted passageways that produce air turbulence:
warm and humidify incoming air
trap
particlesСлайд 19The Palates
Hard palate:
forms floor of nasal cavity
separates nasal and oral
cavities
Soft palate:
extends posterior to hard palate
divides superior nasopharynx from lower
pharynxСлайд 20Air Flow
Nasal cavity opens into nasopharynx through internal nares
The Nasal
Mucosa
Warm and humidify inhaled air for arrival at lower respiratory
organs Breathing through mouth bypasses this important step
Слайд 21The Pharynx and Divisions
A chamber shared by digestive and respiratory
systems
Extends from internal nares to entrances to larynx and esophagus
Nasopharynx
Oropharynx
Laryngopharynx
Слайд 22The Nasopharynx
Superior portion of the pharynx
Contains pharyngeal tonsils and
openings to left and right auditory tubes
The Oropharynx
Middle portion of
the pharynxCommunicates with oral cavity
The Laryngopharynx
Inferior portion of the pharynx
Extends from hyoid bone to entrance to larynx and esophagus
Слайд 23What is the structure of the larynx and its role
in normal breathing
and production of sound?
Слайд 24Anatomy of the Larynx
Figure 23–4
Air Flow-
From the pharynx enters the
larynx:
a cartilaginous structure that surrounds the glottis
Слайд 25Cartilages of the Larynx
3 large, unpaired cartilages form the larynx:
the
thyroid cartilage
the cricoid cartilage
the epiglottis
Слайд 26The Thyroid Cartilage
Also called the Adam’s apple
Is a hyaline
cartilage
Forms anterior and lateral walls of larynx
Ligaments attach to hyoid
bone, epiglottis, and laryngeal cartilagesСлайд 27The Cricoid Cartilage
Is a hyaline cartilage
Form posterior portion of larynx
Ligaments
attach to first tracheal cartilage
Articulates with arytenoid cartilages
The Epiglottis
Composed of
elastic cartilageLigaments attach to thyroid cartilage and hyoid bone
Слайд 28Cartilage Functions
Thyroid and cricoid cartilages support and protect:
the glottis
the
entrance to trachea
During swallowing:
the larynx is elevated
the epiglottis folds back
over glottisPrevents entry of food and liquids into respiratory tract
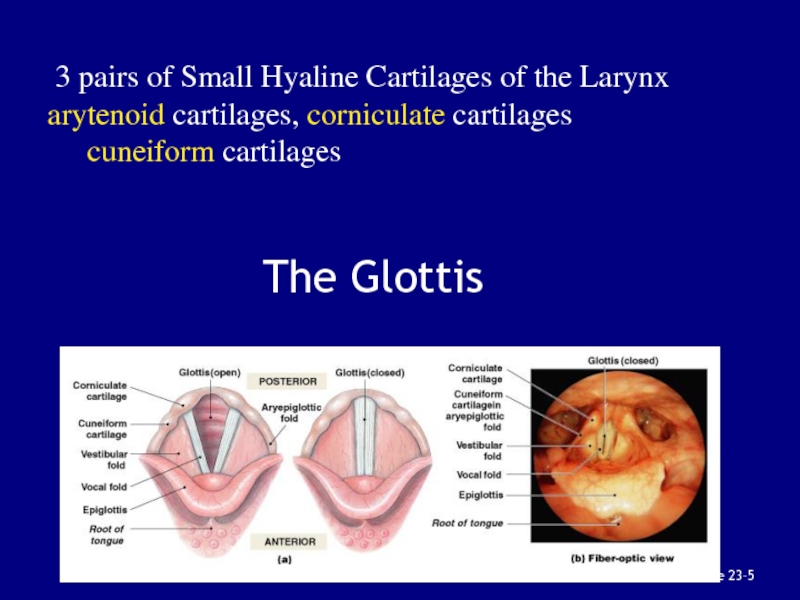
Слайд 29The Glottis
Figure 23–5
3 pairs of Small Hyaline Cartilages of
the Larynx
arytenoid cartilages, corniculate cartilages
cuneiform cartilages
Слайд 30Cartilage Functions
Corniculate and arytenoid cartilages function in:
opening and closing of
glottis
production of sound
Слайд 31Ligaments of the Larynx
Vestibular ligaments and vocal ligaments:
extend between thyroid
cartilage and arytenoid cartilages
are covered by folds of laryngeal epithelium
that project into glottis1) The Vestibular Ligaments
Lie within vestibular folds:
which protect delicate vocal folds
Слайд 32Sound Production
Air passing through glottis:
vibrates vocal folds
produces sound waves
Sound Variation
Sound is varied by:
tension on vocal folds: slender and
short =high pitched, thicker and longer = low pitchedvoluntary muscles (position arytenoid cartilage relative to thyroid cartilage)
Слайд 33Speech
Is produced by:
phonation:
sound production at the larynx
articulation:
modification of sound by
other structures
Слайд 34The Laryngeal Musculature
The larynx is associated with:
muscles of neck and
pharynx
intrinsic muscles that:
control vocal folds
open and close glottis
Coughing reflex: food
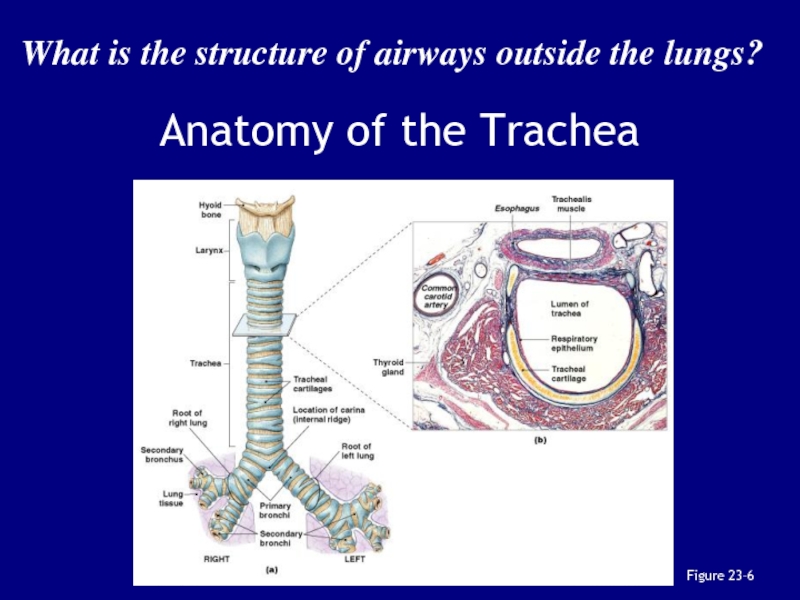
or liquids went “down the wrong pipe”Слайд 36The Trachea
Also called the windpipe
Extends from the cricoid cartilage
into mediastinum
where it branches into right and left pulmonary bronchi
The
SubmucosaBeneath mucosa of trachea
Contains mucous glands
Слайд 37The Tracheal Cartilages
15–20 tracheal cartilages:
strengthen and protect airway
discontinuous where
trachea contacts esophagus
Ends of each tracheal cartilage are connected by:
an
elastic ligament and trachealis muscle Слайд 38The Primary Bronchi
Right and left primary bronchi:
separated by an internal
ridge (the carina)
1) The Right Primary Bronchus
Is larger in diameter
than the leftDescends at a steeper angle
Слайд 39Structure of Primary Bronchi
Each primary bronchus:
travels to a groove (hilus)
along medial surface of the lung
Hilus-Where pulmonary nerves, blood vessels, and lymphatics enter lung
Anchored in meshwork of connective tissue
Слайд 40The Root of the Lung
Complex of connective tissues, nerves, and
vessels in hilus:
anchored to the mediastinum
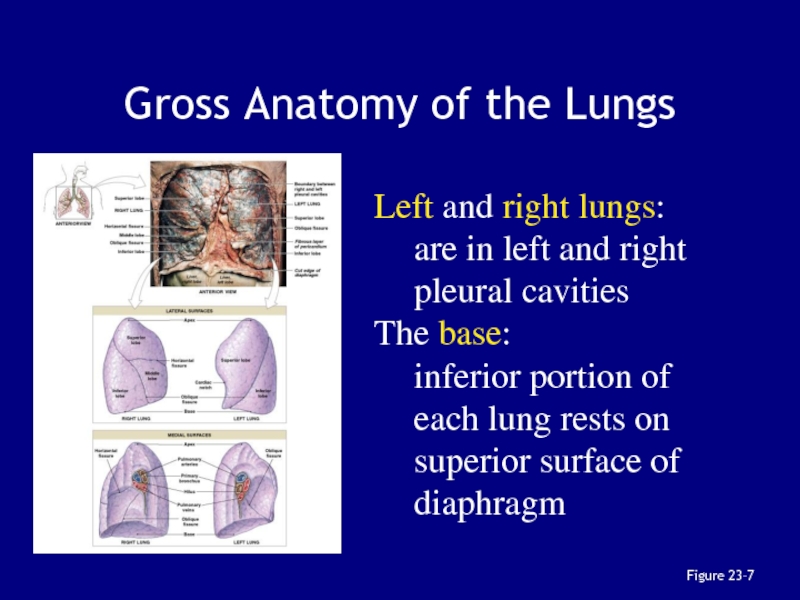
Слайд 41Figure 23–7
Gross Anatomy of the Lungs
Left and right lungs:
are in
left and right pleural cavities
The base:
inferior portion of each lung
rests on superior surface of diaphragmСлайд 42Lobes of the Lungs
Lungs have lobes separated by deep fissures
1) The Right Lung- Has 3 lobes:
superior, middle,
and inferiorseparated by horizontal and oblique fissures
2) The Left Lung- Has 2 lobes:
superior and inferior
are separated by an oblique fissure
Слайд 44Lung Shape
Right lung:
is wider
is displaced upward by liver
Left lung:
is
longer
is displaced leftward by the heart forming the cardiac
notch Слайд 45The Bronchial Tree
Is formed by the primary bronchi and their
branches
Extrapulmonary Bronchi
The left and right bronchi branches outside the lungs
Intrapulmonary Bronchi
Branches within the lungs
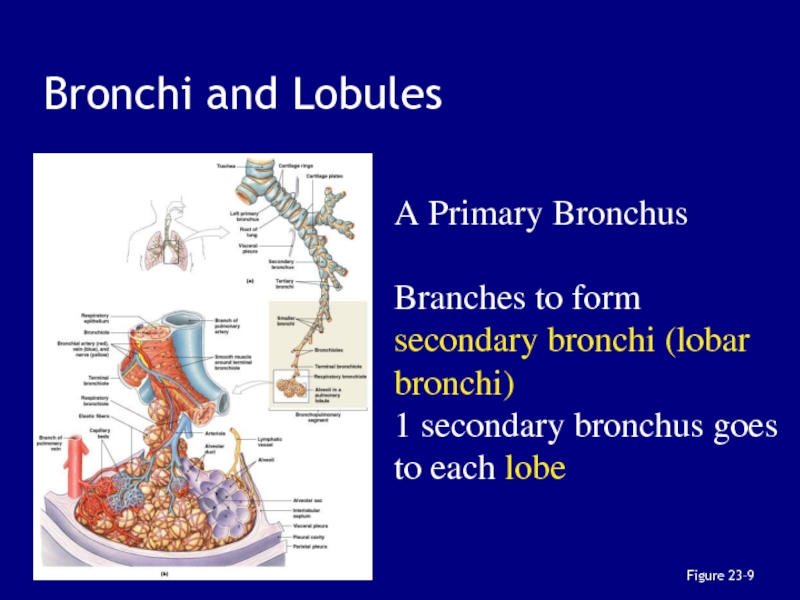
Слайд 46Bronchi and Lobules
Figure 23–9
A Primary Bronchus
Branches to form secondary bronchi
(lobar bronchi)
1 secondary bronchus goes to each lobe
Слайд 47Secondary Bronchi
Branch to form tertiary bronchi, also called the
segmental bronchi
Each segmental bronchus:
supplies air to a single bronchopulmonary segment-
The
right lung has 10The left lung has 8 or 9
Слайд 48Bronchial Structure
The walls of primary, secondary, and tertiary bronchi:
contain progressively
less cartilage and more smooth muscle
increasing muscular effects on airway
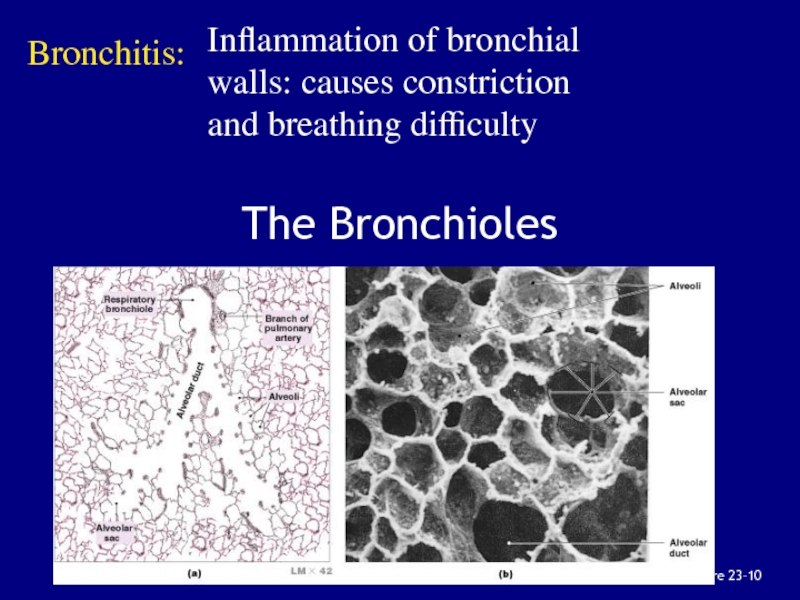
constriction and resistance Слайд 49Figure 23–10
The Bronchioles
Bronchitis:
Inflammation of bronchial walls: causes constriction and
breathing difficulty
Слайд 50The Bronchioles
Each tertiary bronchus branches into multiple bronchioles
Bronchioles branch into
terminal bronchioles:
1 tertiary bronchus forms about 6500 terminal bronchioles
Слайд 51Bronchiole Structure
Bronchioles:
have no cartilage
are dominated by smooth muscle
Autonomic Control
Regulates smooth muscle:
controls diameter of bronchioles
controls airflow and resistance
in lungsСлайд 52Bronchodilation
Dilation of bronchial airways
Caused by sympathetic ANS activation
Reduces resistance
Bronchoconstriction
Constricts bronchi
Caused
by: parasympathetic ANS activation
histamine release (allergic reactions)
Слайд 54Pulmonary Lobules
Are the smallest compartments of the lung
Are divided by
the smallest trabecular partitions (interlobular septa)
Each terminal bronchiole delivers
air to a single pulmonary lobuleEach pulmonary lobule is supplied by pulmonary arteries and veins
Слайд 55Exchange Surfaces
Within the lobule:
each terminal bronchiole branches to form several
respiratory bronchioles, where gas exchange takes place
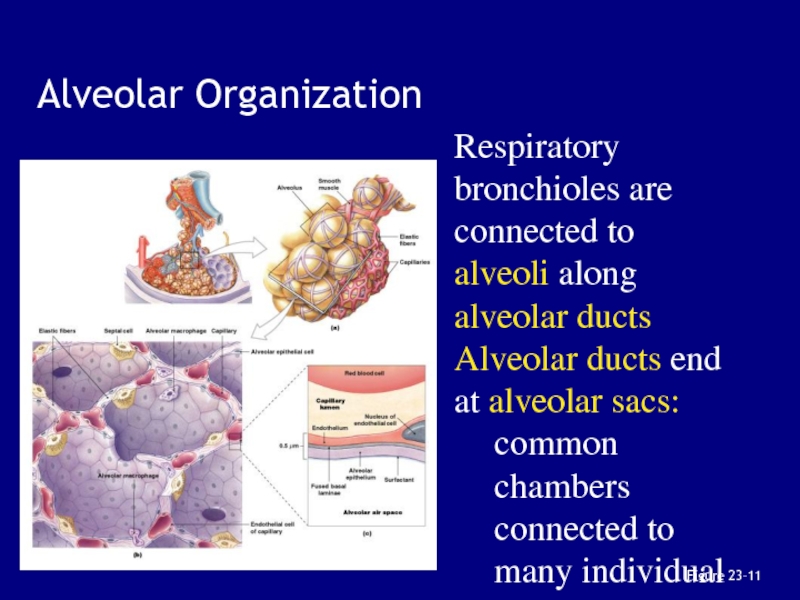
Слайд 56Figure 23–11
Alveolar Organization
Respiratory bronchioles are connected to alveoli along alveolar
ducts
Alveolar ducts end at alveolar sacs:
common chambers connected to
many individual alveoli Слайд 57An Alveolus
Has an extensive network of capillaries
Is surrounded by elastic
fibers
Alveolar Epithelium
Consists
of simple squamous epitheliumConsists of thin, delicate Type I cells
Patrolled by alveolar macrophages, also called dust cells
Contains septal cells (Type II cells) that produce Surfactant- an oily secretion which
1) Contains phospholipids and proteins
2) Coats alveolar surfaces and reduces surface tension
Слайд 58Respiratory Distress
Difficult respiration:
due to alveolar collapse
caused when septal cells
do not produce enough surfactant
Слайд 59Respiratory Membrane - The thin membrane of alveoli where gas
exchange takes place
3 Parts of the
Respiratory Membrane Squamous epithelial lining of alveolus
Endothelial cells lining an adjacent capillary
Fused basal laminae between alveolar and endothelial cells
Diffusion- Across respiratory membrane is very rapid:
because distance is small
gases (O2 and CO2) are lipid soluble
Слайд 60Inflammation of Lobules
Also called pneumonia:
causes fluid to leak into
alveoli
compromises function of respiratory membrane
Слайд 61Blood Supply to
Respiratory Surfaces
Each lobule receives an arteriole and
a venule
respiratory exchange surfaces receive blood:
from arteries of pulmonary circuit
a
capillary network surrounds each alveolus:as part of the respiratory membrane
blood from alveolar capillaries:
passes through pulmonary venules and veins
returns to left atrium
Слайд 62Blood Supply to the Lungs
Capillaries supplied by bronchial arteries:
provide
oxygen and nutrients to tissues of conducting passageways of lung
Venous blood bypasses the systemic circuit and flows into pulmonary veins
Слайд 63Blood Pressure
In pulmonary circuit is low (30 mm Hg)
Pulmonary
vessels are easily blocked by blood clots, fat, or air
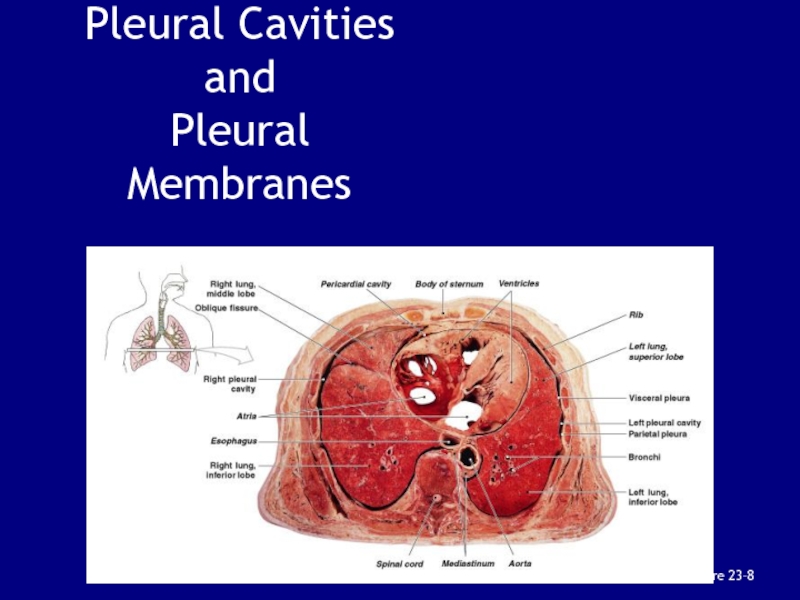
bubbles, causing pulmonary embolismСлайд 65Pleural Cavities and
Pleural Membranes
2 pleural cavities:
are separated by the
mediastinum
Each pleural cavity:
holds a lung
is lined with a serous
membrane (the pleura)Pleura consist of 2 layers:
parietal pleura
visceral pleura
Pleural fluid:
lubricates space between 2 layers
Слайд 66Respiration
Refers to 2 integrated processes:
External respiration-Includes all processes involved
in exchanging O2 and CO2 with the environment
Internal respiration-
Also called cellular respirationInvolves the uptake of O2 and production of CO2 within individual cells
Слайд 673 Processes of
External Respiration
Pulmonary ventilation (breathing)
Gas diffusion:
across membranes
and capillaries
Transport of O2 and CO2:
between alveolar capillaries
between capillary beds
in other tissuesСлайд 69Pulmonary Ventilation
Is the physical movement of air in and out
of respiratory tract
Provides alveolar ventilation
InterActive Physiology: Respiratory System: Anatomy Review:
Respiratory StructuresPLAY
Слайд 70Gas Pressure and Volume
Figure 23–13
Atmospheric Pressure
The weight of air:
has several
important physiological effects
Слайд 71Boyle’s Law
Defines the relationship between gas pressure and volume:
P = 1/V
In a contained gas:
external pressure forces molecules closer
togethermovement of gas molecules exerts pressure on container
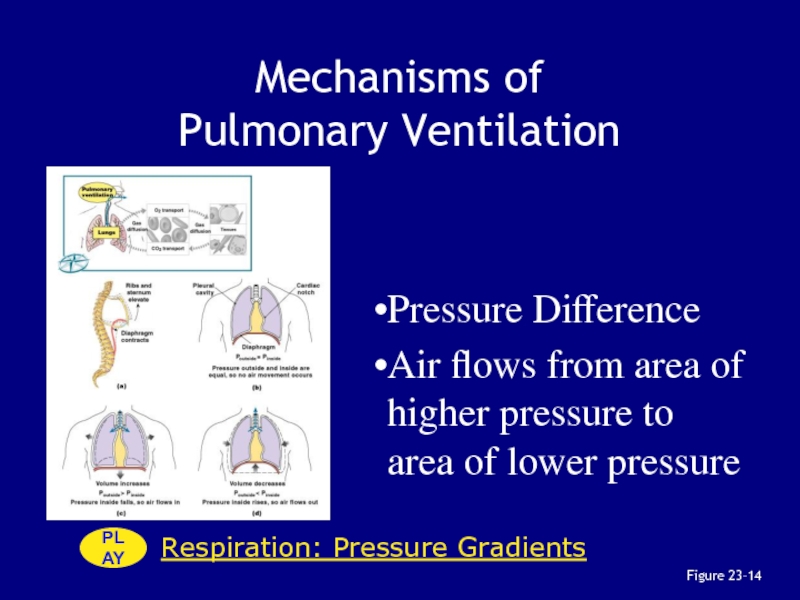
Слайд 72Respiration: Pressure Gradients
PLAY
Figure 23–14
Mechanisms of
Pulmonary Ventilation
Pressure Difference
Air flows from
area of higher pressure to area of lower pressure
Слайд 73A Respiratory Cycle
Consists of:
an inspiration (inhalation)
an expiration (exhalation)
Respiration
Causes volume changes that create changes in pressure
Volume
of thoracic cavity changes:with expansion or contraction of diaphragm or rib cage
Слайд 74Compliance of the Lung
An indicator of expandability
Low compliance requires
greater force
High compliance requires less force
Factors
That Affect ComplianceConnective-tissue structure of the lungs
Level of surfactant production
Mobility of the thoracic cage
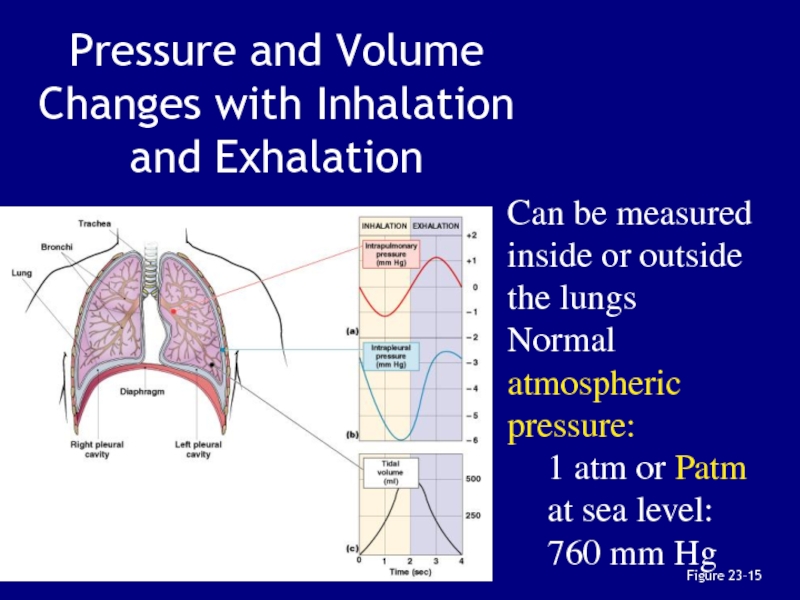
Слайд 75Pressure and Volume Changes with Inhalation and Exhalation
Figure 23–15
Can
be measured inside or outside the lungs
Normal atmospheric pressure:
1
atm or Patm at sea level: 760 mm HgСлайд 76Intrapulmonary Pressure
Also called intra-alveolar pressure
Is relative to Patm
In relaxed
breathing, the difference between Patm and intrapulmonary pressure is small:
about
—1 mm Hg on inhalation or +1 mm Hg on expiration Слайд 77Maximum
Intrapulmonary Pressure
Maximum straining, a dangerous activity, can increase
range:
from —30 mm Hg to +100 mm Hg
Слайд 78Intrapleural Pressure
Pressure in space between parietal and visceral pleura
Averages —4 mm Hg
Maximum of —18 mm Hg
Remains below Patm
throughout respiratory cycle Слайд 79The Respiratory Pump
Cyclical changes in intrapleural pressure operate the respiratory
pump:
which aids in venous return to heart
Tidal Volume
Amount of air
moved in and out of lungs in a single respiratory cycle Слайд 80Injury to the Chest Wall
Pneumothorax:
allows air into pleural cavity
Atelectasis:
also called
a collapsed lung
result of pneumothorax
Слайд 81What are the origins and actions of the respiratory muscles
responsible for respiratory movements?
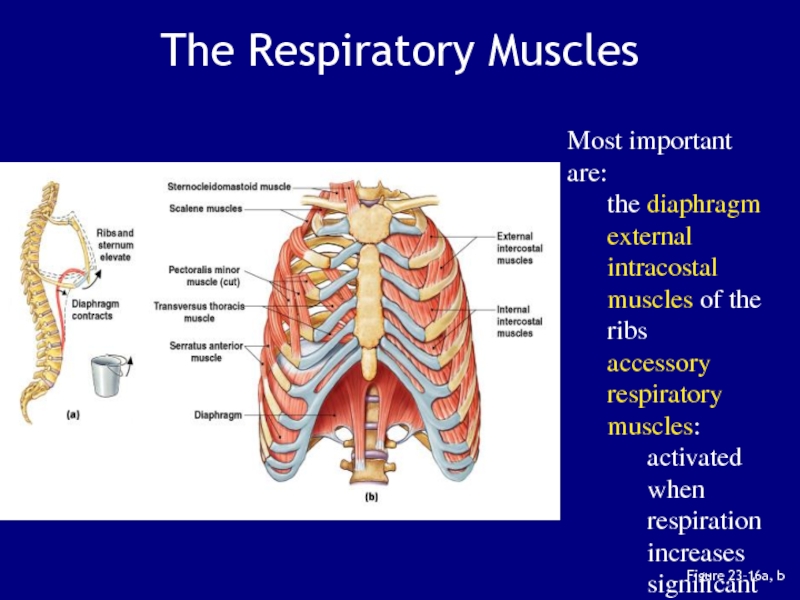
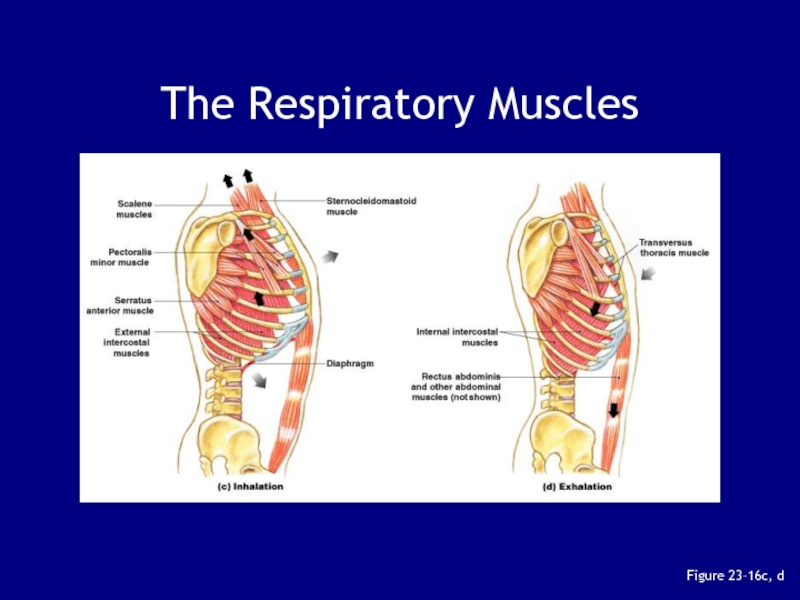
Слайд 82Figure 23–16a, b
The Respiratory Muscles
Most important are:
the diaphragm
external intracostal
muscles of the ribs
accessory respiratory muscles:
activated when respiration increases significantly
Слайд 853 Muscle Groups of Inhalation
Diaphragm:
contraction draws air into lungs
75%
of normal air movement
External intracostal muscles:
assist inhalation
25% of normal air
movementAccessory muscles assist in elevating ribs:
sternocleidomastoid
serratus anterior
pectoralis minor
scalene muscles
Слайд 86Muscles of Active Exhalation
Internal intercostal and transversus thoracis muscles:
depress
the ribs
Abdominal muscles:
compress the abdomen
force diaphragm upward
Слайд 87Modes of Breathing
Respiratory movements are classified:
by pattern of muscle activity
into
quiet breathing and forced breathing
Слайд 88Quiet Breathing (Eupnea)
Involves active inhalation and passive exhalation
Diaphragmatic breathing
or deep breathing:
is dominated by diaphragm
Costal breathing or shallow
breathing:is dominated by ribcage movements
Elastic Rebound
When inhalation muscles relax:
elastic components of muscles and lungs recoil
returning lungs and alveoli to original position
Слайд 89Forced Breathing
Also called hyperpnea
Involves active inhalation and exhalation
Assisted
by accessory muscles
Maximum levels occur in exhaustion
Слайд 90Respiratory Rates and Volumes
Respiratory system adapts to changing oxygen demands
by varying:
the number of breaths per minute (respiratory rate)
the volume
of air moved per breath (tidal volume) Слайд 91Respiratory Minute Volume
Amount of air moved per minute
Is calculated by:
respiratory
rate tidal volume
Measures pulmonary ventilation
Anatomic
Dead SpaceOnly a part of respiratory minute volume reaches alveolar exchange surfaces
Volume of air remaining in conducting passages is anatomic dead space
Слайд 92Alveolar Ventilation
Amount of air reaching alveoli each minute
Calculated as:
tidal
volume — anatomic dead space respiratory rate
Alveoli contain less
O2, more CO2 than atmospheric air:because air mixes with exhaled air
Слайд 93Alveolar Ventilation Rate
Determined by respiratory rate and tidal volume:
for a
given respiratory rate:
increasing tidal volume increases alveolar ventilation rate
for a
given tidal volume:increasing respiratory rate increases alveolar ventilation
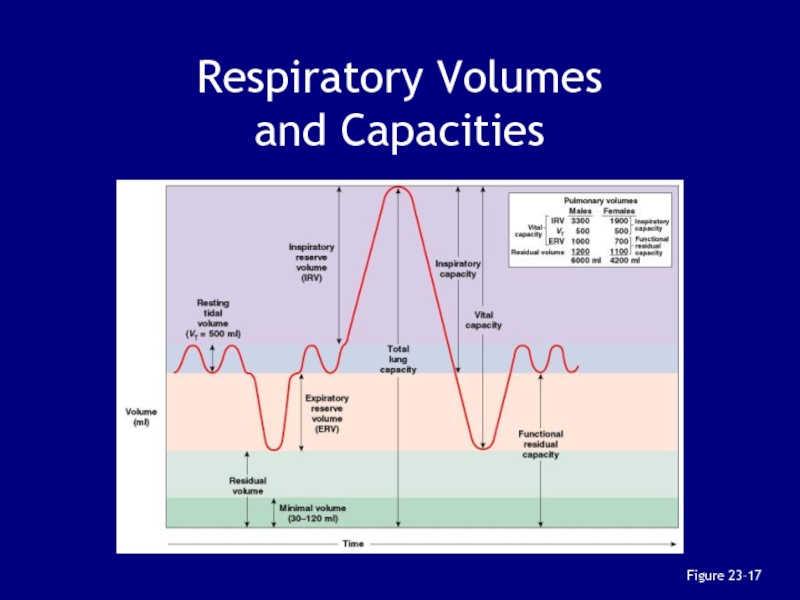
Слайд 95Lung Volume
Total lung volume is divided into a series of
volumes and capacities useful in diagnosis
Pulmonary Function Tests
Measure rates and
volumes of air movementsСлайд 964 Pulmonary Volumes
Resting tidal volume:
in a normal respiratory cycle
Expiratory
reserve volume (ERV):
after a normal exhalation
Residual volume:
after maximal exhalation
minimal volume
(in a collapsed lung)Inspiratory reserve volume (IRV):
after a normal inspiration
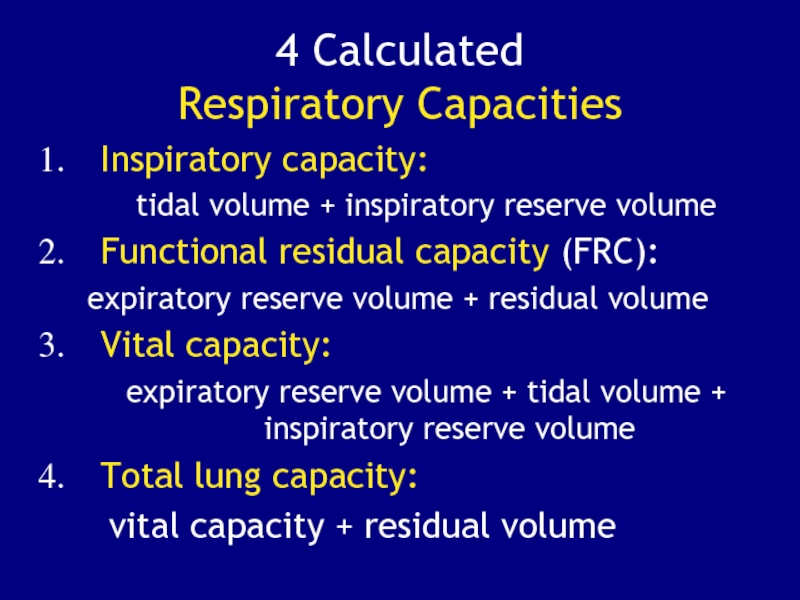
Слайд 974 Calculated
Respiratory Capacities
Inspiratory capacity:
tidal volume + inspiratory
reserve volume
Functional residual capacity (FRC):
expiratory reserve volume + residual
volumeVital capacity:
expiratory reserve volume + tidal volume + inspiratory reserve volume
Total lung capacity:
vital capacity + residual volume
Слайд 98Gas Exchange
Occurs between blood and alveolar air
Across the respiratory membrane
Depends
on:
partial pressures of the gases
diffusion of molecules between gas and
liquidInterActive Physiology: Respiratory System: Gas Exchange
PLAY
Слайд 99The Gas Laws
Diffusion occurs in response to concentration gradients
Rate of
diffusion depends on physical principles, or gas laws
e.g., Boyle’s law
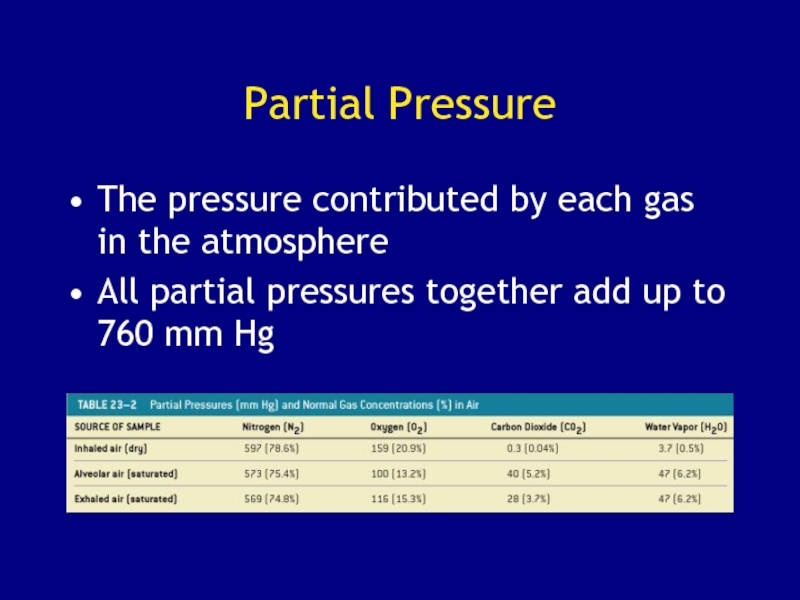
Слайд 100Composition of Air
Nitrogen (N2) about 78.6%
Oxygen (O2) about 20.9%
Water vapor
(H2O) about 0.5%
Carbon dioxide (CO2) about 0.04%
Слайд 101Gas Pressure
Atmospheric pressure (760 mm Hg):
produced by air molecules bumping
into each other
Each gas contributes to the total pressure:
in proportion
to its number of molecules (Dalton’s law)Слайд 102Partial Pressure
The pressure contributed by each gas in the
atmosphere
All partial pressures together add up to 760 mm Hg
Слайд 103Henry’s Law
Figure 23–18
When gas under pressure comes in contact with
liquid:
gas dissolves in liquid until equilibrium is reached
At a given
temperature:amount of a gas in solution is proportional to partial pressure of that gas
Слайд 104Gas Content & Solubility in
body fluids
The actual amount of
a gas in solution (at given partial pressure and temperature)
depends on the solubility of that gas in that particular liquidCO2 is very soluble
O2 is less soluble
N2 has very low solubility
Слайд 105Diffusion and the
Respiratory Membrane
Direction and rate of diffusion of
gases across the respiratory membrane determine different partial pressures and
solubilitiesСлайд 106Efficiency of Gas
Exchange
Due to:
– substantial differences in partial pressure across
the respiratory membrane
– distances involved in gas exchange are small
O2 and
CO2 are lipid soluble– total surface area is large
– blood flow and air flow are coordinated
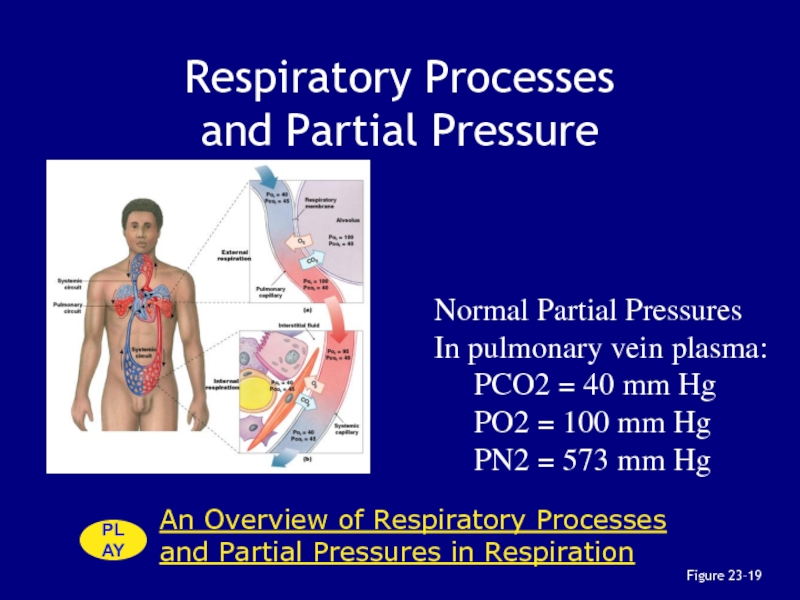
Слайд 107Respiratory Processes
and Partial Pressure
Figure 23–19
An Overview of Respiratory Processes
and Partial Pressures in Respiration
PLAY
Normal Partial Pressures
In pulmonary vein plasma:
PCO2
= 40 mm HgPO2 = 100 mm Hg
PN2 = 573 mm Hg
Слайд 108O2 and CO2
Blood arriving in pulmonary arteries has:
low PO2
high
PCO2
The concentration gradient causes:
O2 to enter blood
CO2 to leave
bloodRapid exchange allows blood and alveolar air to reach equilibrium
Слайд 109Respiration: Gas Mixture in Air
PLAY
Mixing
Oxygenated blood mixes with unoxygenated blood
from conducting passageways
Lowers the PO2 of blood entering systemic
circuit (about 95 mm Hg)Слайд 110Interstitial Fluid
PO2 40 mm Hg
PCO2 45 mm Hg
Concentration
gradient in peripheral capillaries is opposite of lungs:
CO2 diffuses into
bloodO2 diffuses out of blood
Слайд 111How is oxygen picked up, transported, and released in the
blood?
What is the structure and function of hemoglobin?
Слайд 112Gas Pickup and Delivery
Blood plasma can’t transport enough O2 or
CO2 to meet physiological needs
Red Blood Cells (RBCs)Transport O2 to, and CO2 from, peripheral tissues
Remove O2 and CO2 from plasma, allowing gases to diffuse into blood
Слайд 113Oxygen Transport
O2 binds to iron ions in hemoglobin (Hb) molecules:
in
a reversible reaction
Each RBC has about 280 million Hb molecules:
each
binds 4 oxygen molecules -saturatedThe percentage of heme units in a hemoglobin molecule:
that contain bound oxygen
Respiration: Oxygen and Carbon Dioxide Transport
PLAY
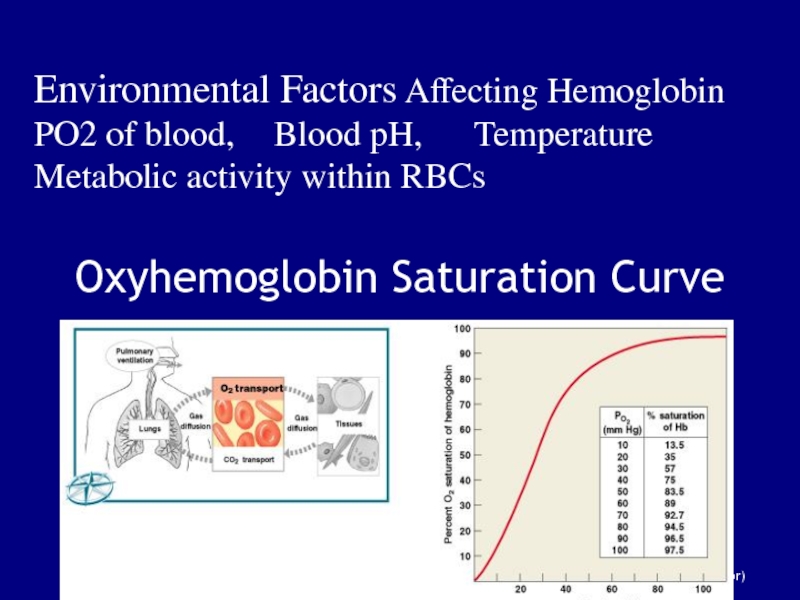
Слайд 114Oxyhemoglobin Saturation Curve
Figure 23–20 (Navigator)
Environmental Factors Affecting Hemoglobin
PO2 of blood,
Blood pH, Temperature
Metabolic activity within RBCs
Слайд 115Oxyhemoglobin Saturation Curve
Is a graph relating the saturation of hemoglobin
to partial pressure of oxygen:
higher PO2 results in greater Hb
saturationIs a curve rather than a straight line:
because Hb changes shape each time a molecule of O2 is bound
each O2 bound makes next O2 binding easier
allows Hb to bind O2 when O2 levels are low
Слайд 116Oxygen Reserves
O2 diffuses:
from peripheral capillaries (high PO2)
into interstitial fluid (low
PO2)
Amount of O2 released depends on interstitial PO2
Up to
3/4 may be reserved by RBCs Carbon Monoxide
CO from burning fuels:
binds strongly to hemoglobin
takes the place of O2
can result in carbon monoxide poisoning
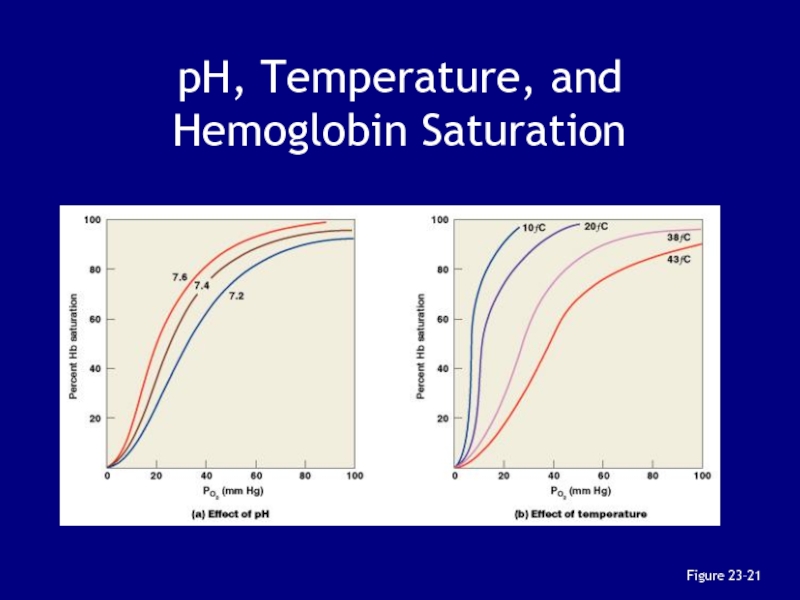
Слайд 118The Oxyhemoglobin
Saturation Curve
Is standardized for normal blood (pH
7.4, 37°C)
When pH drops or temperature rises:
more oxygen is released
curve
shift to rightWhen pH rises or temperature drops:
less oxygen is released
curve shifts to left
Слайд 119The Bohr Effect
Is the effect of pH on hemoglobin saturation
curve
Caused by CO2:
CO2 diffuses into RBC
an enzyme, called carbonic anhydrase,
catalyzes reaction with H2Oproduces carbonic acid (H2CO3)
Carbonic acid (H2CO3):
dissociates into hydrogen ion (H+) and bicarbonate ion (HCO3—)
Hydrogen ions diffuse out of RBC, lowering pH
Слайд 1202,3-biphosphoglycerate (BPG)
RBCs generate ATP by glycolysis:
forming lactic acid and
BPG
BPG directly affects O2 binding and release:
more BPG, more
oxygen releasedBPG levels rise:
when pH increases
when stimulated by certain hormones
If BPG levels are too low:
hemoglobin will not release oxygen
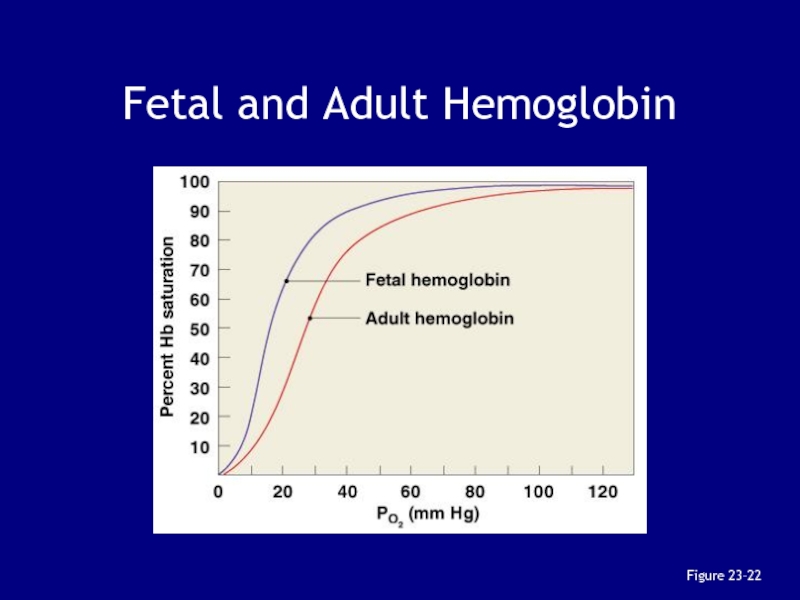
Слайд 122Fetal and Adult Hemoglobin
The structure of fetal hemoglobin:
differs from that
of adult Hb
At the same PO2:
fetal Hb binds more O2
than adult Hbwhich allows fetus to take O2 from maternal blood
Слайд 123KEY CONCEPT
Hemoglobin in RBCs:
carries most blood oxygen
releases it in response
to low O2 partial pressure in surrounding plasma
If PO2 increases,
hemoglobin binds oxygen If PO2 decreases, hemoglobin releases oxygen
At a given PO2:
hemoglobin will release additional oxygen
if pH decreases or temperature increases
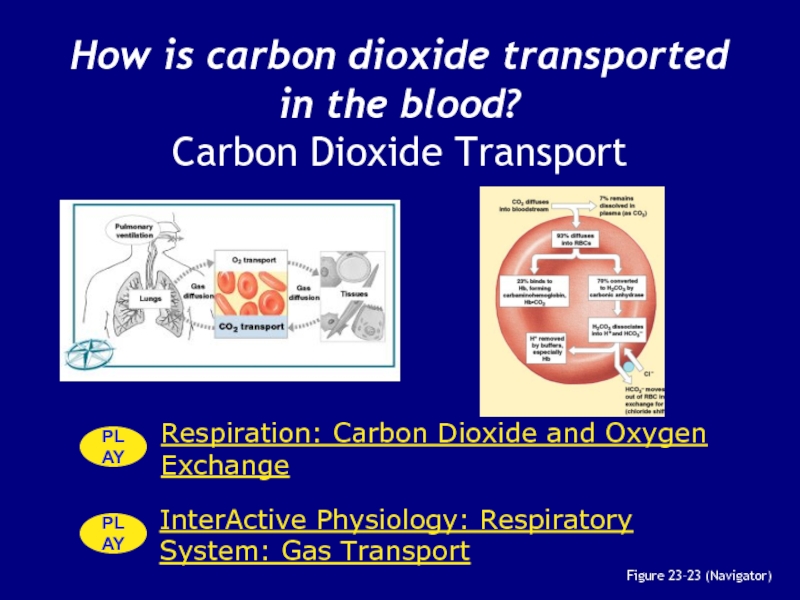
Слайд 124How is carbon dioxide transported in the blood? Carbon Dioxide
Transport
Figure 23–23 (Navigator)
Respiration: Carbon Dioxide and Oxygen Exchange
PLAY
InterActive Physiology: Respiratory
System: Gas TransportPLAY
Слайд 125Carbon Dioxide (CO2)
Is generated as a byproduct of aerobic
metabolism (cellular respiration)
CO2
in the Blood StreamMay be:
converted to carbonic acid
bound to protein portion of hemoglobin
dissolved in plasma
Bicarbonate Ions
Move into plasma by an exchange mechanism (the chloride shift) that takes in Cl— ions without using ATP
Слайд 126CO2 in the Blood Stream
70% is transported as carbonic acid
(H2CO3):
which dissociates into H+ and bicarbonate (HCO3—)
23% is bound to
amino groups of globular proteins in Hb molecule:forming carbaminohemoglobin
7% is transported as CO2 dissolved in plasma
Слайд 127KEY CONCEPT
CO2 travels in the bloodstream primarily as bicarbonate ions,
which form through dissociation of carbonic acid produced by carbonic
anhydrase in RBCsLesser amounts of CO2 are bound to Hb or dissolved in plasma
Слайд 129InterActive Physiology: Respiratory System: Control of Respiration
PLAY
Control of Respiration
Gas diffusion
at peripheral and alveolar capillaries maintain balance by:
changes in blood
flow and oxygen deliverychanges in depth and rate of respiration
Слайд 130Local Regulation of
O2 Transport (1 of 2)
O2 delivery in
tissues and pickup at lungs are regulated by:
rising PCO2 levels:
relaxes
smooth muscle in arterioles and capillariesincreases blood flow
coordination of lung perfusion and alveolar ventilation:
shifting blood flow
PCO2 levels:
control bronchoconstriction and bronchodilation
Слайд 131Respiratory Centers of the Brain
When oxygen demand rises:
cardiac output and
respiratory rates increase under neural control
Have both voluntary and involuntary
componentsInvoluntary Centers
Regulate respiratory muscles
In response to sensory information
Слайд 132Voluntary Centers
In cerebral cortex affect:
respiratory centers of pons and medulla
oblongata
motor neurons that control respiratory muscles
The Respiratory Centers
3 pairs of
nuclei in the reticular formation of medulla oblongata and ponsСлайд 133Respiratory Rhythmicity Centers of the Medulla Oblongata
Set the pace
of respiration
Can be divided into 2 groups:
Dorsal respiratory group (DRG)-
Inspiratory
centerFunctions in quiet and forced breathing
Inspiratory and expiratory center
Functions only in forced breathing
Ventral respiratory group (VRG)
Слайд 134Figure 23–25a
Quiet Breathing
Brief activity in the DRG:
stimulates inspiratory muscles
DRG neurons
become inactive:
allowing passive exhalation
Слайд 135Figure 23–25b
Forced Breathing
Increased activity in DRG:
stimulates VRG
which activates accessory inspiratory
muscles
After inhalation:
expiratory center neurons stimulate active exhalation
Слайд 136The Apneustic and Pneumotaxic
Centers of the Pons
Paired nuclei
that adjust output of respiratory rhythmicity centers:
regulating respiratory rate and
depth of respirationAn Apneustic Center
Provides continuous stimulation to its DRG center
Pneumotaxic Centers
Inhibit the apneustic centers
Promote passive or active exhalation
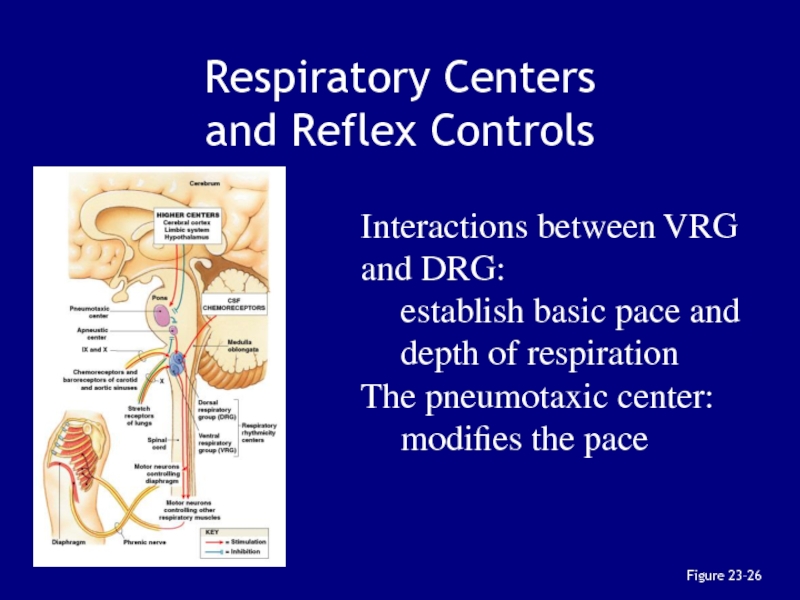
Слайд 137Respiratory Centers
and Reflex Controls
Figure 23–26
Interactions between VRG and DRG:
establish
basic pace and depth of respiration
The pneumotaxic center:
modifies the pace
Слайд 138SIDS
Also known as sudden infant death syndrome
Disrupts normal respiratory
reflex pattern
May result from connection problems between pacemaker complex and
respiratory centers Respiratory Reflexes-Changes in patterns of respiration induced by sensory input
Слайд 1395 Sensory Modifiers of Respiratory Center Activities
Chemoreceptors are sensitive to:
PCO2,
PO2, or pH
of blood or cerebrospinal fluid
Baroreceptors in aortic
or carotic sinuses:sensitive to changes in blood pressure
Слайд 1405 Sensory Modifiers of Respiratory Center Activities
Stretch receptors:
respond to changes
in lung volume
Irritating physical or chemical stimuli:
in nasal cavity,
larynx, or bronchial treeOther sensations including:
pain
changes in body temperature
abnormal visceral sensations
Слайд 141Chemoreceptor Reflexes
Respiratory centers are strongly influenced by chemoreceptor input from:
*
cranial nerve IX -The glossopharyngeal nerve:
from carotid bodies
stimulated by changes
in blood pH or PO2 * cranial nerve X -The vagus nerve:
from aortic bodies
stimulated by changes in blood pH or PO2
* receptors that monitor cerebrospinal fluid-
Are on ventrolateral surface of medulla oblongata
Respond to PCO2 and pH of CSF
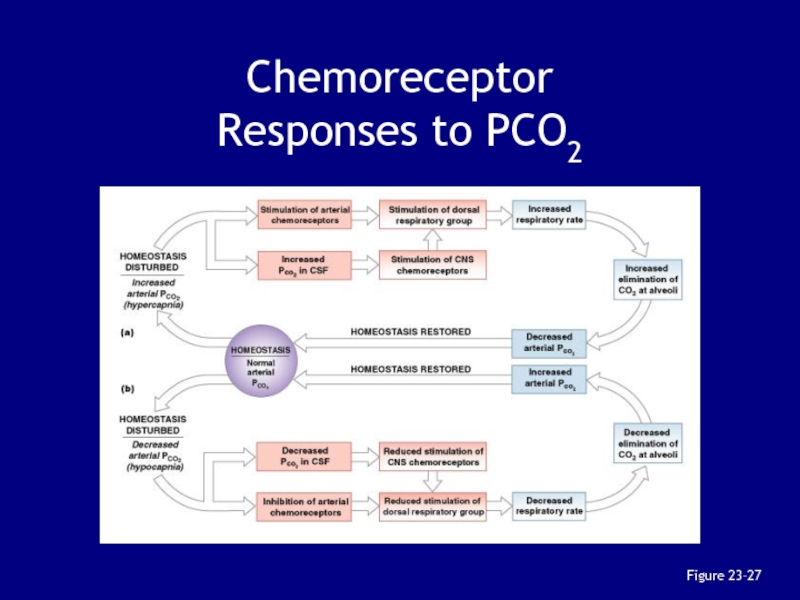
Слайд 143 Hypercapnia- An increase in arterial PCO2
Stimulates chemoreceptors
in the medulla oblongata:
to restore homeostasis
Hypoventilation- A common cause of
hypercapniaAbnormally low respiration rate:
allows CO2 build-up in blood
Hyperventilation-Excessive ventilation
Results in abnormally low PCO2 (hypocapnia)
Stimulates chemoreceptors to decrease respiratory rate
Слайд 144Baroreceptor Reflexes
Carotid and aortic baroreceptor stimulation:
affects blood pressure and respiratory
centers
When blood pressure falls:
respiration increases
When blood pressure increases:
respiration decreases
Слайд 145Protective Reflexes
Triggered by receptors in epithelium of respiratory tract
when lungs are exposed to:
toxic vapors
chemicals irritants
mechanical stimulation
Cause sneezing, coughing,
and laryngeal spasmСлайд 146Apnea
A period of suspended respiration
Normally followed by explosive exhalation
to clear airways:
sneezing and coughing
Laryngeal SpasmTemporarily closes airway:
to prevent foreign substances from entering
Слайд 147The Cerebral Cortex and Respiratory Centers
Strong emotions:
can stimulate respiratory centers
in hypothalamus
2. Temporarily closes airway:
to prevent foreign substances from entering
Anticipation
of strenuous exercise:can increase respiratory rate and cardiac output
by sympathetic stimulation
Слайд 148KEY CONCEPTS
A basic pace of respiration is established between respiratory
centers in the pons and medulla oblongata, and modified in
response to input from:Chemoreceptors, baroreceptors, stretch receptors
In general, CO2 levels, rather than O2 levels, are primary drivers of respiratory activity
Respiratory activity can be interrupted by protective reflexes and adjusted by the conscious control of respiratory muscles
Слайд 149Changes in Respiratory
System at Birth (1)
Before birth:
pulmonary vessels
are collapsed
lungs contain no air
During delivery:
placental connection is lost
blood PO2
fallsPCO2 rises
At birth:
newborn overcomes force of surface tension to inflate bronchial tree and alveoli and take first breath
Слайд 150Changes in Respiratory
System at Birth (2)
Large drop in pressure
at first breath:
pulls blood into pulmonary circulation
closing foramen ovale and
ductus arteriosusredirecting fetal blood circulation patterns
Subsequent breaths:
fully inflate alveoli
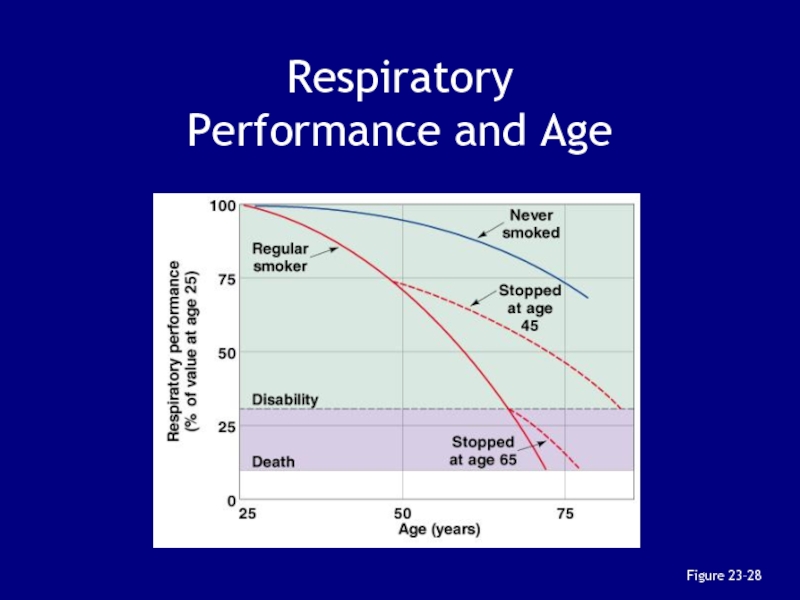
Слайд 1523 Effects of Aging on
the Respiratory System
Elastic tissues deteriorate:
reducing
lung compliance
lowering vital capacity
Arthritic changes:
restrict chest movements
limit respiratory minute volume
Emphysema:
affects
individuals over age 50depending on exposure to respiratory irritants (e.g., cigarette smoke)
Слайд 153Integration with Other Systems
Maintaining homeostatic O2 and CO2 levels in
peripheral tissues requires coordination between several systems:
particularly the respiratory
and cardiovascular systemsСлайд 154Coordination of Respiratory
and Cardiovascular Systems
Improves efficiency of gas exchange:
by
controlling lung perfusion
Increases respiratory drive:
through chemoreceptor stimulation
Raises cardiac output and
blood flow:through baroreceptor stimulation
Слайд 156SUMMARY (1 of 4)
5 functions of the respiratory system:
gas
exchange between air and circulating blood
moving air to and from
exchange surfacesprotection of respiratory surfaces
sound production
facilitating olfaction
Structures and functions of the respiratory tract:
alveoli
respiratory mucosa
lamina propria
respiratory defense system
Слайд 157SUMMARY (2 of 4)
Structures and functions of the upper respiratory
system:
the nose and nasal cavity
the pharynx
Structures and functions of the
larynx:cartilages and ligaments
sound production
the laryngeal musculature
Structures and functions of the trachea and primary bronchi
Слайд 158SUMMARY (3 of 4)
Structures and functions of the lungs:
lobes and
surfaces, the bronchi
the bronchioles, alveoli and alveolar ducts
blood supply to
the lungspleural cavities and membranes
Respiratory physiology:
external respiration
internal respiration
Pulmonary ventilation:
air movement
pressure changes
the mechanics of breathing
respiratory rates and volumes
Слайд 159SUMMARY (4 of 4)
Gas exchange:
the gas laws
diffusion and respiration
Gas pickup
and delivery:
partial pressure
oxygen transport (RBCs and hemoglobin)
carbon dioxide transport
Control of
respiration:local regulation (lung perfusion, alveolar ventilation)
respiratory centers of the brain
respiratory reflexes
voluntary control of respiration
Changes in the respiratory system at birth
Aging and the respiratory system