Разделы презентаций
- Разное
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Геометрия
- Детские презентации
- Информатика
- История
- Литература
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
ENDOMETRIOSIS
Содержание
- 1. ENDOMETRIOSIS
- 2. ENDOMETRIOSISINTRODUCTION OF ENDOMETRIOSISSITESAETIOLOGYTHEORIES FOR ENDOMETRIOSISCLINICAL FEATURESCLASSIFIC ATION OF ENDOMETRIOSISPATHO-PHYSIOLOGYDIAGNOSIS OF ENDOMETRIOSISMANAGEMENT
- 3. Слайд 3
- 4. INTRODUCTION Endometriosis initially described by Von Rokitansky
- 5. SITES
- 6. Слайд 6
- 7. Слайд 7
- 8. Слайд 8
- 9. AETIOLOGYAge - 30-40 years(most common) - between
- 10. Theories for EndometriosisRetrograde menstruation (Sampson’s theory)Metaplasia of
- 11. Retrograde menstruation ( Samson’s Theory)John Sampson first
- 12. Слайд 12
- 13. Coelemic metaplasia( Mayer And Ivanol)In this theory,
- 14. Lymphatic Theory (vascular theory )
- 15. Genetic factorsThe risk or endometriosis is 7
- 16. Autoimmune theory In cellular immunity, can facilitate
- 17. Induction theory The induction theory is, in
- 18. Inflamation Substantial evidence suggests that endometriosis is
- 19. PathophysiologyEndometriosis is an estrogen-dependent condition.Estradiol concentration greater
- 20. Increased concentration of macrophages derived growth factors
- 21. Sign &SymptomsSIGNSTenderness in cul-de-sacNodularity in cul-de-sacFixed retroverted uterusAdnexal tendernessAdnexal massesSYMPTOMSDysmenorrhoeaDyspareuniaDeep seated pelvic painDysuriaDyscheziaHematuriaInfertility
- 22. Clinical FeaturesSymptoms:Pelvic- Dysmenorrhea(50%)
- 23. DysmenorrheaMost common symptomPain starts a few days
- 24. DyspareuniaIt is usually deep, due to stretching
- 25. InfertilityPresent in majority of the women with
- 26. DiagnosisRecommended that pelvic examination be performed at
- 27. Bimanual Pelvic ExaminationExaminationOn bimanual pelvic examination, fixed
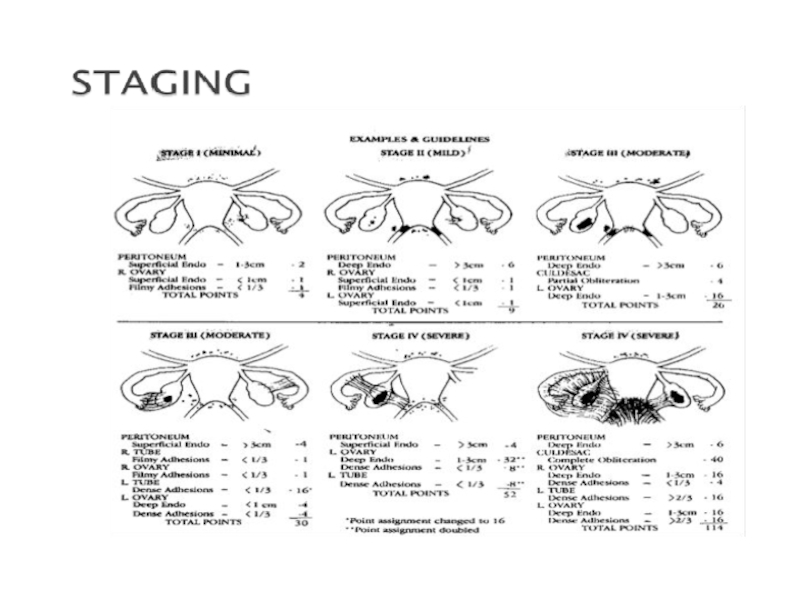
- 28. Classification
- 29. Слайд 29
- 30. DiagnosisInvestigationsLaparoscopy: Gold standard It should not be
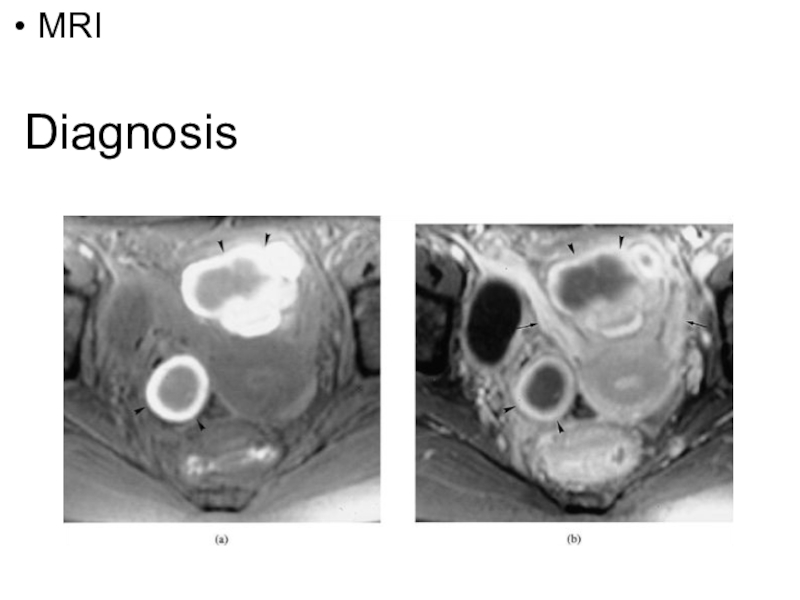
- 31. DiagnosisMRI
- 32. DiagnosisHistological Confirmation:Visual inspection is usually adequate but
- 33. Слайд 33
- 34. DiagnosisLaparoscopy (Sensitivity : 97%, Specificity 95%) Types
- 35. Слайд 35
- 36. Слайд 36
- 37. LAPROSCOPIC IMAGES :A )OLD ENDOMETRIOSIS (Blue/Grey) B )
- 38. Tranvaginal Ultrasound scanRetroverted uterus with obliteration of
- 39. Слайд 39
- 40. CA-125
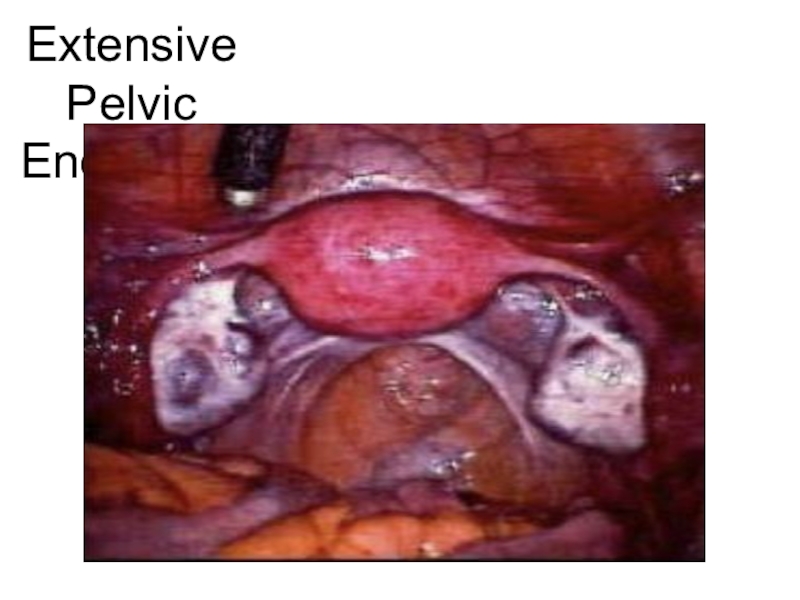
- 41. Extensive Pelvic Endometriosis
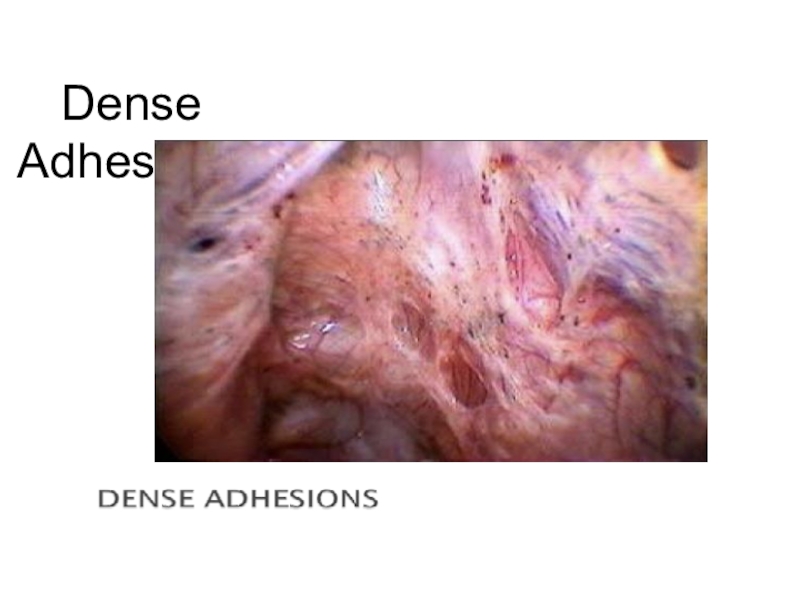
- 42. Dense Adhesions
- 43. DiagnosisSonographic Features :Endometritic cysts (oval or round)-
- 44. Differential Diagnosis Chronic PIDPostoperative adhesionsOld ectopic gestationPelvic congestion syndromeIrritable bowel syndromeDiverticulitisUlcerative colitisCrohn’s disease
- 45. Слайд 45
- 46. Drug Treatment Combined oral contraceptives:Administered intermittently or
- 47. Drug Treatment DanazolA synthetic derivative of ethinyl
- 48. Drug Treatment Gonadotropin releasing hormone:GnRH is administered
- 49. Minimal Invasive Surgery Aspiration of peritoneal fluid in cul-de-sac.Destruction of endometriotic implants
- 50. Minimal Invasive Surgery Role of surgery:u Failed
- 51. Слайд 51
- 52. Слайд 52
- 53. SurgeryIndications for surgery:Advanced stage of disease detectedLarge
- 54. Surgery Laparotomy:In advanced & larger lesions if
- 55. Combined Therapy Preoperative GnRH:monthly for 3 monthsreduces
- 56. ProphylaxisLow-dose OCP reduce the menstrual flow &
- 57. Слайд 57
- 58. Скачать презентанцию
ENDOMETRIOSISINTRODUCTION OF ENDOMETRIOSISSITESAETIOLOGYTHEORIES FOR ENDOMETRIOSISCLINICAL FEATURESCLASSIFIC ATION OF ENDOMETRIOSISPATHO-PHYSIOLOGYDIAGNOSIS OF ENDOMETRIOSISMANAGEMENT
Слайды и текст этой презентации
Слайд 2ENDOMETRIOSIS
INTRODUCTION OF ENDOMETRIOSIS
SITES
AETIOLOGY
THEORIES FOR ENDOMETRIOSIS
CLINICAL FEATURES
CLASSIFIC ATION OF ENDOMETRIOSIS
PATHO-PHYSIOLOGY
DIAGNOSIS OF
ENDOMETRIOSIS
Слайд 4INTRODUCTION
Endometriosis initially described by Von Rokitansky in 1860
Endometriosis is
a clinical and pathological entity.
It is characterized by the presence
of tissue resembling functional endometrial glands and stroma outside the uterine cavity.It is not a neoplastic condition, but malignant transformation is possible.
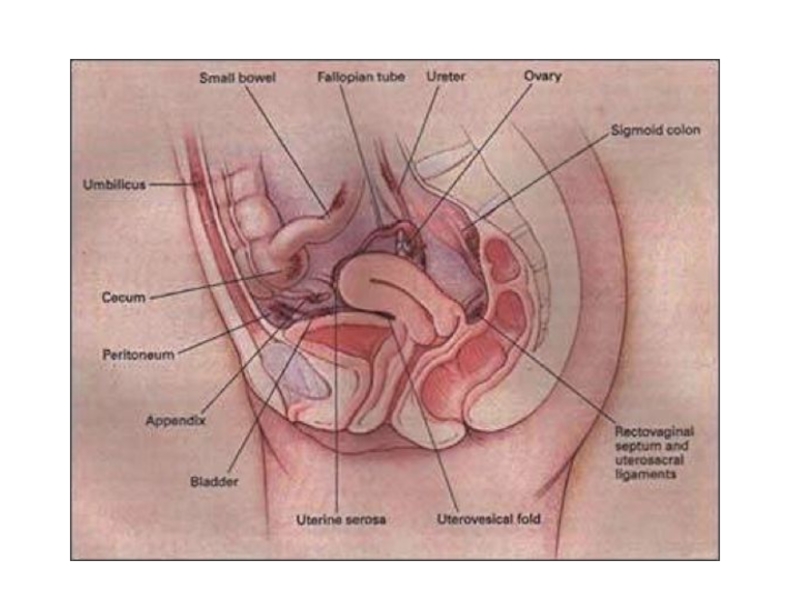
Слайд 5SITES
ABDOMINAL
Most common site - OVARY (44% involved)
Pouch of Douglas
Uterosacral ligament
Broad ligament
Rectovaginal septum
Pelvic lymph node
Rare sites - Gut, Appendix, Ureter, Urinary Bladder
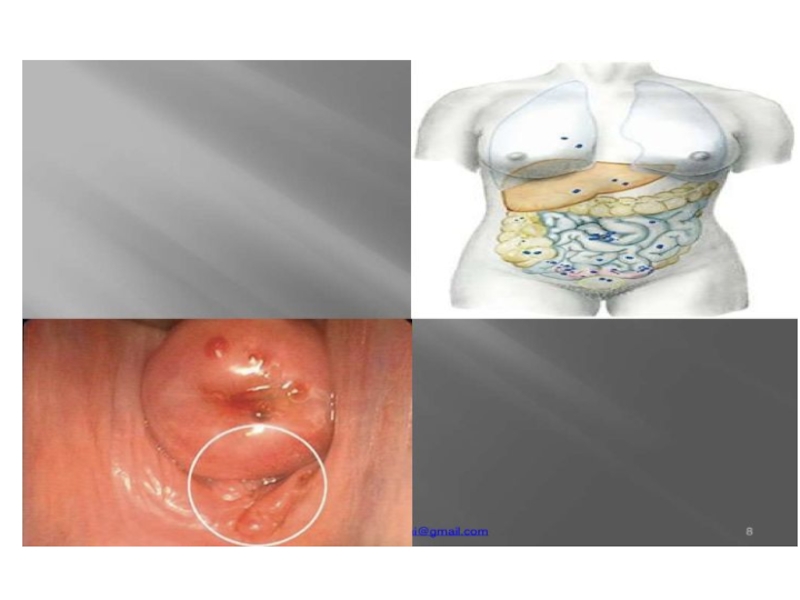
Слайд 7
Common sites
- Abdominal scar of Hysterotomy,
Caesarean Section,
Tubectomy,
Myomectomy
Umbilicus
Episiotomy Scar
Vagina
Cervix
Remote sites - Pleura, Lungs, deep tissues of arms, thighs
Слайд 9AETIOLOGY
Age - 30-40 years(most common) - between the menarche and
menopause.
Family history - 7 times greater if 1st degeneration affected
by endometriosis.New study - Early menarche
Social and Economic factors - more common in highly civilized communitis .
Parity- 50-70% affected women are childless.
Слайд 10Theories for Endometriosis
Retrograde menstruation (Sampson’s theory)
Metaplasia of coelomic epithelium (Meyer
and Ivanoff)
Lymphatic dissemination
Haematogenous Spread
Hereditary factor
Immunologic factor
Induction theory
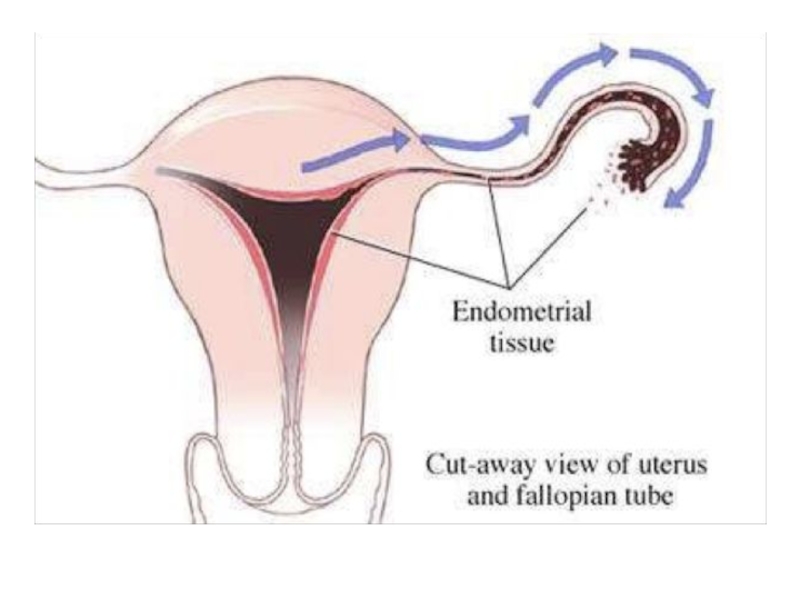
Слайд 11Retrograde menstruation ( Samson’s Theory)
John Sampson first postulated that endometriosis
arose from retrograde flow of fragments of endometrial tissue through
the oviducts and into the peritoneal cavity.Epidemiologic data suggests that women who menstruate more frequently, more heavily, or for a longer duration have increased chance of disease development.
There is retrograde flow of menstrual blood through the uterine tube during menstruation. The endometrial fragments get implanted in the peritoneal surface of pelvic organs( Sites– ovaries, uterosacral ligament)
Anomalies of the Mullerian tract, increased occurrence of endometriosis and stenosis of external cervical os.
Слайд 13Coelemic metaplasia( Mayer And Ivanol)
In this theory, the germinal epithelia
of the ovary, endometrium and peritoneum all originate from the
same totipotential coelomic epithelium.In coelomic Metaplasia, these totipotential coelomic cell are transformed by repeated exposure to hormonal or infection stimuli.
Development of endometriotic lesions in unusual locations.
Prolonged treatment with estrogen.
Слайд 15Genetic factors
The risk or endometriosis is 7 times greater if
a first- degree relative has been affected by endometriosis .
Multifactorial inheritance has been postulated.Monozygotic twins are markedly concordant for endometriosis.
A worldwide collaborative project (The Oxford Endometriosis Gene Study) has been organized to identify a genetic basis for endometriosis
Слайд 16Autoimmune theory
In cellular immunity, can facilitate the successful implantation
of translocated endometrial cells.
In endometriosis lymphocytes decreased cytotoxic response to
endometrial cell may be due to defect in natural killer cell activity, such as a decreased lytic effect toward stroma that allow ectopic development of endometrial fragments.There may be increased resistance of endometrium in women with endometriosis to natural killer cytotoxicity.
Слайд 17Induction theory
The induction theory is, in principle, an extension
of the coelomic metaplasia theory.
It proposes that an endogenous (undefined)
biochemical factor can induce undifferentiated peritoneal cells to develop into endometrial tissue.This theory has been supported by experiments in rabbitsbut has not been substantiated in women and primates.
Слайд 18Inflamation
Substantial evidence suggests that endometriosis is associated with a
state of subclinical peritoneal inflammation, marked by
↑ peritoneal fluid volume,
↑
peritoneal fluid white blood cell concentration↑ inflammatory cytokines, growth factors, and angiogenesis-promoting substances
Macrophages or other cells may promote the growth of endometrial cells by secretion of growth and angiogenic factors such as epidermal growth factor (EGF)
There is increasing evidence that local inflammation and secretion of prostaglandins (PG) is related to differences in endometrial aromatase activity between women with and without endometriosis
Слайд 19Pathophysiology
Endometriosis is an estrogen-dependent condition.
Estradiol concentration greater than 60pg/ml is
necessary for proliferation of endometrial lesions.
Estrogen & Progesterone receptors are
found in much lower concentrations in endometriotic tissue than in normal endometrial tissue,Growth factors can originate from the peritoneal environment to stimulate endometrial development.
Platelet derived growth factor, macrophage secretory
products enhance endometrial stromal cell proliferation.
Слайд 20Increased concentration of macrophages derived growth factors including vascular endothelial
growth factor.
Molecular alterations in steroidogenic enzyme function have been implicated
in the pathogenesis of endometriosis.Menstrual effluent contains factors that induce alterations in the peritoneal mesothelium, facilitating adhesions of endometrial cells.
Слайд 21Sign &Symptoms
SIGNS
Tenderness in cul-de-sac
Nodularity in cul-de-sac
Fixed retroverted uterus
Adnexal tenderness
Adnexal masses
SYMPTOMS
Dysmenorrhoea
Dyspareunia
Deep
seated pelvic pain
Dysuria
Dyschezia
Hematuria
Infertility
Слайд 22Clinical Features
Symptoms:
Pelvic- Dysmenorrhea(50%)
Abnormal menstruation(60%)
Dyspareunia,chronic
pelvic painPremenstrual Spotting
Gastrointestinal - Constipation,diarrhea, hematochezia, tenesmus.
Urinary complaint- Flank pain,back pain, abdominal pain,urgency frequency hematuria.
Pulmonary - Haemoptysis, pneumothorax
Infertility.
Слайд 23Dysmenorrhea
Most common symptom
Pain starts a few days prior to menstruation,
gets worse during menstruation( secondary dysmenorrhoea)
Pain due to Increased secretion
of PGF2α, Thromboxane β2 from endometriotic tissue.Abnormal Menstruation:
Menorrhagia is a predominant abnormality.
Polymennorhoea, premenstrual spotting also occur.
Слайд 24Dyspareunia
It is usually deep, due to stretching of the structures
of the Pouch of Douglas or direct contact tenderness found
in endometriosis of rectovaginal septum or Pouch of Douglas and with fixed retroverted uterus.Abdominal pain:
lower abdominal pain or backache
May be due to inflammation in peritoneal implants due to cystic bleeding
Irritation or invasion of nerve
Action of inflammatory cytokines released by the macrophages.
Слайд 25Infertility
Present in majority of the women with endometriosis.
Advanced disease, adhesions
and fixity results in structural damage to
tubes and ovaries à
impairs tubo-ovarian mobility.Ovarian problems: anovulation, luteinized unruptured follicle, oocyte maturation defects.
Tubal problem: altered tubal motility or ovum pick up.
Peritoneal factors: intraperitoneal inflammation
Sperm problems: phagocytosis by macrophages, inactivation by antibodies.
Endometrium: luteal phase defect, implantation defects
Слайд 26Diagnosis
Recommended that pelvic examination be performed at the time of
menses when tenderness is easier to detect.
The vulva, vagina, and
cervix should be inspected for any signs of endometriosis, although the occurrence of endometriosis in these areas is rare (e.g., episiotomy scar).The uterus is often in fixed retroversion, and the mobility of the ovaries and fallopian tubes is reduced.
Other possible signs of endometriosis include uterosacral or cul-de-sac nodularity, cervical displacement due to uterosacral scarring , painful swelling of the rectovaginal septum, and unilateral ovarian (cystic) enlargement.
Слайд 27Bimanual Pelvic Examination
Examination
On bimanual pelvic examination, fixed retroverted uterus, bilateral
pelvic tenderness, fixed or enlarged ovaries and painful uterosacral nodularity.
Deeply
infiltrating nodules are most reliably detected when clinical examination is performed during menstruation. Adenomyotic uterus is seldom > 12 weeks, soft, smooth & tender in contrast to fibroid uterus. Isolated adenomyoma can be differentiated by presence of localised tendernessСлайд 30Diagnosis
Investigations
Laparoscopy: Gold standard It should not be performed within 3
months of hormonal treatment to prevent under diagnosis
Ultrasound: Ultrasound has
a limited role, however the addition of colour doppler claims to increase the sensitivity to 91.8%, specificity of 91.3%MRI –useful
Ca 125-Maybe elevated in severe
Слайд 32Diagnosis
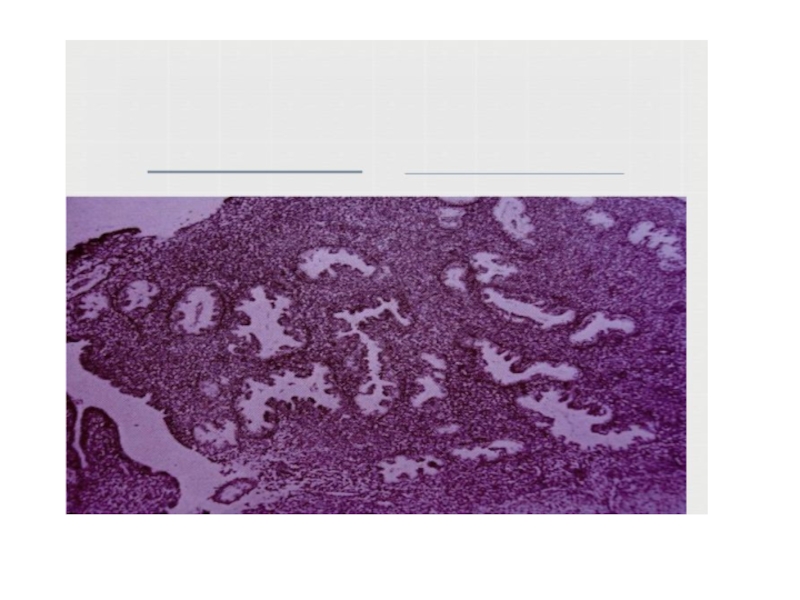
Histological Confirmation:
Visual inspection is usually adequate but histological confirmation of
at least one lesion is ideal.
In cases of ovarian endometrioma
>3 cm in diameter and in deeply infiltrating disease, histology is a must to rule out malignancy.Слайд 34Diagnosis
Laparoscopy (Sensitivity : 97%, Specificity 95%) Types of lesions on
laparoscopy:
Powder burn or black lesions White opacified peritoneum Glandular excrescences
Flame like red lesionsPeritoneal pockets or windows
Clear vesicles
Yellow brown patches
Unexplained adherence of ovary to peritoneum of ovarian fossa
Encysted collection of thick chocolate coloured or tarry fluids
Adhesions to posterior lip of broad ligaments/other pelvic structures
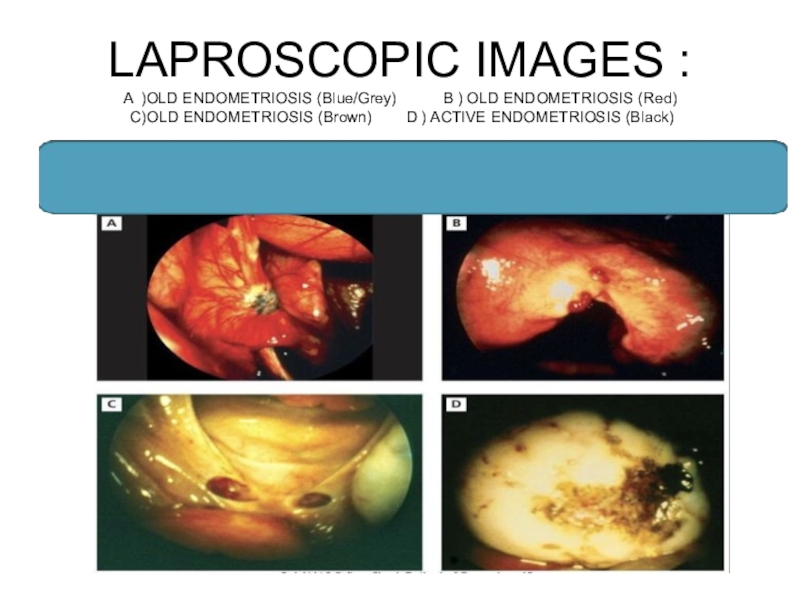
Слайд 37LAPROSCOPIC IMAGES :
A )OLD ENDOMETRIOSIS (Blue/Grey) B ) OLD ENDOMETRIOSIS (Red)
C)OLD ENDOMETRIOSIS (Brown) D ) ACTIVE ENDOMETRIOSIS (Black)
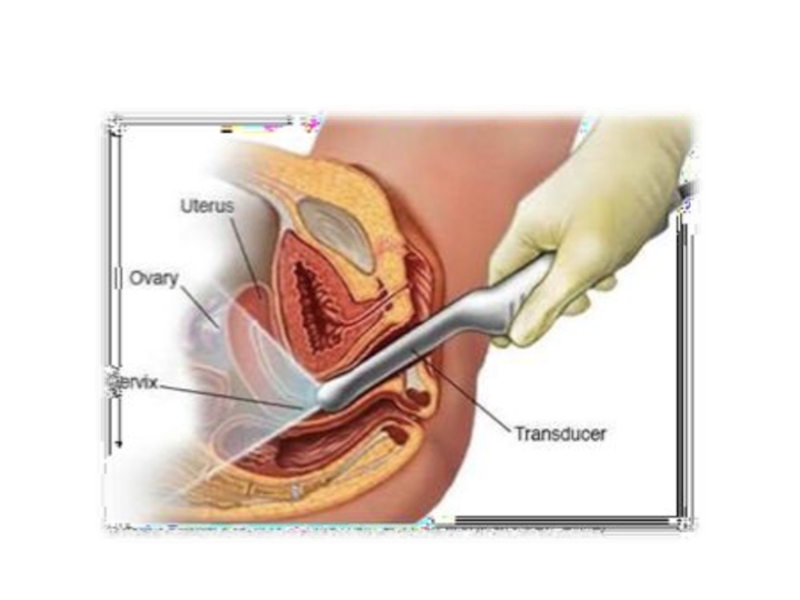
Слайд 38Tranvaginal Ultrasound scan
Retroverted uterus with obliteration of cul-de-sac & B\L
complex adnexal masses maybe suggestive.
Helps to differentiate endometrial cysts from
other complex cysts like dermoids:Endometrial cyst: low level internal echoes with posterior acoustic enhancement – Ground glass appearance.
Dermoid: posterior acoustic shadowing d/t presence of bone & teeth in cyst. Presence of mural nodule & “pins and needle”.
Слайд 43Diagnosis
Sonographic Features :
Endometritic cysts (oval or round)- capsulated, fine homogeneous,
uniform, granular echoes, anechoic, single or multiple, unilateral or bilateral
On
Doppler: no vascularity within the mass Ovarian adhesions to uterusFree floating fimbria on sonosalpingography
Слайд 44Differential Diagnosis
Chronic PID
Postoperative adhesions
Old ectopic gestation
Pelvic congestion syndrome
Irritable bowel
syndrome
Diverticulitis
Ulcerative colitis
Crohn’s disease
Слайд 46Drug Treatment
Combined oral contraceptives:
Administered intermittently or continuously.
High Incidence of
side effects & risk of thrombus-embolism limit their prolonged use.
Seasonal
OC for 84 days , with 6 days tablet free, reduce the menstrual periods to just four cycles in a year.Oral progestogens:
Exert an anti-oestrogenic effect and their continuous administration causes decidualization and endometrial atrophy.
Norethisterone 5.0 – 20.0mg daily or Dydrogesterone 10 -30mg daily.
This hormone does not prevent ovulation and is suitable for a woman
trying to conceive.
Слайд 47Drug Treatment
Danazol
A synthetic derivative of ethinyl testosterone,
Mildly anabolic ,
anti-oestrogenic and anti-progestational
200-800mg daily for 3-6 months starting on first
day of menses.S/E: wt. gain, hirsutism, excessive sweating, muscle cramps,
depression, atrophy of breasts & vaginal epithelium.
Aromatase inhibitors:
Letrozole(2.5mg), anastrozole(1-2mg) daily for 6 months.
Anti-oestogenic & prevent conversion of androgen to oestrogen.
Should be given with Vitamin D and Calcium to prevent osteoporosis.
Nausea , vomiting and diarrhea are other side effects.
Слайд 48Drug Treatment
Gonadotropin releasing hormone:
GnRH is administered continuously to down
regulate and suppress pituitary gonadotropins .
It causes atrophy of endometriotic
tissue.The synthetic analogue of GnRH is given in doses of 10-20mg
intravenously twice daily.
Prolonged GnRH therapy over 6months causes hypo-oestrogenism & menopausal symptoms such as hot flushes, dry vagina, urethral syndrome and osteoporosis.
RU-486:
Tried at a dose of 50mg daily for 3months.
Reduces pain and delay recurrences.
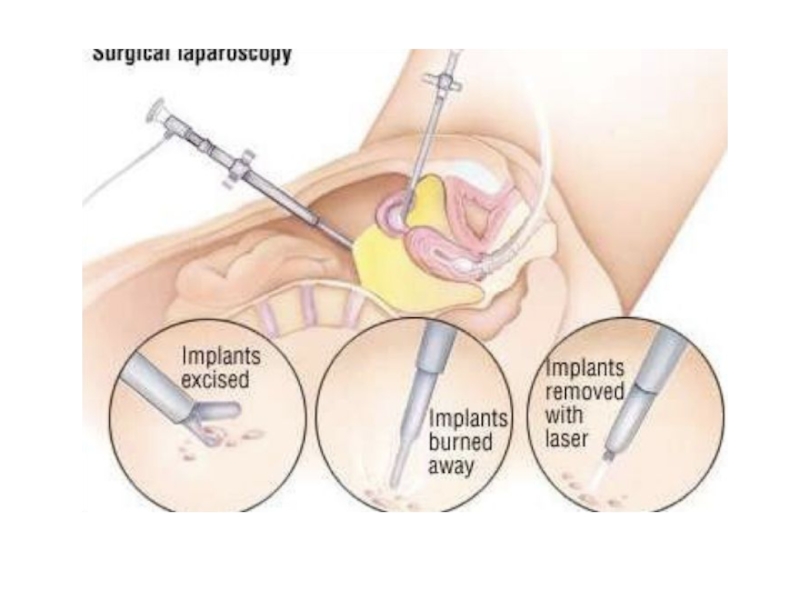
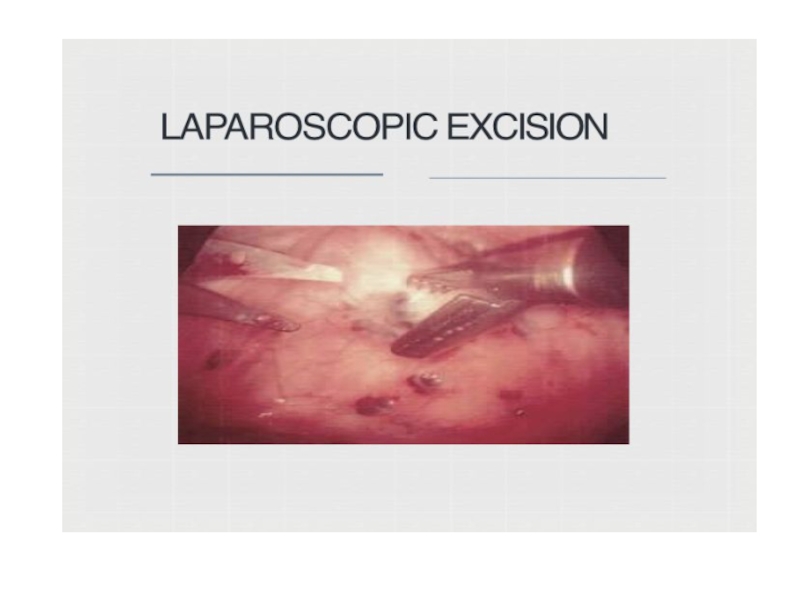
Слайд 49Minimal Invasive Surgery
Aspiration of peritoneal fluid in cul-de-sac.
Destruction of endometriotic
implants
Nd:YAG laser.Larger lesions and chocolate cyst can be excised. Residual lesion can be dealt with by hormonal therapy. Cauterization of cyst wall – young females.
Слайд 50Minimal Invasive Surgery
Role of surgery:
u Failed Medical therapy
u Infertility
u
Recurrence
u Chocolate cyst ovary
Laparoscopic breaking of adhesions in pelvis relieves
dysmenorrhea and pelvic pain.LUNA (Laser uterosacral nerve ablation) for midline pain.
Prolapse of genital tract & bladder dysfunction is noted with LUNA.
Слайд 53Surgery
Indications for surgery:
Advanced stage of disease detected
Large lesion
Medical therapy fails
or intolerable
Recurrence occurs
In elderly parous women
Aim:
Coagulation of peritoneal endometrial lesions
Adhesiolysis
Fenestration
& drainage of small ovarian endometriomas <3cm diameter. Cystectomy- >3cm.Слайд 54Surgery
Laparotomy:
In advanced & larger lesions if medical therapy fails.
Dissection
and excision of a chocolate cyst.
Salpingo-oophorectomy
Abdominal hysterectomy and bilateral salpingo-oophorectomy.
Premenopausal
woman may need HRT after radical surgery.HRT following bilateral ovarian removal in young women may be prescribed under strict monitoring, as a risk for recurrence remains.
Total hysterectomy & B/L oophorectomy- women with severe
symptoms & those with fertility is not a problem.
Слайд 55Combined Therapy
Preoperative GnRH:
monthly for 3 months
reduces size & extend
of lesions,
softens adhesions
makes subsequent surgery more easier & complete.
Postoperative hormonal
therapy:When surgery is incomplete or some residual lesion is left behind.
Слайд 56Prophylaxis
Low-dose OCP reduce the menstrual flow & protect against endometriosis.
3 monthly OCP’s are convenient to take & effective.
Tubal patency
tests should be avoided in immediate premenstrual phase to avoid spill.Operations on genital tract should be scheduled in postmenstrual period.