Разделы презентаций
- Разное
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Геометрия
- Детские презентации
- Информатика
- История
- Литература
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
Physiological Changes in Pregnancy
Содержание
- 1. Physiological Changes in Pregnancy
- 2. Introductory CommentsThis lecture/presentation is a “work in
- 3. Physiological Adaptations to PregnancyNumerous normal changes in
- 4. Weight Gain in PregnancyNormal weight gain can
- 5. Weight Gain in Pregnancy
- 6. Weight Gain in Pregnancy
- 7. Breast Changes Increased blood flow to breastsIncreased sizeIncreased ductal growth, alveolar enlargementColustrum productionLactation dependent onEstrogenProgesteroneProlactinCortisolInsulin
- 8. Musculoskeletal Changes in PregnancyLigament laxity throughoutProgressively more
- 9. Skin Changes Vascular spidersPalmar erythemaStriae gravidarumHyperpigmentation effectsLinea
- 10. Gastrointestinal ChangesKey ChangesAppetite
- 11. Common GI Changes in PregnancyNausea and vomiting
- 12. Physiological GI Changes.The hormonal effects on the
- 13. Physiological GI ChangesRecent studies, however, have shed
- 14. Hepatic Function Laboratory Studies
- 15. Hematological Changes in PregnancyPlasma volume increases early
- 16. More Hematological Changes Occurring During PregnancyPregnancy considered
- 17. Pulmonary AdaptationsAnatomicalIncreased chest diameter, subcostal angle changes,
- 18. Ventilation and Respiratory Gases.A progressive increase in
- 19. Ventilation and Respiratory Gases.Arterial and alveolar carbon
- 20. Ventilation and Respiratory GasesOxygen consumption increases gradually
- 21. Cardiac Changes in PregnancyCardiac output increases around
- 22. Key Cardiovascular Changes During Pregnancy
- 23. Blood VolumeBlood Volume increases progressively from 6-8
- 24. Blood VolumeThe increased blood volume serves two
- 25. Blood Constituents.As mentioned above, red cell mass
- 26. Cardiac OutputCardiac Output increases to a similar
- 27. Cardiac OutputDuring labor, further increases are seen
- 28. Cardiac Size/Position/ECG.There are both size and position
- 29. Blood Pressure. Systemic arterial pressure is never
- 30. Renal Changes in PregnancyMinimal renal enlargement, bilaterallyBoth
- 31. More Renal Changes in PregnancyGFR increases 50%
- 32. Endocrine Changes with PregnancyCarbohydrate MetabolismOverall effect is
- 33. MetabolismAll metabolic functions are increased during pregnancy
- 34. MetabolismCarbohydrate metabolism, however, demonstrates the most dramatic
- 35. Hypoglycaemia.Optimal blood glucose levels in pregnant women
- 36. Hypoglycaemia.Hypoglycaemia initiates the release of glucagon, cortisol
- 37. Endocrine Changes in Pregnancy Thyroid Function in
- 38. Endocrine Changes in PregnancyGnRH concentration increases
- 39. Endocrinology Changes in Pregnancy
- 40. Endocrine Changes in PregnancyThe placenta produces a
- 41. Endocrine Changes in PregnancyThe placenta produces corticotropin-releasing
- 42. Endocrine Changes in PregnancyThe placenta produces melanocyte-stimulating
- 43. Endocrine Changes in PregnancyEffects of thyroid hormone
- 44. Endocrine Changes in PregnancyThe pituitary gland enlarges
- 45. Скачать презентанцию
Introductory CommentsThis lecture/presentation is a “work in progress”Not possible to cover “all” the changes that occur during pregnancy!We will highlight some of the important changes that occur, affecting some of the
Слайды и текст этой презентации
Слайд 2Introductory Comments
This lecture/presentation is a “work in progress”
Not possible to
cover “all” the changes that occur during pregnancy!
We will highlight
some of the important changes that occur, affecting some of the major organ systemsKey concept: one needs to know “normal” to be able to diagnose and manage the common problems in pregnancy!
This may be of personal importance some day!
Слайд 3Physiological Adaptations to Pregnancy
Numerous normal changes in response to pregnancy
It
is important to have an awareness of what is considered
“normal” in pregnancySuch awareness allows an obstetrician to diagnose and manage common medical problems such as
Hypertension
Hyperthyroidism
Anemia
Acute appendicitis or acute cholecystitis
Peripartum cardiomyopathy
Mitral stenosis
Asthma
Gestational diabetes or Insulin dependent diabetes
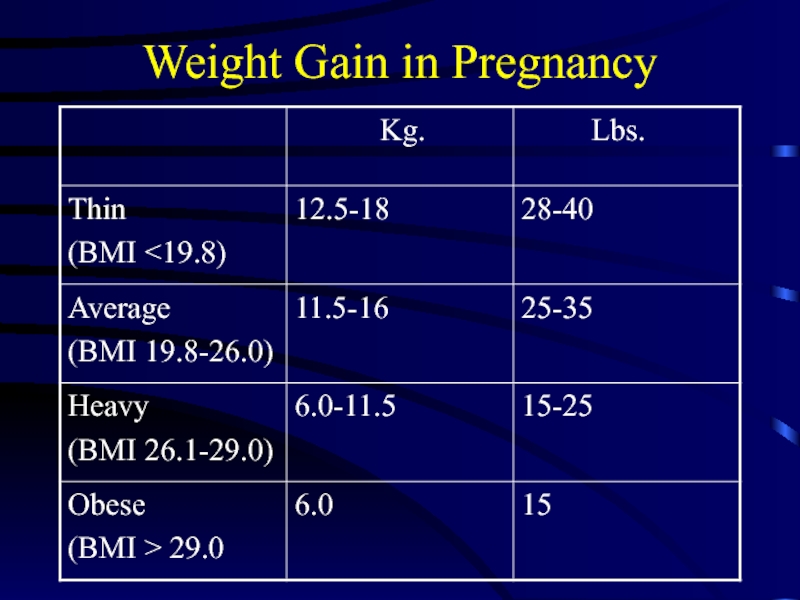
Слайд 4Weight Gain in Pregnancy
Normal weight gain can be 30-35 lbs
in average patient and 50-70 lbs. in twin pregnancy
Daily requirements
of 2000-2500 caloriesAssociated with good outcome, ie delivery of normal sized baby
Excess weight gain associated with variety of complications:
GDM, pre-eclampsia, macrosomia
Total pregnancy expenditure is 75,000kcalories
Recommendations for appropriate weight gain in pregnancy based on initial weight, BMI
Слайд 7Breast Changes
Increased blood flow to breasts
Increased size
Increased ductal growth, alveolar
enlargement
Colustrum production
Lactation dependent on
Estrogen
Progesterone
Prolactin
Cortisol
Insulin
Слайд 8Musculoskeletal Changes in Pregnancy
Ligament laxity throughout
Progressively more bothersome backpain not
uncommon
“Pride of pregnancy”
Total calcium levels decreased but ionized calcium levels
normalIncreased PTH
Increased relaxin
No loss of bone density during pregnancy
Слайд 9Skin Changes
Vascular spiders
Palmar erythema
Striae gravidarum
Hyperpigmentation effects
Linea nigra
Mask of pregnancy
Increased fine
hair growth while pregnant
Pruritus at end of pregnancy with cholestasis
Слайд 10 Gastrointestinal Changes
Key Changes
Appetite
Usually increased, with cravings
Gastric Reflux Sphincter relaxation
GI Motility
DecreasedGI Transit Time Slower
Liver Functionally unchanged
Gallbladder Dilated
Слайд 11Common GI Changes in Pregnancy
Nausea and vomiting of pregnancy or
“morning sickness”
Exact etiology is unknown
Supportive therapy usually helpful
On rare occasion,
TPN and hyperalimentation necessaryDietary cravings commonplace
Pica
Ptyalism
Increased tendency for gallbladder dysfunction with possible need for surgery, or laporoscopic cholecystectomy
Слайд 12Physiological GI Changes.
The hormonal effects on the gastrointestinal tract are
an issue of debate among anaesthetists. Relaxation of the lower
oesophageal sphincter has been described, but there have been differing views about the effect on motility of the gastrointestinal tract and the times at which it is most prominent. Many believe that there is also retardation of gastrointestinal motility and gastric emptying, producing increased gastric volume with decreased pH, beginning as early as 8-10 weeks of gestation.Слайд 13Physiological GI Changes
Recent studies, however, have shed a different light
on the subject. Measuring peak plasma concentrations of drugs absorbed
exclusively in the duodenum in both non-pregnant and pregnant volunteers, at different times of gestation, it was shown that peak absorption occurred at the same interval in all women with the exception those in labour. This suggests that gastric emptying is delayed only at the time of delivery.Слайд 15Hematological Changes in Pregnancy
Plasma volume increases early in pregnancy with
a 50% increase (and higher in higher order multiple pregnancies)
and a delayed increase in RBC mass and volume but less than the plasma volumeNormal pregnancy associated with a “demand” of 1000 milligrams of additional iron
500 mg. to increase maternal RBC volume
300 mg. tranpsorted to fetus
200 mg. for normal iron loss
60 mg. of elemental iron required daily, provided in 300 mg. of ferrous sulfate
Serum iron decreased
Transferrin and TIBC are increased
Слайд 16More Hematological Changes Occurring During Pregnancy
Pregnancy considered a “hypercoagulable state”
Fibrinogen
increases to 450-600 mg/dl
Factors VII, VIII, IX and X increase
Prothrombin,
Factor V, and XII are unchangedBleeding time does not change
Platelet count may increase to 450,000 to 600,000
WBC count may increase to as high as 20,000 due to an increase in granulocytes
Слайд 17Pulmonary Adaptations
Anatomical
Increased chest diameter, subcostal angle changes, increased diaphragmatic excursion
with diaphragm elevated as well
Physiological
Hyperventilation, Increased IC,VC and Minute
Volume, Residual volume decreased, Expiratory Reserve Volume decreased Tidal volume increased by 40%, pO2 increased, pCO2 decreased, arterial pH unchanged, and serum bicarbonate reduced Слайд 18Ventilation and Respiratory Gases.
A progressive increase in minute ventilation starts
soon after conception and peaks at 50% above normal levels
around the second trimester. This increase is effected by a 40% rise in tidal volume and a 15% rise in respiratory rate (2-3 breaths/minute). Since dead space remains unchanged, alveolar ventilation is about 70% higher at the end of gestation.Слайд 19Ventilation and Respiratory Gases.
Arterial and alveolar carbon dioxide tensions are
decreased by the increased ventilation. An average PaCO2 of 32 mmHg
(4.3 kPa) and arterial oxygen tension of 105 mmHg (13.7 kPa) persist during most of gestation. The development of alkalosis is forestalled by compensatory decreases in serum bicarbonate. Only carbon dioxide tensions below 28 mmHg (3.73 kPa) will lead to a respiratory alkalosis.Слайд 20Ventilation and Respiratory Gases
Oxygen consumption increases gradually in response to
the needs of the growing fetus, culminating in a rise
of at least 20% at term. During labour, oxygen consumption is further increased (up to and over 60%) as a result of the exaggerated cardiac and respiratory work load.Слайд 21Cardiac Changes in Pregnancy
Cardiac output increases around 50% from an
increase in HR and SV (3L/min to 6.2L/min)
There is an
additional 40% increase above that level during active laborImmediately following delivery, cardiac output may be increased by an additional 10-20%
Cardiac exam is different during pregnancy
Many patients will have an S3 after midpregnancy
Diastolic murmurs are usually considered serious
Systolic murmurs (“flow murmurs”) common
Displacment of heart is to right and upwards
EKG shows left axis deviation and low voltage QRS complexes
Слайд 23Blood Volume
Blood Volume increases progressively from 6-8 weeks gestation (pregnancy)
and reaches a maximum at approximately 32-34 weeks with little
change thereafter. Most of the added volume of blood is accounted for by an increased capacity of the uterine, breast, renal, striated muscle and cutaneous vascular systems, with no evidence of circulatory overload in the healthy pregnant woman. The increase in plasma volume (40-50%) is relatively greater than that of red cell mass (20-30%) resulting in hemodilution and a decrease in haemoglobin concentration. Intake of supplemental iron and folic acid is necessary to restore hemoglobin levels to normal (12 g/dl).Слайд 24Blood Volume
The increased blood volume serves two purposes. First, it
facilitates maternal and fetal exchanges of respiratory gases, nutrients and
metabolites. Second, it reduces the impact of maternal blood loss at delivery. Typical losses of 300-500 ml for vaginal births and 750-1000 ml for Caesarean sections are thus compensated with the so-called "autotransfusion" of blood from the contracting uterusСлайд 25Blood Constituents.
As mentioned above, red cell mass is increased 20-30%.
Leukocyte counts are variable during gestation, but usually remain within
the upper limits of normal. Marked elevations, however, develop during and after parturition (delivery). Fibrinogen, as well as total body and plasma levels of factors VII, X and XII increase markedly. The number of platelets also rises, yet not above the upper limits of normal. Combined with a decrease in fibrinolytic activity, these changes tend to prevent excessive bleeding at delivery. Thus, pregnancy is a relatively hypercoagulable state, but during pregnancy neither clotting or bleeding times are abnormalСлайд 26Cardiac Output
Cardiac Output increases to a similar degree as the
blood volume. During the first trimester cardiac output is 30-40%
higher than in the non-pregnant state. Steady rises are shown on Doppler echocardiography, from an average of 6.7 litres/minute at 8-11 weeks to about 8.7 litres/minute flow at 36-39 weeks; they are due, primarily, to an increase in stroke volume (35%) and, to a lesser extent, to a more rapid heart rate (15%). There is a steady reduction in systemic vascular resistance (SVR) which contributes towards the hyperdynamic circulation observed in pregnancy.During labor, further increases are seen with pain in response to increased catecholamine secretion; this increase can be blunted with the institution of labour analgesia. Also during labour, there is an increase in intravascular volume by 300-500 ml of blood from the contracting uterus to the venous system. Following delivery this autotransfusion compensates for the blood losses and tends to further increase cardiac output by 50% of pre-delivery values. At this point, stroke volume is increased while heart rate is slowed.
Слайд 27Cardiac Output
During labor, further increases are seen with pain in
response to increased catecholamine secretion; this increase can be blunted
with the institution of labour analgesia. Also during labour, there is an increase in intravascular volume by 300-500 ml of blood from the contracting uterus to the venous system. Following delivery this autotransfusion compensates for the blood losses and tends to further increase cardiac output by 50% of pre-delivery values. At this point, stroke volume is increased while heart rate is slowed.Слайд 28Cardiac Size/Position/ECG.
There are both size and position changes which can
lead to changes in ECG appearance. The heart is enlarged
by both chamber dilation and hypertrophy. Dilation across the tricuspid valve can initiate mild regurgitant flow causing a normal grade I or II systolic murmur. Upward displacement of the diaphragm by the enlarging uterus causes the heart to shift to the left and anteriorly, so that the apex beat is moved outward and upward. These changes lead to common ECG findings of left axis deviation, sagging ST segments and frequently inversion or flattening of the T-wave in lead III.Слайд 29Blood Pressure
. Systemic arterial pressure is never increased during normal
gestation. In fact, by midpregnancy, a slight decrease in diastolic
pressure can be recognized. Pulmonary arterial pressure also maintains a constant level. However, vascular tone is more dependent upon sympathetic control than in the nonpregnant state, so that hypotension develops more readily and more markedly consequent to sympathetic blockade following spinal or extradural anaesthesia. Central venous and brachial venous pressures remain unchanged during pregnancy, but femoral venous pressure is progressively increased due to mechanical factors.Слайд 30Renal Changes in Pregnancy
Minimal renal enlargement, bilaterally
Both renal pelvises and
ureters are dilated (“hydronephrosis of pregnancy”)
Greater urinary stasis, ureteral compression,
leading to urinary stasis and possilbe urinary tract infections, pyelonephritisLoss of urinary control
Bladder capacity diminished
RPF increases to 75% of non-pregnant value
Слайд 31More Renal Changes in Pregnancy
GFR increases 50% over on-pregnant state
Creatinine
clearance increases to 150-200 ml/min
Plasma osmolality decreases
Urine output is unchanged
There
is an increased sensitivity to renin and angiotensinRenal glycosuria common
Proteinuria up to 300 mg/24 hours normal
Слайд 32Endocrine Changes with Pregnancy
Carbohydrate Metabolism
Overall effect is that pregnancy is
diabetogenic
First half: tendency to hypoglycemia
Second half: tendency to hyperglycemia
Progressive insulin
resistance as pregnancy progressesProgesterone
Estrogen
HPL
“Typical” FBS less than in non-pregnant state
Blunting response to meals, eating as pregnancy progresses
Hypertrophy of beta cells as well
Слайд 33Metabolism
All metabolic functions are increased during pregnancy to provide for
the demands of fetus, placenta and uterus as well as
for the gravida's increased basal metabolic rate and oxygen consumption. Protein metabolism is enhanced to supply substrate for maternal and fetal growth. Fat metabolism increases as evidenced by elevation in all lipid fractions in the blood.Слайд 34Metabolism
Carbohydrate metabolism, however, demonstrates the most dramatic changes. Metabolically speaking,
pregnant women live in a state of "accelerated starvation." First,
nutritional demands of the growing fetus are met by the intake of glucose and, second, secretion of insulin in response to glucose is augmented. As early as 15 weeks of gestation, maternal blood glucose levels after an overnight fast are considerably lower than in the nongravid state.Слайд 35Hypoglycaemia.
Optimal blood glucose levels in pregnant women range between 4.4
to 5.5 mmol/1. In healthy non-pregnant individuals, signs of hypoglycaemia usually
begin when the blood glucose level declines to approximately 2.2 mmol/1 (40mg/dl); in pregnant women, however, hypoglycaemia is defined as a concentration below 3.3 mmol/1 (60mg/dl).Слайд 36Hypoglycaemia.
Hypoglycaemia initiates the release of glucagon, cortisol and, importantly, catecholamines.
In the anaesthetised state, however, these compensatory mechanisms, particularly the
release of epinephrine (adrenaline), are blocked. Autonomic derangements in the form of hypotension and tachycardia tend to ensue during high regional blockade or deep general anaesthesia, which may mask the symptoms and signs of hypoglycaemiaСлайд 37Endocrine Changes in Pregnancy
Thyroid Function in Pregnancy
The normal pregnant
woman remains euthyroid while pregnant despite/ with hormonal changes which
occurEstrogen production increases
Increased TBG
Increased total thyroxine, and T3
Free T4 and T3 remain unchanged
BMR increases 15-20% above normal
There is lowered T3 uptake during pregnancy
TSH does not cross the placenta
Слайд 38 Endocrine Changes in Pregnancy
GnRH concentration increases during pregnancy, but
the physiological significance of this change has not been determined
corticotropin-releasing hormone (CRH) is expressed by placental and chorionic trophoblasts, amnion, and decidual cells . Its concentration in maternal circulation is high and rises exponentially throughout pregnancy
Endocrine Changes in Pregnancy












































![Звуки [х], [ х′ ].
Позначення їх
буквами Х, х ( ха](/img/thumbs/35dbf8338bb9957e36032e16906181a0-800x.jpg)
















