Разделы презентаций
- Разное
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Геометрия
- Детские презентации
- Информатика
- История
- Литература
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
Malaria (Febris intermittens)
Содержание
- 1. Malaria (Febris intermittens)
- 2. OverviewIntroductionEtiology, epidemiologyPathogenesisClinical features Complications Diagnosis TreatmentPrevention
- 3. Malaria is a life-threatening disease caused
- 4. Between 2010 and 2015, malaria incidence
- 5. Слайд 5
- 6. Слайд 6
- 7. Malaria in Kyrgyzstan in 1923-20020,0010,010,11101001000100001923192619291932193519381941194419471950195319561959196219651968197119741977198019831986198919921995Fighting periodLiquidation period
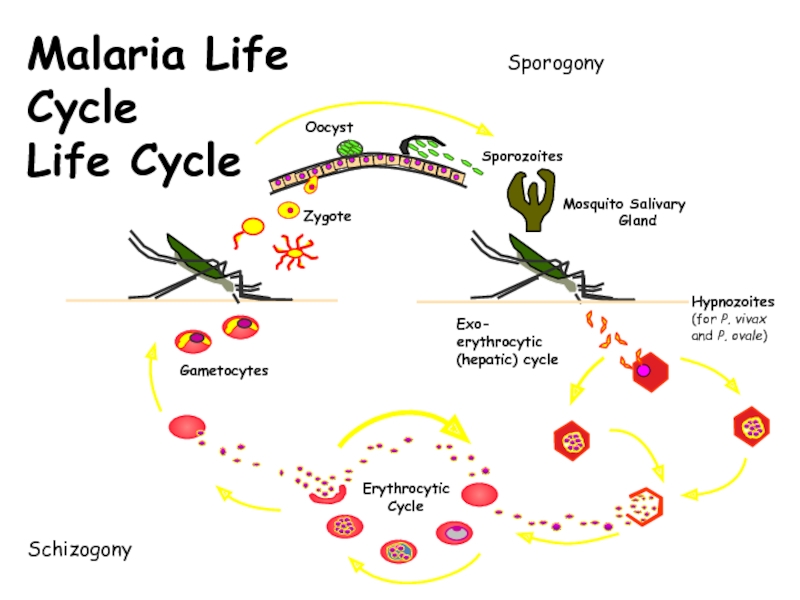
- 8. Exo-erythrocytic (hepatic) cycleMalaria Life CycleLife CycleSchizogonySporogony
- 9. Слайд 9
- 10. Plasmodium spp. (Malaria)Pathology and clinical significance:When merozoits
- 11. Слайд 11
- 12. Clinical presentationEarly symptomsHeadacheMalaiseFatigueNauseaMuscular painsSlight diarrheaSlight fever, usually not intermittentCould mistake for influenza or gastrointestinal infection
- 13. Malarial ParoxysmProdrome 2-3 days beforeMalaise, fever,fatigue, muscle
- 14. Types of InfectionsRecrudescenceexacerbation of persistent undetectable parasitemia,
- 15. Clinical presentationVaries in severity and courseParasite factorsSpecies
- 16. Malarial ParoxysmPeriodicityDays 1 and 3 for P.v.,
- 17. paroxysms associated with synchrony of merozoite releasebetween
- 18. Presentation of P.vivaxMost people of West African
- 19. Incubation period in non-immunes 12-17 days but
- 20. Слайд 20
- 21. Lack classical paroxysm followed by asymptomatic periodHeadache,
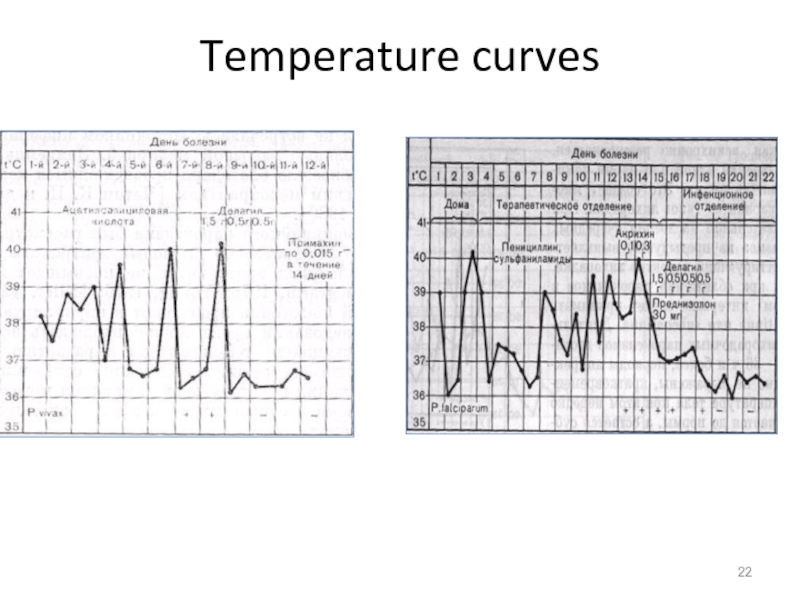
- 22. Temperature curves
- 23. Complication: Coma - brain edema, disturbance of
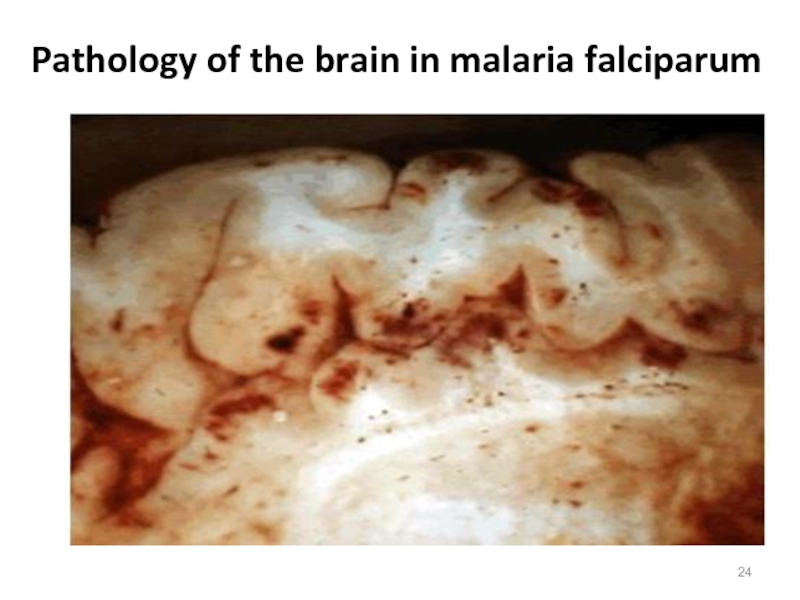
- 24. Pathology of the brain in malaria falciparum
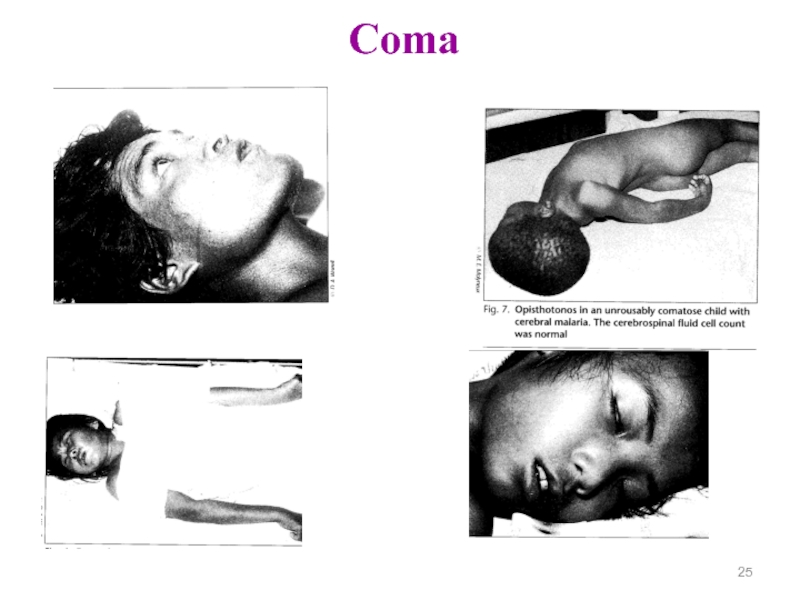
- 25. Coma
- 26. Malaria in pregnant womenAbortionPremature birthsNeonatal complicationsDeaths.Often develop
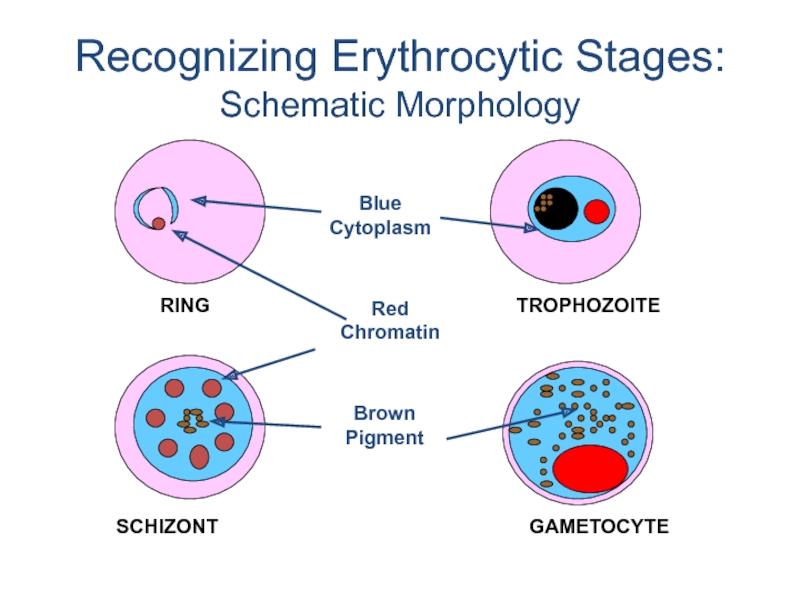
- 27. Recognizing Erythrocytic Stages: Schematic Morphology
- 28. Parasitemia and clinical correlates
- 29. Parasitemia and clinical correlates*WHO criteria for severe
- 30. Слайд 30
- 31. Слайд 31
- 32. Слайд 32
- 33. Слайд 33
- 34. Слайд 34
- 35. Слайд 35
- 36. Malaria Serology – antibody detectionImmunologic assays to
- 37. Malaria Serology – antibody detectionValuable epidemiologic tool
- 38. Polymerase Chain Reaction (PCR)Molecular technique to identify
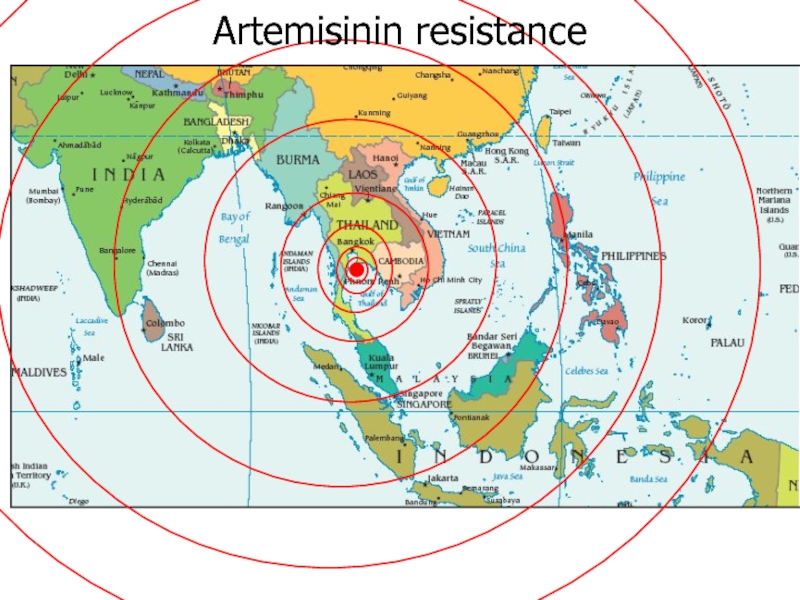
- 39. Artemisinin resistance
- 40. Скачать презентанцию
Слайды и текст этой презентации
Слайд 1 Malaria
(Febris intermittens)
Department of Infectious Diseases
Prepared by Professor
Kutmanova A.Z.
Слайд 2Overview
Introduction
Etiology, epidemiology
Pathogenesis
Clinical features
Complications
Diagnosis
Treatment
Prevention
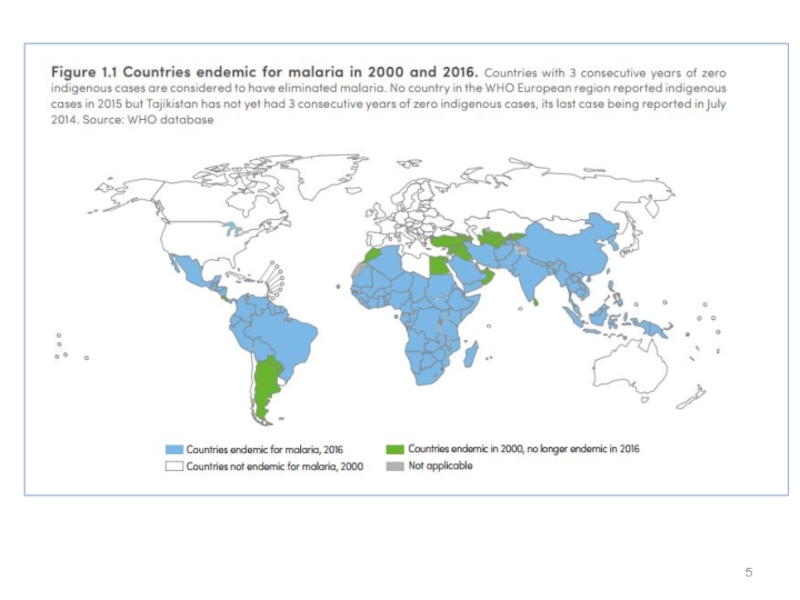
Слайд 3 Malaria is a life-threatening disease caused by parasites that
are transmitted to people through the bites of infected female Anopheles mosquitoes.
In 2015, 91 countries and areas had ongoing malaria transmission.Malaria is preventable and curable, and increased efforts are dramatically reducing the malaria burden in many places.
Слайд 4 Between 2010 and 2015, malaria incidence among populations at
risk (the rate of new cases) fell by 21% globally.
In that same period, malaria mortality rates among populations at risk fell by 29% globally among all age groups, and by 35% among children under 5.The WHO African Region carries a disproportionately high share of the global malaria burden. In 2015, the region was home to 90% of malaria cases and 92% of malaria deaths.
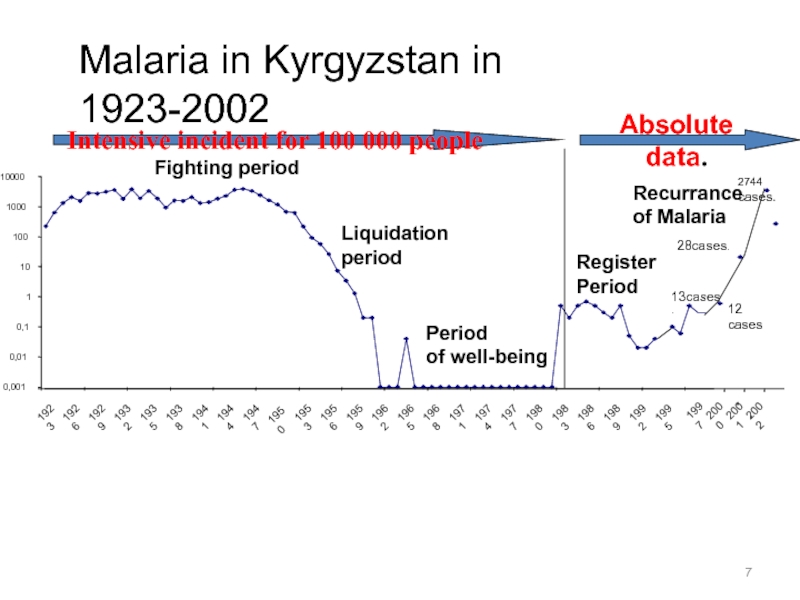
Слайд 7Malaria in Kyrgyzstan in 1923-2002
0,001
0,01
0,1
1
10
100
1000
10000
1923
1926
1929
1932
1935
1938
1941
1944
1947
1950
1953
1956
1959
1962
1965
1968
1971
1974
1977
1980
1983
1986
1989
1992
1995
Fighting period
Liquidation
period
Period
of
well-being
Register
Period
2000
1997
2001
2002
Recurrance
of Malaria
2744 сases.
28сases.
12 сases
13сases.
Intensive incident for 100 000
peopleAbsolute data.
Слайд 10Plasmodium spp. (Malaria)
Pathology and clinical significance:
When merozoits invade the blood
cells, using hemoglobin as a nutrient, eventually, the infected red
cells rupture, releasing merozoits that can invade other erythrocytes. If a large numbers of red cells rupture at roughly the same time, a paroxysm (sudden onset) of fever can result from the massive release of toxic substance.Plasmodium falciparum is the most dangerous species.
P. malriae, P. vivax, and P. ovale cause milder form of the disease, probably because they invade either young or old red cells, but not both. This is in contrast to P. falciparum, which invades cells of all ages.
Plasmodium falciparum is characterized by persistent high fever and orthostatic hypertension. Infection can lead to capillary obstruction and death if treatment is not introduced.
Слайд 12Clinical presentation
Early symptoms
Headache
Malaise
Fatigue
Nausea
Muscular pains
Slight diarrhea
Slight fever, usually not intermittent
Could mistake
for influenza or gastrointestinal infection
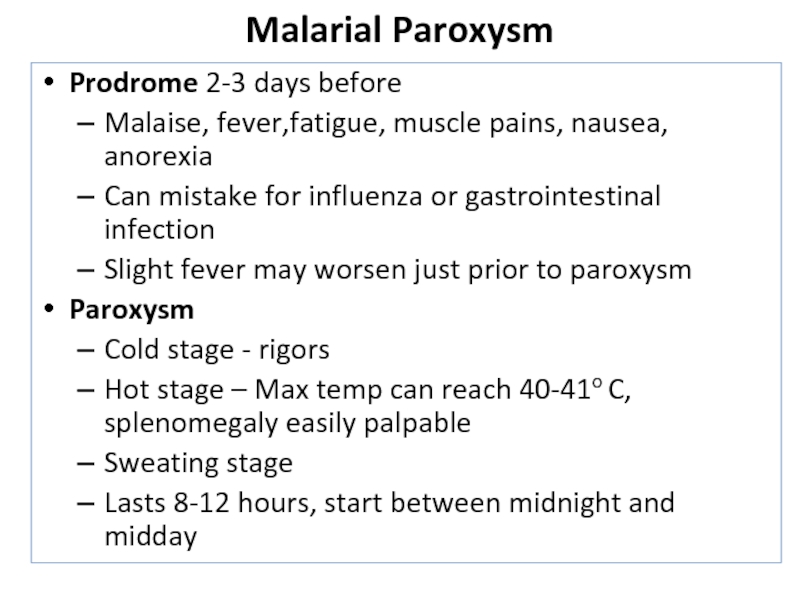
Слайд 13Malarial Paroxysm
Prodrome 2-3 days before
Malaise, fever,fatigue, muscle pains, nausea, anorexia
Can
mistake for influenza or gastrointestinal infection
Slight fever may worsen just
prior to paroxysmParoxysm
Cold stage - rigors
Hot stage – Max temp can reach 40-41o C, splenomegaly easily palpable
Sweating stage
Lasts 8-12 hours, start between midnight and midday
Слайд 14Types of Infections
Recrudescence
exacerbation of persistent undetectable parasitemia, due to survival
of erythrocytic forms, no exo-erythrocytic cycle (P.f., P.m.)
Relapse
reactivation of hypnozoites
forms of parasite in liver, separate from previous infection with same species (P.v. and P.o.)Recurrence or reinfection
exo-erythrocytic forms infect erythrocytes, separate from previous infection (all species)
Can not always differentiate recrudescence from reinfection
Слайд 15Clinical presentation
Varies in severity and course
Parasite factors
Species and strain of
parasite
Geographic origin of parasite
Size of inoculum of parasite
Host factors
Age
Immune
statusGeneral health condition and nutritional status
Chemoprophylaxis or chemotherapy use
Mode of transmission
Mosquito
Bloodborne, no hepatic phase (transplacental, needlestick, transfusion, organ donation/transplant)
Слайд 16Malarial Paroxysm
Periodicity
Days 1 and 3 for P.v., P.o., (and P.f.)
- tertian
Usually persistent fever or daily paroxyms for P.f.
Days 1
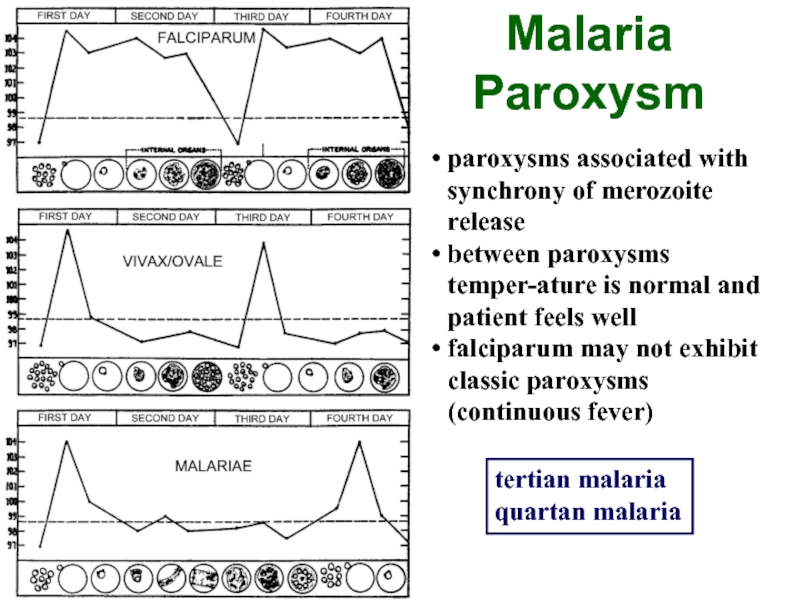
and 4 for P.m. - quartianСлайд 17paroxysms associated with synchrony of merozoite release
between paroxysms temper-ature is
normal and patient feels well
falciparum may not exhibit classic
paroxysms (continuous fever)Malaria Paroxysm
tertian malaria
quartan malaria
Слайд 18Presentation of P.vivax
Most people of West African descent are resistant
to P.v.
Lack Duffy blood group antigens needed for RBC invasion
Mild
– severe anemia, thrombocytopenia, mild jaundice, tender hepatosplenomegalySplenic rupture carries high mortality
Headache, dizziness, muscle pain, malaise, anorexia, nausea, vague abdominal pain, vomiting
Fever constant or remittent
Слайд 19Incubation period in non-immunes 12-17 days but can be 8-9
months or longer
Some strains from temperate zones show longer incubation
periods, 250-637 daysFirst presentation of imported cases – 1 month – over 1 year post return from endemic area
Relapses
60% untreated or inadequately treated will relapse
Time from primary infection to relapse varies by strain
Treat blood stages as well as give terminal prophylaxis for hypnozoites
Presentation of P.vivax
Слайд 21Lack classical paroxysm followed by asymptomatic period
Headache, dizziness, muscle pain,
malaise, anorexia, nausea, vague abdominal pain, vomiting
Fever constant or remittent
Postural
hypotension, jaundice, tender hepatosplenomegalyCan progress to severe malaria rapidly in non-immune patients
Cerebral malaria can occur
Parasites can sequester in tissues, not detected on peripheral smear
Presentation of P.falciparum
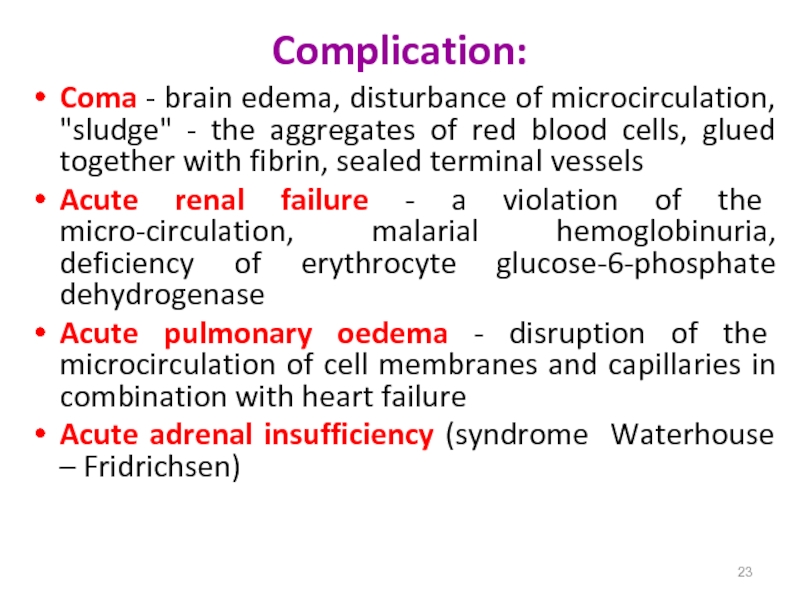
Слайд 23Complication:
Coma - brain edema, disturbance of microcirculation, "sludge" -
the aggregates of red blood cells, glued together with fibrin,
sealed terminal vesselsAcute renal failure - a violation of the micro-circulation, malarial hemoglobinuria, deficiency of erythrocyte glucose-6-phosphate dehydrogenase
Acute pulmonary oedema - disruption of the microcirculation of cell membranes and capillaries in combination with heart failure
Acute adrenal insufficiency (syndrome Waterhouse – Fridrichsen)
Слайд 26Malaria in pregnant women
Abortion
Premature births
Neonatal complications
Deaths.
Often develop severe anemia.
Often
observed the birth of premature infants and cases of stillbirth
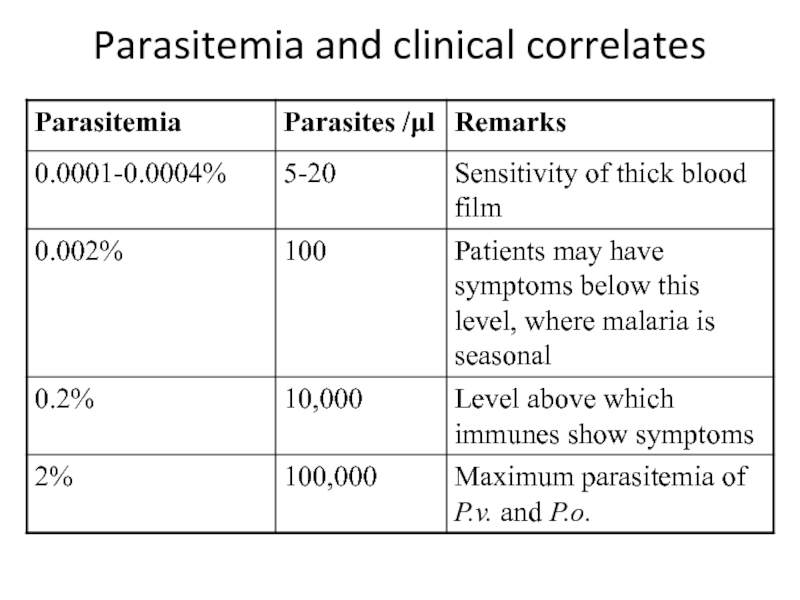
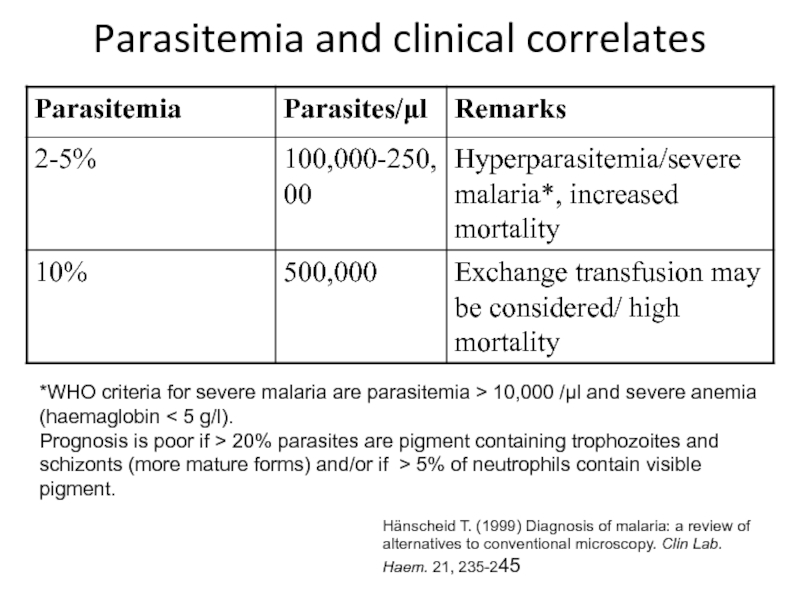
Слайд 29Parasitemia and clinical correlates
*WHO criteria for severe malaria are parasitemia
> 10,000 /l and severe anemia (haemaglobin < 5 g/l).
Prognosis
is poor if > 20% parasites are pigment containing trophozoites and schizonts (more mature forms) and/or if > 5% of neutrophils contain visible pigment.Hänscheid T. (1999) Diagnosis of malaria: a review of alternatives to conventional microscopy. Clin Lab. Haem. 21, 235-245
Слайд 36Malaria Serology – antibody detection
Immunologic assays to detect host response
Antibodies to asexual parasites appear some days after invasion of
RBCs and may persist for monthsPositive test indicates past infection
Not useful for treatment decisions
Слайд 37Malaria Serology – antibody detection
Valuable epidemiologic tool in some settings
Useful
for
Identifying infective donor in transfusion-transmitted malaria
Investigating congenital malaria, esp. if
mom’s smear is negativeDiagnosing, or ruling out, tropical splenomegaly syndrome
Retrospective confirmation of empirically-treated non-immunes
Слайд 38Polymerase Chain Reaction (PCR)
Molecular technique to identify parasite genetic material
Uses
whole blood collected in anticoagulated tube (200 µl) or directly
onto filter paper (5 µl)100% DNA is extracted
10% blood volume used in PCR reaction