Разделы презентаций
- Разное
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Геометрия
- Детские презентации
- Информатика
- История
- Литература
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
Role of Ca 2+ ions in mechanisms of cell signaling
Содержание
- 1. Role of Ca 2+ ions in mechanisms of cell signaling
- 2. The ion Ca2+ is also the fifth-most-abundant dissolved
- 3. Слайд 3
- 4. Calcium absorption 1 – Cholesterol is precursor
- 5. Calcium absorption 3 – in liver, 25-hydroxylase
- 6. Calcium absorption Calcium is absorbed across the
- 7. Ca2+Skeletal muscle contractionNeuronal transmissionStructural: bones and teeth
- 8. Слайд 8
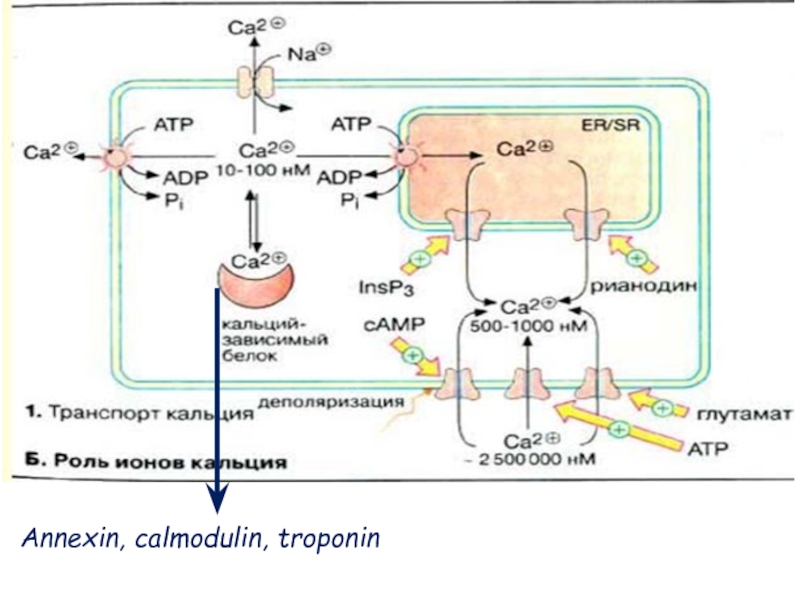
- 9. Annexin, calmodulin, troponin
- 10. Function of calcium ions as secondary messenger:Са2+
- 11. Ca2+Catalyzing the production of nitric oxide (NO)
- 12. Protein kinase C: Regulatory domain & catalytic
- 13. Слайд 13
- 14. Слайд 14
- 15. Слайд 15
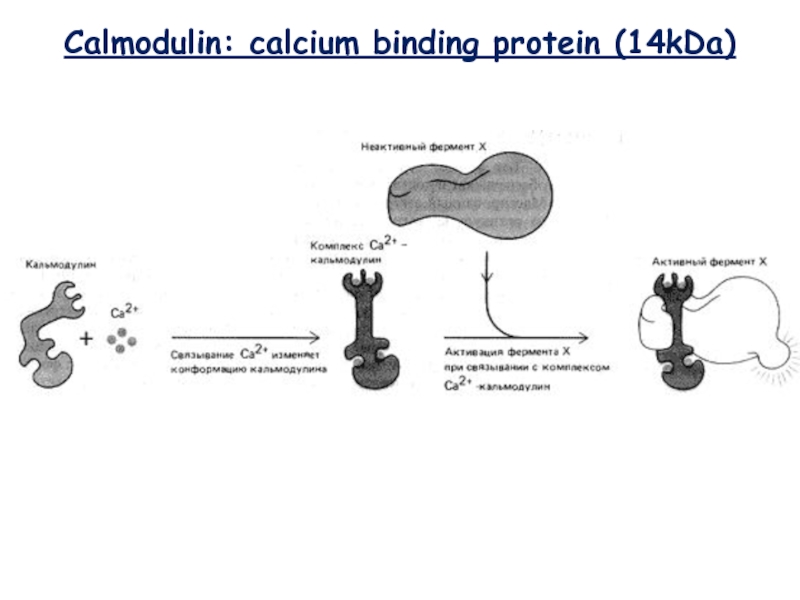
- 16. Calmodulin: calcium binding protein (14kDa)
- 17. Calmodulin: calcium binding protein (14kDa)
- 18. Слайд 18
- 19. Annexin A1 belongs to the annexin family of Ca2+-dependent phospholipid-binding
- 20. Neuronal transmission In the resting state, neurotransmitters are
- 21. Neuronal transmission Calcium (Ca2+) is a vital element in
- 22. Слайд 22
- 23. Слайд 23
- 24. Слайд 24
- 25. Слайд 25
- 26. Слайд 26
- 27. Слайд 27
- 28. Слайд 28
- 29. Functioning of heart The importance of calcium-dependent signaling
- 30. Functioning of heart Cardiac muscle fibers contract via
- 31. Functioning of heart During stimulation of the muscle
- 32. Functioning of heart Excitation-contraction coupling describes the process
- 33. Functioning of heart The pathway of contraction can
- 34. Functioning of heart
- 35. Functioning of heart
- 36. Слайд 36
- 37. Слайд 37
- 38. Слайд 38
- 39. Слайд 39
- 40. Impact on cytoskeleton Formation is regulated by
- 41. Regulation of Ca2+ ions in blood The main
- 42. Regulation of Ca2+ ions in bloodPre-parathyroid hormone
- 43. Regulation of Ca2+ ions in blood Biological action
- 44. Regulation of Ca2+ ions in blood Calcitonin is
- 45. Thanks for attention!!!
- 46. Скачать презентанцию
Слайды и текст этой презентации
Слайд 2 The ion Ca2+ is also the fifth-most-abundant dissolved ion in seawater by
both molarity and mass, after Na, Cl, Mn, S.
Melting
point 1115 K (842 °C, 1548 °F)Boiling point 1757 K (1484 °C, 2703 °F)
Density near r.t. 1.55 g/cm3
when liquid, at m.p.1.378 g/cm3
Calcium is a soft grayish-yellow alkaline earth metal, fifth-most-abundant element by mass in the Earth's crust.
Слайд 4Calcium absorption
1 – Cholesterol is precursor of Calcitriol;
2
– In skin 7-dehydrocholesterol is converted (not enzymatically) into cholecalciferol
(vitamin D3);Слайд 5Calcium absorption
3 – in liver, 25-hydroxylase converts cholecalciferol into
calcidiol;
4 – in kidney the formation of calcitriol is catalyzed
by 1α-hydroxylase.In the cells of intestine, calcitriol induce the synthesis of Са2+-transporting proteins, which provide absorption of calcium ions and transport to the blood.
In kidneys, calcitriol stimulate reabsorption of calcium and phosphate ions.
Слайд 6Calcium absorption
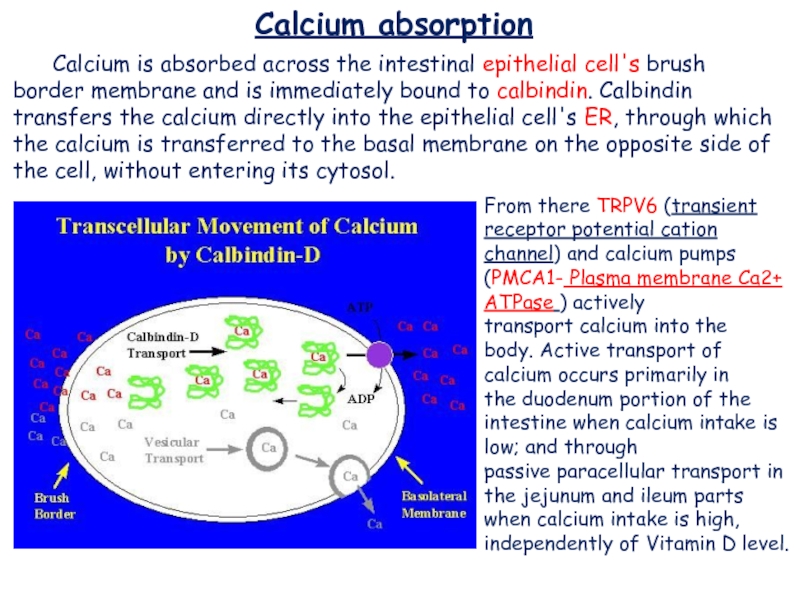
Calcium is absorbed across the intestinal epithelial cell's brush
border membrane and is immediately bound to calbindin. Calbindin transfers the calcium
directly into the epithelial cell's ER, through which the calcium is transferred to the basal membrane on the opposite side of the cell, without entering its cytosol.From there TRPV6 (transient receptor potential cation channel) and calcium pumps (PMCA1- Plasma membrane Ca2+ ATPase ) actively
transport calcium into the body. Active transport of calcium occurs primarily in the duodenum portion of the intestine when calcium intake is low; and through passive paracellular transport in the jejunum and ileum parts when calcium intake is high, independently of Vitamin D level.
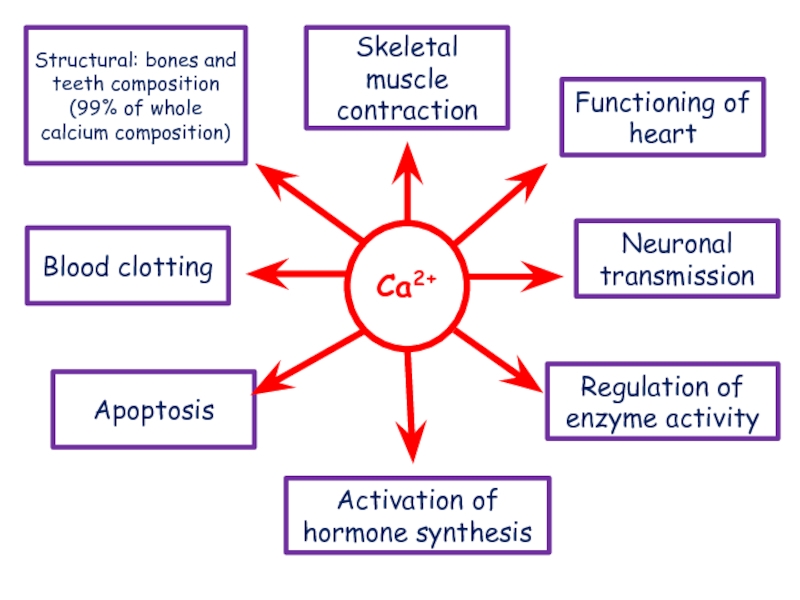
Слайд 7Ca2+
Skeletal muscle contraction
Neuronal transmission
Structural: bones and teeth composition (99% of
whole calcium composition)
Functioning of heart
Blood clotting
Apoptosis
Regulation of enzyme activity
Activation of hormone synthesis
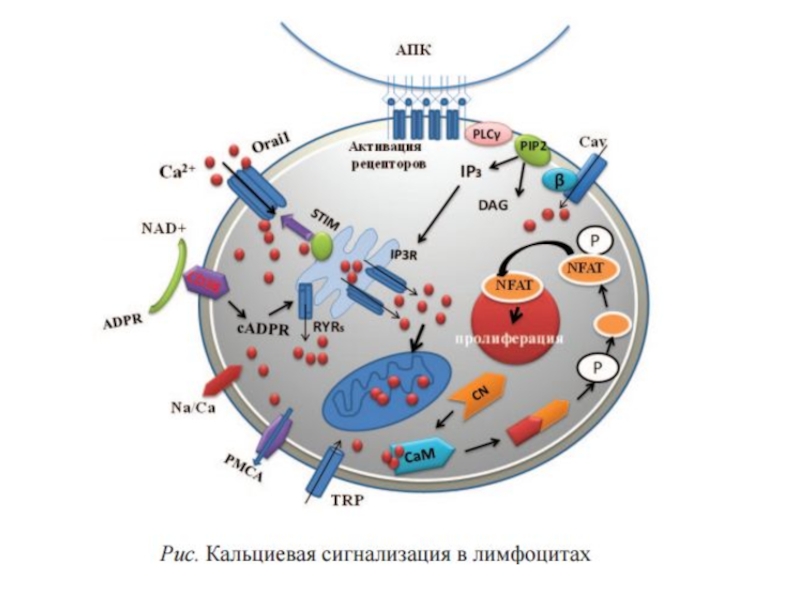
Слайд 10Function of calcium ions as secondary messenger:
Са2+ directly binds with
effector molecules (Protein kinases)
Са2+ binds with inactive cytoplasmic modulators
of effector molecules and activates them. Слайд 11Ca2+
Catalyzing the production of nitric oxide (NO) from L-arginine.
Protein kinases
(PKs) are the effectors of phosphorylation is a phosphotransferase enzyme
that catalyzes the interconversion of adenine nucleotides, and plays an important role in cellular energy homeostasis (Protein kinase C).Co factors -> nitric oxide synthase, protein phosphatases (Calcinevrin-Phosphatase IIB), and adenylate kinase, but calcium activates these enzymes in allosteric regulation in a complex with calmodulin
Слайд 12Protein kinase C:
Regulatory domain & catalytic domain tethered together
by a hinge region:
*C1 domain, present in all of
the isoforms of PKC has a binding site for DAG *C2 domain acts as a Ca2+ sensor
*Catalytic Region brings about phosphorylation Ser/Thr a.a. of proteins
*Upon activation, translocated to the plasma membrane
C1 domain
C2 domain
Ca2+
DAG
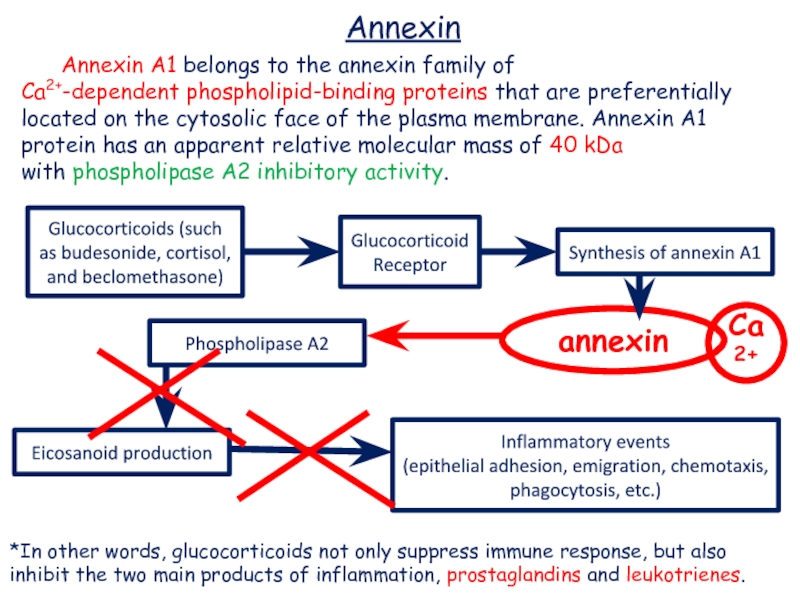
Слайд 19 Annexin A1 belongs to the annexin family of Ca2+-dependent phospholipid-binding proteins that are
preferentially located on the cytosolic face of the plasma membrane. Annexin A1
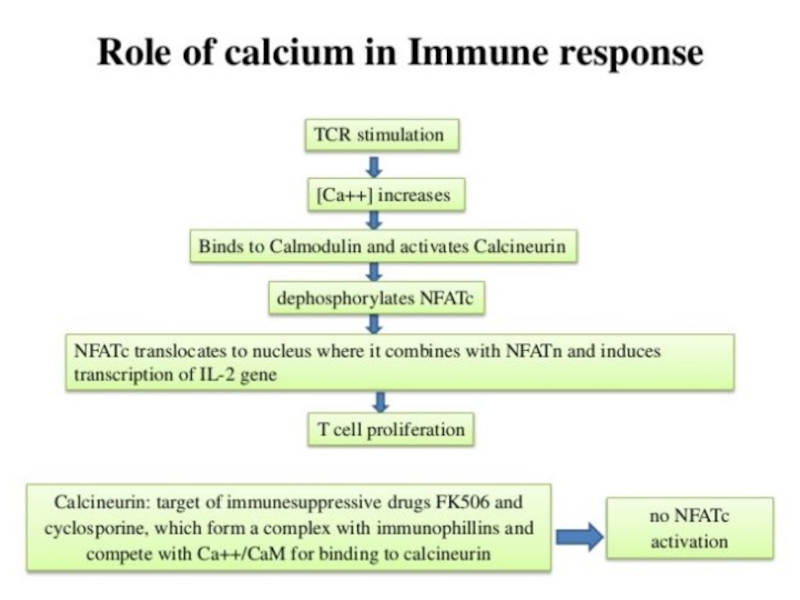
protein has an apparent relative molecular mass of 40 kDa with phospholipase A2 inhibitory activity.*In other words, glucocorticoids not only suppress immune response, but also inhibit the two main products of inflammation, prostaglandins and leukotrienes.
Annexin
Glucocorticoids (such as budesonide, cortisol, and beclomethasone)
Glucocorticoid Receptor
Synthesis of annexin A1
annexin
Ca2+
Phospholipase A2
Eicosanoid production
Inflammatory events (epithelial adhesion, emigration, chemotaxis, phagocytosis, etc.)
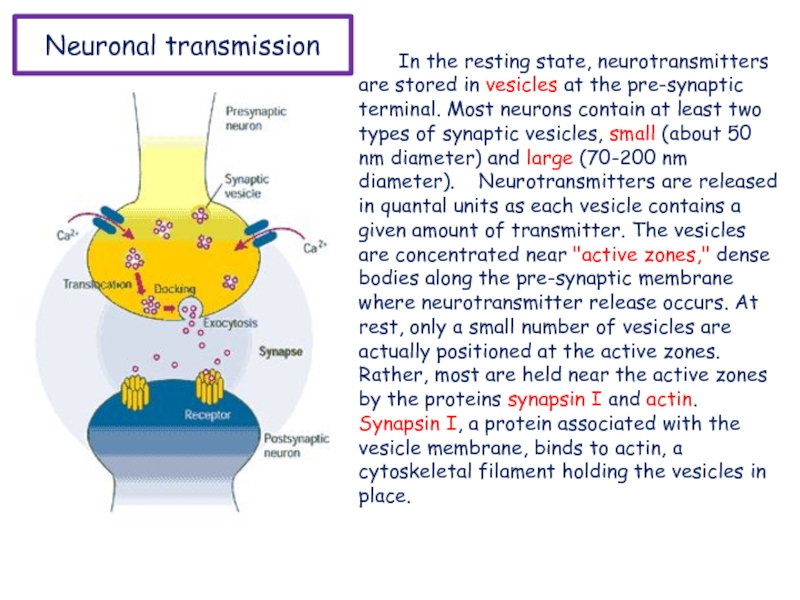
Слайд 20Neuronal transmission
In the resting state, neurotransmitters are stored in vesicles
at the pre-synaptic terminal. Most neurons contain at least two
types of synaptic vesicles, small (about 50 nm diameter) and large (70-200 nm diameter). Neurotransmitters are released in quantal units as each vesicle contains a given amount of transmitter. The vesicles are concentrated near "active zones," dense bodies along the pre-synaptic membrane where neurotransmitter release occurs. At rest, only a small number of vesicles are actually positioned at the active zones. Rather, most are held near the active zones by the proteins synapsin I and actin. Synapsin I, a protein associated with the vesicle membrane, binds to actin, a cytoskeletal filament holding the vesicles in place.Слайд 21Neuronal transmission
Calcium (Ca2+) is a vital element in the process of
neurotransmitter release; when Ca2+ channels are blocked, neurotransmitter release is inhibited.
When the action potential reaches the nerve terminal, voltage-dependent Ca2+ channels open and Ca2+ rushes into the neuron terminal due to a greater extracellular concentration.Ca2+ channels appear to be localized near the active zones of the vesicular membrane. In the giant squid neuron, it has been found that Ca2+ influx is ten times greater in the area of the active zone than elsewhere in the neuron. Furthermore, during an action potential Ca2+ concentration at the active zone can rise one-thousand fold, from 100 nM (nano-molar concentration) to 100 micro-M within a few hundred microseconds. The observation of intramembranous proteins thought to be Ca2+ channels near active zones is consistent with rapid neurotransmitter release following Ca2+ influx.
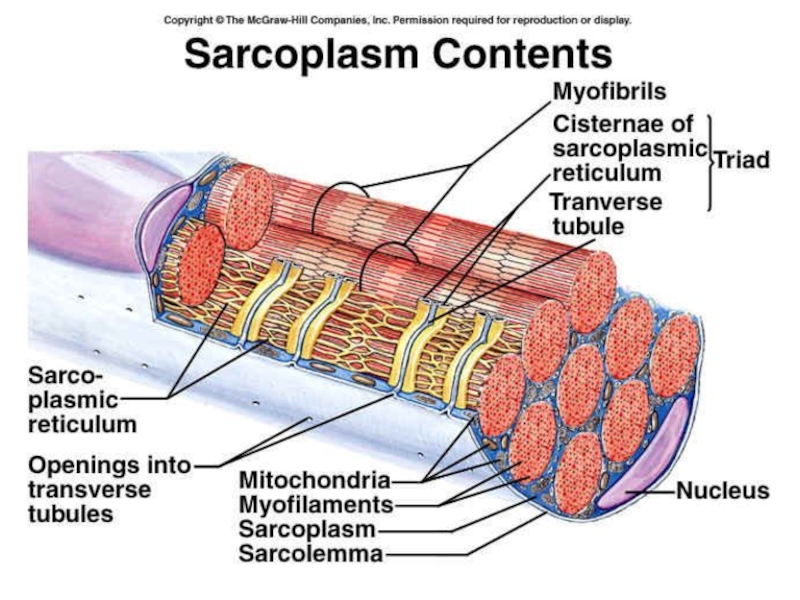
Слайд 29Functioning of heart
The importance of calcium-dependent signaling in the heart
has been appreciated for decades. For example, it is well
accepted that intracellular calcium release from the sarcoplasmic reticulum (SR) is required for cardiac muscle contraction. Indeed, with each heart beat the calcium concentration in the cytosol of cardiac myocytes is elevated approximately 10-fold from a resting level of ∼100 nM to ∼1 μM.Presumably, a defect in signaling that prevents effective elevation of cytosolic calcium would impair contractility as the contraction of heart muscle is directly determined by the level of calcium elevation during systole. Similarly, a defect in the removal of calcium from the cytosol during diastole would impair cardiac relaxation, which is critically important in that it allows the heart chambers to refill with blood in preparation for the next beat.
Слайд 30Functioning of heart
Cardiac muscle fibers contract via excitation-contraction coupling, using
a mechanism unique to cardiac muscle called calcium-induced calcium release. CICR
is A process whereby calcium can trigger release of further calcium from the muscle sarcoplasmic reticulum.Слайд 31Functioning of heart
During stimulation of the muscle cell, the motor
neuron releases the neurotransmitter acetylcholine, which then binds to a
post-synaptic nicotinic acetylcholine receptor. The inward flow of calcium from the L-type calcium channels activates ryanodine receptors to release calcium ions from the sarcoplasmic reticulum.Слайд 32Functioning of heart
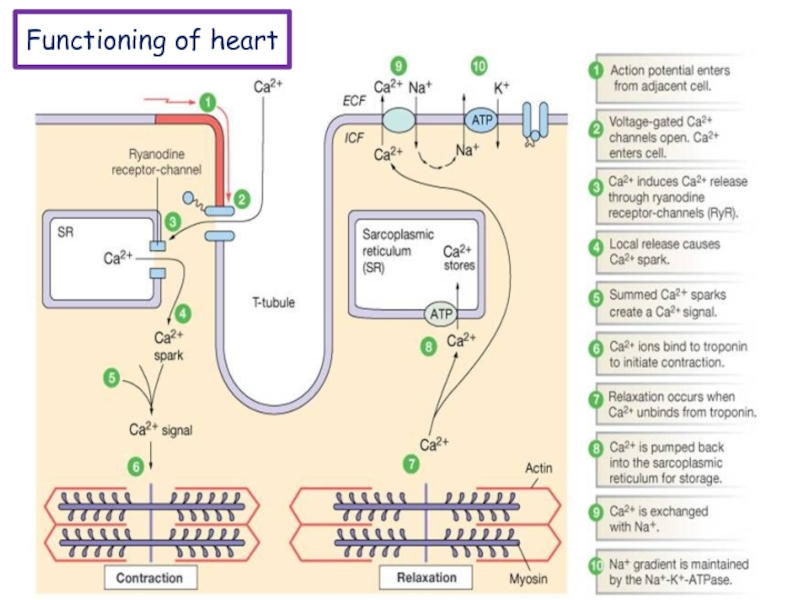
Excitation-contraction coupling describes the process of converting an
electrical stimulus (action potential) into a mechanical response (muscle contraction).
Calcium-induced calcium release involves the conduction of calcium ions into the cardiomyocyte, triggering further release of ions into the cytoplasm. Calcium prolongs the duration of muscle cell depolarization before repolarization occurs. Contraction in cardiac muscle occurs due to the binding of the myosin head to adenosine triphosphate (ATP), which then pulls the actin filaments to the center of the sarcomere, the mechanical force of contraction. In the sliding filament model, myosin filaments slide along actin filaments to shorten or lengthen the muscle fiber for contraction and relaxation
Слайд 33Functioning of heart
The pathway of contraction can be described in
five steps: An action potential, induced by the pacemaker cells in
the sinoatrial (SA) and atrioventricular (AV) nodes, is conducted to contractile cardiomyocytes through gap junctions. As the action potential travels between sarcomeres, it activates the calcium channels in the T-tubules, resulting in an influx of calcium ions into the cardiomyocyte. Calcium in the cytoplasm then binds to cardiac troponin-C, which moves the troponin complex away from the actin binding site. This removal of the troponin complex frees the actin to be bound by myosin and initiates contraction. The myosin head binds to ATP and pulls the actin filaments toward the center of the sarcomere, contracting the muscle.Intracellular calcium is then removed by the sarcoplasmic reticulum, dropping intracellular calcium concentration, returning the troponin complex to its inhibiting position on the active site of actin, and effectively ending contraction as the actin filaments return to their initial position, relaxing the muscle
Слайд 40Impact on cytoskeleton
Formation is regulated by actin-binding G-proteins
Cytoskeleton (actin)
*Profilin,
a protein that separates the actin monomers;
*G-proteins, rupturing actin filaments->
gelglin, vorsin, sverinin, adzeverin, destrin and cofilin;*Protein-> GCap39, blocking the ends of actin filaments;
*A-actinin, protein, cross-linking actin filaments.
PIP2
Phosphoinozitoldiphosphate
Polymerization
Ca2+
Depolymerization
Слайд 41Regulation of Ca2+ ions in blood
The main regulators of the
exchange of Ca2 + in the blood are parathyroid hormone,
calcitriol and calcitonin.Parathyroid hormone
Parathyroid hormone (PTH) is a single-chain polypeptide consisting of 84 amino acid residues (about 9.5 kD), whose action is aimed at increasing the concentration of calcium ions and reducing the concentration of phosphates in the blood plasma.
Слайд 42Regulation of Ca2+ ions in blood
Pre-parathyroid hormone (115 amino acids
)
ER
Signal peptide (25a.a) is cleaved
Pro-hormone
Pro-hormone
GA
Hormone maturation (84 a.a.)
N-terminal peptides containing 34 amino acid residues have complete biological activity and are secreted by glands along with mature parathyroid hormone. It is the N-terminal peptide that is responsible for binding to the receptors on the target cells. The role of the C-terminal fragment is not exactly established. The rate of hormone degradation decreases with a low concentration of calcium ions and increases if the concentration of calcium ions is high.
The secretion of PTH is regulated by the level of calcium ions in the plasma: the hormone is secreted in response to a decrease in the concentration of calcium in the blood
Слайд 43Regulation of Ca2+ ions in blood
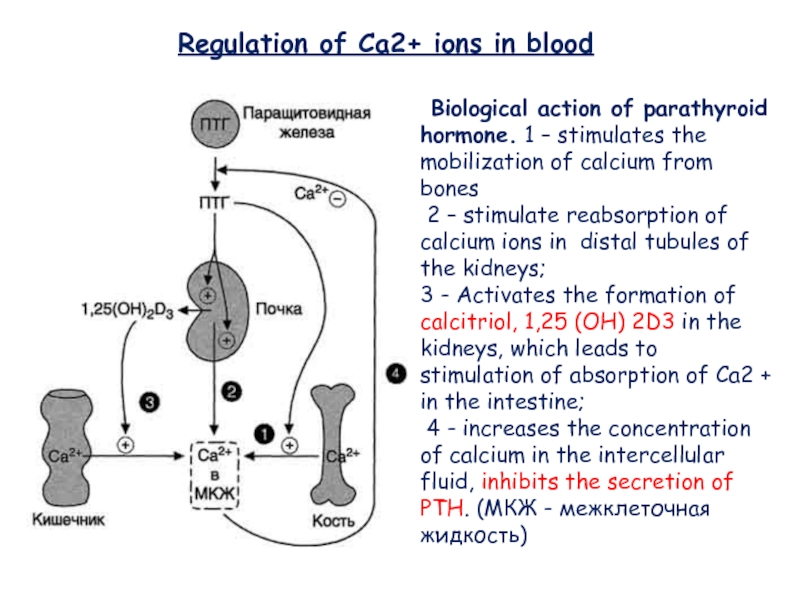
Biological action of parathyroid hormone. 1
– stimulates the mobilization of calcium from bones
2
– stimulate reabsorption of calcium ions in distal tubules of the kidneys;3 - Activates the formation of calcitriol, 1,25 (OH) 2D3 in the kidneys, which leads to stimulation of absorption of Ca2 + in the intestine;
4 - increases the concentration of calcium in the intercellular fluid, inhibits the secretion of PTH. (МКЖ - межклеточная жидкость)
Слайд 44Regulation of Ca2+ ions in blood
Calcitonin is a polypeptide consisting
of 32 amino acid residues with one disulfide bond. The
hormone is secreted by parafollicular K-cells of the thyroid gland or C-cells of parathyroid glands in the form of a high-molecular precursor protein. Secretion of calcitonin increases with increasing concentration of Ca2 + and decreases with decreasing Ca2 + concentration in the blood.Calcitonin is a parathyroid hormone antagonist.
It inhibits: 1) the release of Ca2 + from the bone, reducing the activity of osteoclasts.
2) inhibits tubular reabsorption calcium ions, stimulating their excretion by kidneys with urea.
*The rate of secretion of calcitonin in women strongly depends on the level of estrogens. With a lack of estrogens, the secretion of calcitonin decreases. This causes an acceleration of the mobilization of calcium from bone tissue, which leads to the development of osteoporosis.