Слайд 1Drugs affecting
the cardiovascular system
Cardiotonic agents
Antiarrythmic agents
Слайд 2Cardiotonic agents – are the agents that stimulate cardiac activity.
They can be divided into the following groups:
1.Agents increasing intracellular
content of Ca ions
Na+,K+-ATPase inhibitors (cardiac glycosides): digoxin, strophanthin, corglyconum
Agents increasing cAMP content (non-glycosides structure):
Drugs increasing cAMP content by activating adenylyl cyclase (agents stimulating β1-adrenoreceptors): dopamine, dobutamine
Drugs increasing cAMP content by inhibiting phosphodiesterase 3: milrinone
2. Agents increasing the sensitivity of myofibrils to Ca ions - levosimendan
Слайд 4Cardiac glycosides are agents of plant origin. They produce marked
cardiotonic effect, but they do not increase the heart rate.
They can be used for the treatment of acute and chronic heart failure.
The other drugs increase contractile force and heart rate. They are used for the treatment of acute heart failure only.
Слайд 5Digitalis
Convallaria
Strophanthus
Adonis vernalis
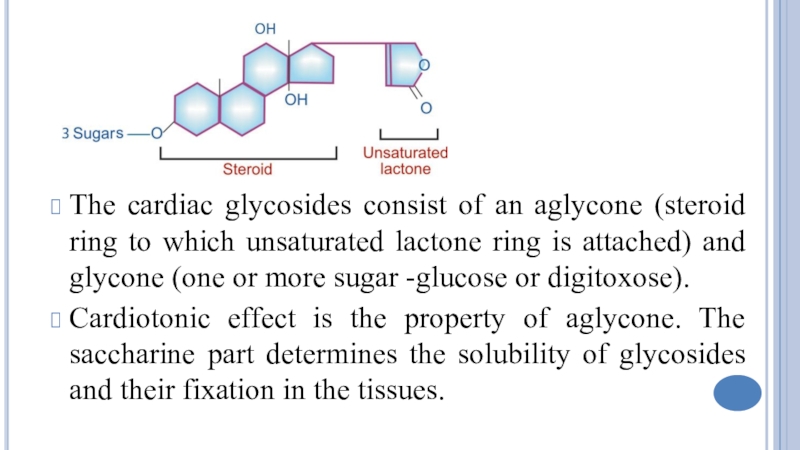
Слайд 6The cardiac glycosides consist of an aglycone (steroid ring to
which unsaturated lactone ring is attached) and glycone (one or
more sugar -glucose or digitoxose).
Cardiotonic effect is the property of aglycone. The saccharine part determines the solubility of glycosides and their fixation in the tissues.
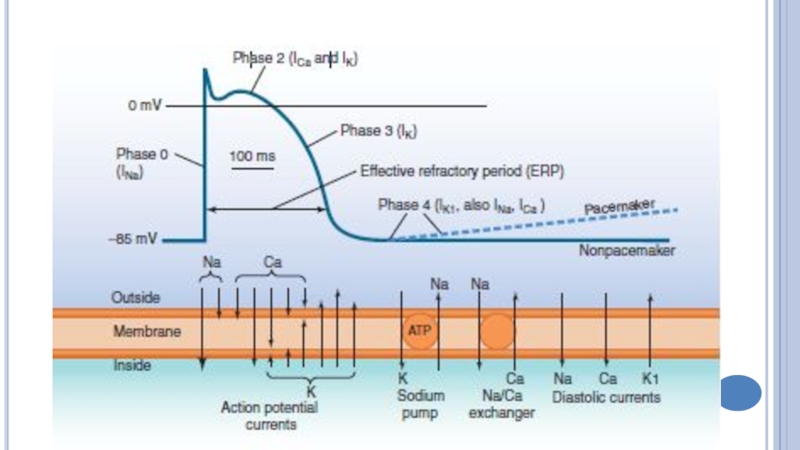
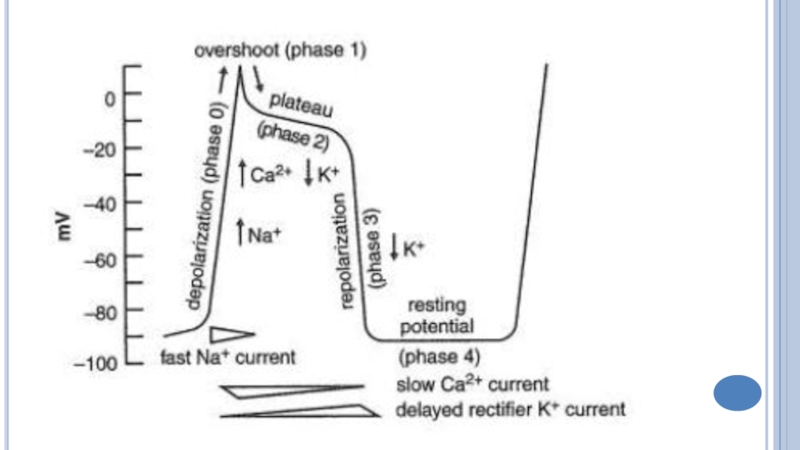
Слайд 8Cardiotonic effect (increase in systole, positive inotropic action)
CGs block Na+,K+-ATPase
→ Na+,K+ flow disturbance → ↑ intracellular Na+, but ↓
K+ → ↑ intracellular Ca (Ca enters the cardiomyocites from outside via the Ca L-channels and releases from the sarcoplasmatic reticulum) → Ca interacts with the troponine complex and eliminates its suppressive effect on the contractile proteins.
Actin interacts with myosin→ rapid and intensive myocardial contraction.
There is more complete emptying of failing and dilated ventricles—cardiac output is increased and end-diastolic volume is reduced.
Слайд 9CGs decrease heart rate (negative chronotropic effect). They lengthen diastole
and create the most economical regimen of cardiac work (restoring
the energetic resources of the myocardium).
Mechanism: ↑ vagal stimulation, cardio-cardiac reflex.
systole
diastole
Before treatment
After treatment
Слайд 10A-V conduction is demonstrably slowed by therapeutic doses (negative dromotropic
effect).
Myocardial excitability is increased (positive batmotropic effect).
CGs increase arterial
blood pressure, but decrease venous pressure. Peripheral vascular resistance decreases, blood supply and tissue oxygenation are improved. The dysfunction of organs ( the CNS, kidneys, lungs, liver, GI) gradually resolve. Edema gradually disappear.
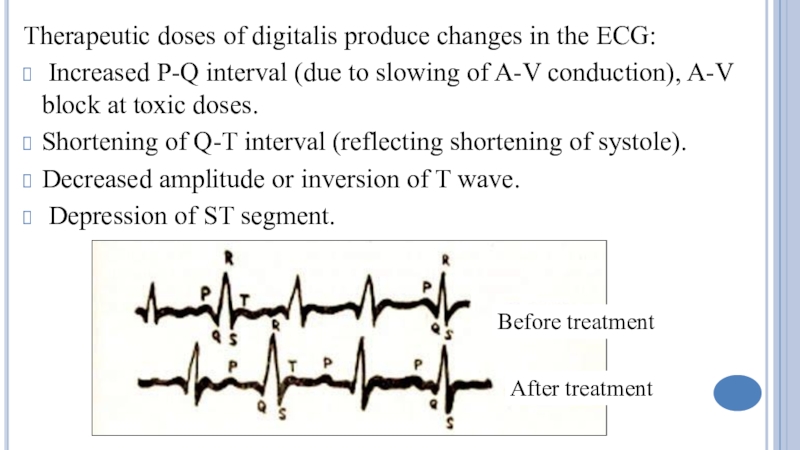
Слайд 11Therapeutic doses of digitalis produce changes in the ECG:
Increased P-Q interval (due to slowing of A-V conduction), A-V
block at toxic doses.
Shortening of Q-T interval (reflecting shortening of systole).
Decreased amplitude or inversion of T wave.
Depression of ST segment.
Before treatment
After treatment
Слайд 12Intoxication with digitalis agents
Symptoms: extrasystoles, partial or complete A-V block;
vision (colour) disturbances, fatigue, muscle weakness, dyspepsia (nausea, vomiting, diarrhea),
mental disorders (agitation, hallucinations), headache, skin rash.
Treatment: potassium agents (“Asparcam”, “Pananginum”), phenytoin, lidocaine, atropine; digoxin Fab (digibind), unithiol (contains sulfhydryl groups).
Слайд 13Dopamine causes positive inotropic effect (β1R) combined with dilatation of
kidneys and mesenteric vessels (dopamine receptors and β2 R).
D.
is used for the treatment of cardiogenic shock, is administered intravenously drip.
D. can cause tachycardia, arrhythmia, excessive increases in peripheral vascular resistance and cardiac work.
Слайд 14Levosimendan increases the sensitivity of the myofibrils of the heart
to calcium ions.
Increases intensity of heart contractions without increased myocardial
oxygen consumption.
Dilates coronary vessels, increases oxygen delivery to the myocardium.
Dilates blood vessels, reduces peripheral vascular resistance, decreases pre- and afterload.
L. is used IV for the treatment of acute cardiac failure.
Side effects: arrhythmias, hypotension, headache, dizziness.
Слайд 15Milrinone increases contractile activity of the myocardium and causes vasodilatation
(↓ the preload).
It is used intravenously drip in case of
acute cardiac decompensation.
Side effects: ↑heart rate, arrhythmia, thrombocytopenia, hypotension.
Слайд 16Antiarrhythmic drugs are used for the treatment and prophylaxis of
cardiac arrhythmias.
Classification
D. mainly blocking ion channels of the cardiomyocytes
(of the cardiac conduction system and contractile myocardium)
A) D. blocking sodium channels (membrane stabilizing D.)
Subgroup 1A: Quinidine, Procainamide
Subgroup 1B: Lidocaine, Phenytoin
Subgroup 1C: Propaphenone
Слайд 17B) D. blocking potassium channels (agents increasing the duration of
repolarization and duration of action potential; class III): Amiodaron
C)
D. blocking L-type calcium channels (class IV): Verapamil, Diltiazem
D) D. blocking sodium/potassium channels of sinoatrial node (block of If inward current; group V; bradycardic drugs): Ivabradine
Слайд 182. D.mostly affecting receptors of the afferent innervations of the
heart:
D. that suppress adrenergic effects: β-adrenoblockers – Propranolol, Metoprolol
D. that
intensify adrenergic effects: Dobutamine, Ephedrine
D. suppressing cholinergic effects: M-cholinoblockers (Atropin)
3. Other drugs possessing antiarrhythmic activity:
Cardiac glycosides, Magnesium and potassium agents
Слайд 21Quinidine, Procainamide IA class
Block slow Na channels →extend 4-phase →
↓automatism
Inhibit the conductance of fast Na channels (0 phase) →
↓AV conduction
Inhibit K channels (phase 3)→ ↑ action potential duration (APD),
↑effective refractory period (ERP), ↓ excitability
Слайд 22Quinidine is an M-blocker and can increase the heart rate
and AV conduction.
Procainamide has less M block than quinidine
and no alpha block.
Use: paroxysmal supraventricular and ventricular tachycardia, fibrillation and atrial flutter, extrasystoles
Слайд 23Side effects
Quinidine: fall in BP, AV block, vomiting, diarrhoea and
neurological effects (ringing in ears, vertigo, deafness, visual disturbances and
mental changes)
Procainamide: nausea and vomiting, weakness, mental confusion and hallucinations, hypotension hypersensitivity reactions (rashes, fever, angioedema), agranulocytosis and aplastic anaemia.
Слайд 25Lidocaine, Phenytoin
Inhibit slow Na channels - ↑ 4-phase →↓ automaticity
in ectopic foci of Purkinje fibers
L. slightly inhibits fast Na
channels→ decreases APD in PF and ventricular muscle
Drugs slightly affect conduction, increase repolarization (activate K+ channels)
Use: ventricular tachyarrhythmias (extrasystoles)
Слайд 26Lidocaine is injected intravenously drip. Side effects: headache, drowsiness, nausea,
paresthesias, vision changes, tremor, seizures.
Phenytoin is used orally. Side effects:
nystagmus, ataxia, tremor, gingival hyperplasia, dyspepsia.
Слайд 27Propaphenone
Decreases automatism; slightly affects conduction, increases repolarization and ERP.
P.
is used for the treatment of ventricular arrhythmias orally or
IV.
Side effects: nausea, vomiting, constipation, bronchospasm, weakness, fatigue, arrhythmogenic effect.
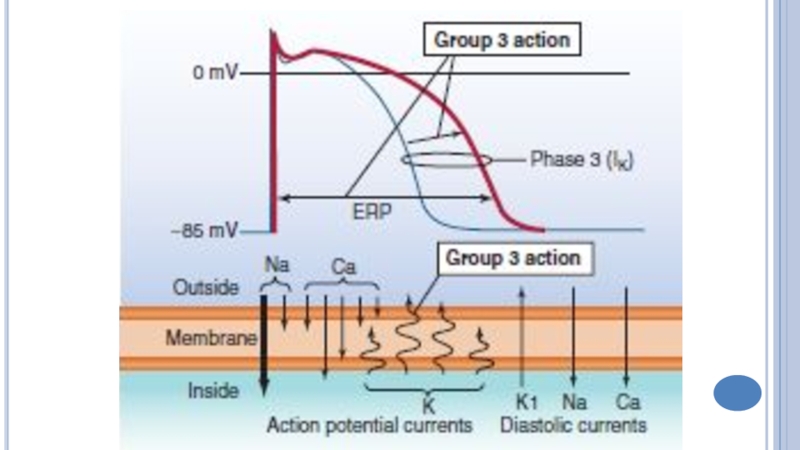
Слайд 29Amiodaron
blocks K+-channels → slows repolarization and ↑ERP;
inhibits Na+ and Ca2+channels,
↑ APD;
↓ automaticity, excitability and conduction in the SA and
AV, ectopic foci;
blocks of β – and α-AR.
Use: supraventricular and ventricular tachycardia, fibrillation and atrial flutter, extrasystoles.
Слайд 30Adverse effects: dyspepsia, pulmonary fibrosis, bradycardia, AV-blockade, blue pigmentation of
the skin and the cornea, phototoxicity, thyroid dysfunction.
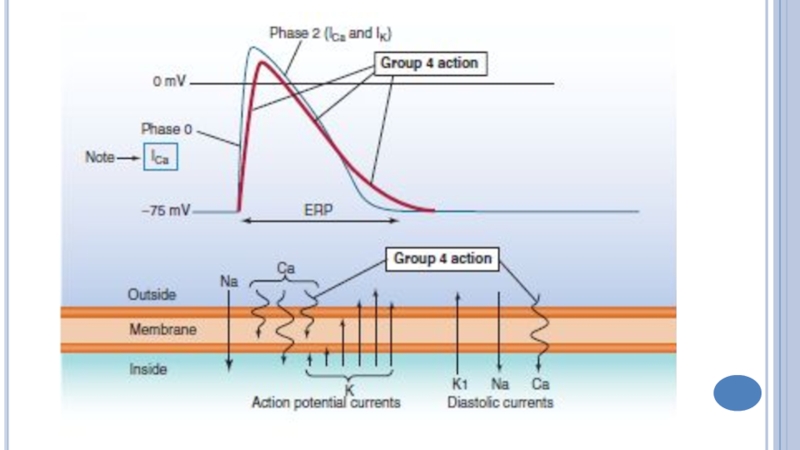
Слайд 32Verapamil, Diltiazem
Blocks the slow Ca2⁺ channels in SA and AV
nodes, ↓spontaneous diastolic depolarization (4-phase) →↓automaticity pacemaker - ↓heart rate;
Lengthens
the 0-phase of action potential - ↓conduction;
Increases ERP, ↓ excitability.
They are used: sinus tachycardia, supraventricular tachyarrhythmia.
Side effects: bradycardia, decreased heart contractility, ↓BP; dizziness, swelling of the ankles, nausea, constipation.